Radiation therapy: Clinical application of volumetric modulated arc therapy
Images
The development of intensity-modulated radiotherapy (IMRT) has greatly advanced the field of radiation oncology since its introduction to the clinic in 1990s.1 Since then, IMRT has been widely used to treat different types of cancers. IMRT is capable of modulating the intensity of the radiation fields such that the tumor is adequately covered while the dose to healthy tissue is minimized. Two techniques are used to deliver IMRT. One is static gantry IMRT, which is composed of 5 to 11 radiation beams. For each beam, a multi-leaf collimator (MLC) is used to modulate the beam intensity in a dynamic sweeping manner (sliding window or SW) or in a step-and-shoot (SS) manner. The other technique delivers IMRT while the gantry is rotating. In 1993, Mackie et al developed a rotating fan-beam technique using a dedicated helical tomotherapy system.2 In 1995, Yu proposed the linac-based rotating cone-beam technique, and coined this technique intensity-modulated arc therapy (IMAT) as an alternative to tomotherapy.3 In the original design of IMAT, several arcs were required to achieve intensity modulation.
One key feature of IMRT is inverse planning, where computational optimization algorithms are utilized to design the motion trajectories or segment shapes of the MLC to achieve intensity modulation. Depending on the planning technique, the MLC patterns can be directly outputted by the optimization algorithm, or be converted from the optimized fluence map with a leaf-sequencing algorithm. Different planning systems and optimization algorithms have been developed for static gantry IMRT. At that time, an efficient planning method for IMATwas not available, yet much research has since been devoted to developing optimization algorithms for IMAT.4 In 2008, Otto designed an optimization algorithm to deliver IMAT in a single-arc manner, which he called volumetric-modulated arc therapy (VMAT).5 In VMAT delivery, both dose rate and gantry rotation speed can vary. These additional degrees-of-freedom increased the capability of beam intensity modulation.
Based upon Otto’s VMAT algorithm, Varian (Palo Alto, CA) implemented the single-arc form of IMAT and named the system RapidArcTM. Elekta (Stockholm, Sweden) and Philips (Amsterdam, The Netherlands) also released their rotational IMRT solutions, VMATTM and Smart-ArcTM respectively. Since the clinical implementation of these different single-arc forms of IMAT by different vendors, the feasibility of applying this novel delivery technique to different cancer sites has been explored. Comparisons between VMAT, 3-dimensional (3D) conformal therapy, conventional static gantry IMRT, and helical tomotherapy have been extensively studied to better understand the differences among different techniques.
Theoretical investigations6,7 and treatment planning studies compared different intensity-modulation techniques. This article reviews clinical applications of VMAT technology in treating tumors of the central nervous system, head and neck, lung, liver, prostate, and other sites, and discusses advantages and limitations of VMAT.
Clinical applications of VMAT
Brain cancers
VMAT has been used to treat primary brain tumors and metastases. Davidson et al8 compared VMAT and standard IMRT to treat gliomas, specifically with respect to the dosimetric impact of adding one partial arc to one full arc for VMAT planning. The researchers observed improved spinal cord sparing and reduced integral dose with the use of an additional coplanar partial arc and concluded that VMAToffers faster treatment than IMRT, with similar dosimetric qualities.
Clark et al9 reported the feasibility of using VMAT stereotactic radiosurgery (SRS) to treat multiple brain metastases. For each patient,3 VMAT plans were designed—single-arc/single isocenter, triple-arc/single isocenter, and triple-arc/triple-isocenter—to deliver 20 Gy prescription dose to all lesions. They found that the single isocenter VMAT plan has similar conformity as multiple isocenter plans with< ½ beam-on time. Multiple isocenter plan was recommended for closely spaced targets.
Hsu et al10 investigated the feasibility of using VMAT to treat whole brain with hippocampal avoidance and a simultaneous integrated boost for 1 to 3 brain metastases. They showed that VMAT achieved adequate whole-brain coverage with conformal hippocampal avoidance and radiosurgical quality dose distribution for 1 to 3 brain metastases. The mean delivery time was 3.6 min. Awad et al11 shared their experience of whole-brain radiotherapy with hippocampal avoidance and a simultaneous integrated boost to achieve stereotactic radiotherapy (SRS) for melanoma brain metastases. The treatment was well tolerated, with only one patient among 26 having grade 4 late toxicity.They concluded that VMAT provided safe treatment with survival times similar to conventional SRS.
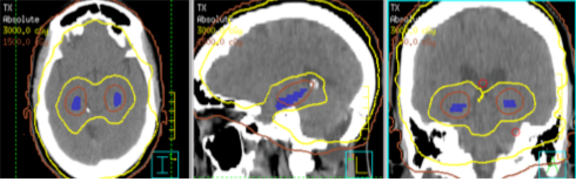
In our clinic, VMAT was also utilized to treat whole brain with hippocampal avoidance. Figure 1 shows the dose distribution of a representative VMAT plan.
Spinal tumors
VMAT has been used to treat both primary paraspinal tumors and spinal metastases. The geometric relationship between the target volume and the spinal cord brings challenges to treatment planning. Bedford et al12 reported a case study where VMAT was used to treat a para-spinal tumor. A highly conformal dose distribution while sparing spinal cord was achieved using VMAT and the delivery time was 2 min15 sec. Lee et al13 compared a single arc VMAT with 7-field IMRT to deliver a concomitant hypofractionated treatment to spine metastases with simultaneous integrated boost. They found that target coverage was similar for IMRT and VMAT plans; however, a higher dose to the regions around the spinal cord was observed in VMAT plans of unclear clinical significance. The mean delivery time of VMAT plans was one third that of IMRT plans. Wu et al14 evaluated the feasibility of using VMAT for spine stereotactic body radiotherapy (SBRT) to achieve highly conformal dose distributions while sparing the spinal cord. They found that single-arc VMAT could not achieve spinal cord sparing comparable to IMRT, whereas two-arc VMAT could. The monitor units (MUs) and treatment time were significantly reduced (> 50%) in the two-arc VMAT plan compared to the IMRT plan. No significant difference in integral dose was observed.
Navarria et al15 assessed the clinical outcomes (acute toxicity, local control, and survival) for re-irradiating patients with spinal metastases with VMAT. Thirty-one patients were included in their study; 93% obtained clinical pain remission, and 73% showed neurological improvement. No acute or late toxicities were observed and no recurrence occurred. Median survival was 10 months (range 6-24 months).
Head and neck cancer
IMRT is the standard technique used to treat head and neck cancers to spare several organs at risk (OAR) surrounding the tumor volume.Bertelsen et al16 replanned 25 oropharyngeal or hypopharyngeal carcinoma cases treated with IMRT using one single-arc VMAT. Similar or better target coverage and OAR sparing were observed with the VMAT plans compared to clinically used step-shoot IMRT plans. The MUs and treatment time were reduced by 8.5% and 35%, respectively, in VMAT delivery compared to IMRT. Johnson et al17 compared VMAT andIMRT plans using a simultaneous integrated boost for head and neck cancer. Similar plan quality in terms of target coverage and OAR sparing were achieved by VMAT; however, the MUs of VMAT plans were reduced to one-third that of IMRT plans. Comparisons between VMATand serial tomotherapy for head and neck cancer were also conducted by several authors.18,19 In general, tomotherapy provides equivalent dose distribution or better conformity index, but longer delivery time, than VMAT. Neubauer et al20 assessed the shoulder position variation and its impact on dose in VMAT and IMRT plans for head and neck cancer. The shoulder motion averaged 2 mm to 5 mm in each direction and causedD99 (minimal dose to 99% of the volume) of the clinical target volume (CTV) to decrease by 1.01 Gy and dose to the brachial plexus to increase by 0.72 Gy. IMRT plans were more sensitive to posterior shifts than VMAT plans. Oliver et al21 evaluated the tradeoffs in planning and treating locally advanced head and neck cancer with IMRT and VMAT techniques. Based on 15 patients in their study, the main tradeoffs betweenIMRT and VMAT were shorter treatment times, but longer planning times, for VMAT.
Lung cancer
Conventional fractionated radiotherapy and SBRT for lung cancer can both be delivered using VMAT techniques. Bedford et al22 reported using VMAT to deliver 50 Gy in 25 fractions for lung cancer. An in-house planning system was used to generate VMAT plans that were compared to conventional 3-field 3D conformal plans. The authors found that VMAT improved the efficiency of delivery. VMAT has also been used to treat early-stage nonsmall cell lung cancer (NSCLC).23,24 In a study by Brock et al, comparisons between VMAT plans with the best 3D conformal plans with coplanar and noncoplanar 3-, 5-, 7-, and 9-beams showed that VMAT had equivalent V20 oflungs and target coverage, but much faster delivery time. However, in another study by McGrath et al24 that compared VMAT to 3D conformal plans, an improved V5, V10, V12.5, and V20 of lungs in the VMAT plan were observed. This difference was due to the partial arcs used in McGrath study to avoid the contralateral lung.
Recently, SBRT has emerged as an efficacious treatment for medically inoperable NSCLC with excellent control rates and acceptable toxicity.25-27 VMAT has also been used to deliver SBRT treatment of lung cancer. Holt et al compared VMAT plans with coplanar and non-coplanar IMRT plans for lung SBRT prescribed to 54 Gy in 3 fractions.28 Plan quality was evaluated using the RTOG 0236 criteria. They concluded that VMAT achieved similar plan quality as noncoplanar IMRT and better quality than coplanar IMRT. In addition, the delivery time could be reduced by 70% with VMAT.
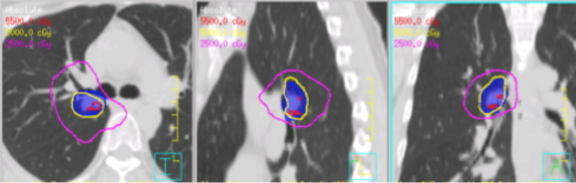
Tumor motion in lung-cancer treatment is a concern with VMAT and IMRT techniques due to the interplay between tumor motion during the respiratory cycle and the movement of the MLC leaves.29 Active breathing coordination (Elekta, Stockholm, Sweden) may be used to manage tumor motion by temporarily suspending patient breath. In our clinic, VMAT combined with active breathing control were used to deliver SBRT treatment for NSCLC. Figure 2 shows the dose distributions for a representative case with a prescription of 50 Gy in 5 fractions.
Abdominal cancer
Scorsetti et al conducted a feasibility study using VMAT for SBRT for abdominal targets, including primary or metastatic liver tumor,pancreatic cancer, and nodal metastasis in the retroperitoneum.30 They found that the planning objective on targets and OARs were met inmost cases. Delivery time ranged from 2.8 to 9.2 minutes on average. Good early clinical results in terms of local control and toxicity were observed at 6 months after treatment. Local control at 6 months was achieved in 19 patients with a crude rate of 79.2% (assessed in 24 of 37 patients).
Gong et al31 reported their experience in treating hepatocellular carcinoma with VMAT combined with the use of an active-breathing coordination device. Compared to conventional IMRT, the VMAT plan achieved more conformal and homogeneous dose in the PTV while the V5 and V10 of the liver was higher. The average treatment time of using the VMAT plan was 2 min 10 sec, which was comparable to the3D conformal radiotherapy and significantly reduced compared to IMRT plans (average of 10 min 26 sec).
Prostate cancer
Treatment for prostate cancer offers an ideal geometry for application of VMAT technique. Palma et al32 compared VMAT with IMRTand 3D-conformal plans for treatment of localized prostate cancer in terms of dose to OARs, equivalent uniform dose, dose homogeneity and conformity, and MUs. They concluded that both IMRT and VMAT resulted in lower dose to normal structures than 3D conformal therapy. Variable-dose rate VMAT provided best sparing of OAR. VMAT plans required less MUs (~40%) than IMRT plans. Yoo et al33 compared VMAT to IMRT for prostate cancer involving seminal vesicles and lymph nodes. They found that IMRT better spared OARs for lymph nodes-positive cancer. VMAT plans with two arcs achieved similar dose distributions to IMRT plans if only prostate and seminal vesicles were involved. Wolff et al34 compared VMAT, tomotherapy, step-shoot IMRT, and 3D-conformal therapy for treating prostate cancer. VMAT, tomotherapy, and IMRT offered better plan quality compared to 3D-conformal treatments. Tomotherapy provided the bestOAR sparing and VMAT was the most efficient treatment option. Pardo-Montero et al35 performed a methodological comparison between tomotherapy-like and VMAT-like techniques for prostate cancer. They found that the quality of tomotherapy-like plans depended on the fan-beam width and pitch used to deliver treatment. With 1 cm fan-beam width, tomotherapy-like plans achieved slightly better quality thanVMAT-like plans. However, with 2.5 cm fan-beam width, the dosimetric advantage was lost.
Myrehaug et al36 investigated the acute toxicity of VMAT and IMRT for hypofractionated high-risk prostate cancer radiotherapy. They found that VMAT planning with 2 or 3 arcs were necessary to achieve adequate dosimetric quality. They found a higher integral dose without consistent dosimetric benefits for VMAT plans. Consistent with other studies, the treatment times were reduced.
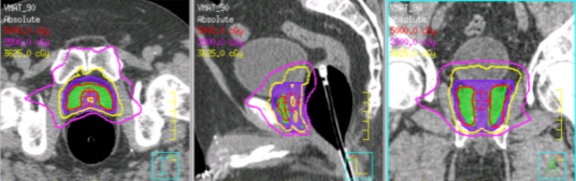
Using VMAT to treat localized prostate with SBRT in 5 fractions to a total dose of 36.25 Gy was also implemented in our clinic. A rectal balloon was inserted to minimize the intra-fraction prostate motion. Figure 3 shows the dose distribution for one representative case.
Other tumors
VMAT technique has also been implemented for other cancers and treatments, such as total-marrow irradiation (TMI),37-40 pancreatic malignancies,41 and breast cancer.42-44 Improved delivery efficiency (fewer MU and shorter treatment times) with VMAT was a common finding from these studies. This advantage is particularly important for pediatric patients for whom the risk of secondary cancer in long-term survivors is a concern. Shaffer et al conducted a planning study to compare VMAT, IMRT, 3D conformal therapy, and parallel opposed (POP) beams in the treatment of pediatric retroperitoneal tumors.45 They found that VMAT was dosimetrically similar to IMRT and offers a reduction of treatment time by 50%. POP beams resulted in the fastest delivery and the worst dosimetry quality.
Conclusion
VMAT can generate treatment plans with similar planning target volume coverage as conventional IMRT, 3D conformal therapy, and tomotherapy. However, the plan quality differences regarding OAR sparing, integral dose, and low dose to normal tissue between VMAT and other conventional techniques were controversial among the different studies reviewed. This difference is partially due to the number of arcs used inVMAT plan and the number of beams used for IMRT/3D conformal therapy. For instance, the use of partial arcs in VMAT plans resulted in lower integral dose for brain tumors8 and reduced low-dose to normal lung for lung tumors.24 In general, VMAT plans with two arcs can achieve better dosimetric quality than single-arc VMAT.
All the studies reviewed have shown that VMAT improves efficiency of delivery with reduced MU and delivery time compared to conventional IMRT. The lower MU in VMAT delivery may potentially reduce the risk of radiation-induced cancers, which needs to be validated by long-term studies. Few studies have reported on the toxicity and clinical outcomes of VMAT compared to IMRT. In general,VMAT is a safe and efficient treatment modality for various cancer types. However, longer treatment planning time for VMAT is needed due to the complicated optimization process and dose calculation.
References
- Palta J, Mackie TR. Intensity-modulated radiation therapy: The State of the Art. American Association of Physicists in Medicine 2003 Summer School Proceedings. 2003, Colorado College, Colorado Springs, CO.
- Mackie TR, Holmes T, Swerdloff S, et al. Tomotherapy: A new concept for the delivery of dynamic conformal radiotherapy. Med Phys. 1993;20:1709-1719.
- Yu CX. Intensity-modulated arc therapy with dynamic multileaf collimation: An alternative to tomotherapy. Phys Med Biol. 1995;40:1435-1449.
- Yu CX, Tang G. Intensity-modulated arc therapy: Principles, technologies and clinical implementation. Phys Med Biol. 2011;56:R31-54.
- Otto K. Volumetric modulated arc therapy: IMRT in a single gantry arc. Med Phys. 2008;35:310-317.
- Bortfeld T, Webb S. Single-Arc IMRT? Phys Med Biol. 2009;54:N9-20.
- Bortfeld T. The number of beams in IMRT—theoretical investigations and implications for single-arc IMRT. Phys Med Biol. 2010;55:83-97.
- Davidson MT, Masucci GL, Follwell M, et al. Single arc volumetric modulated arc therapy for complex brain gliomas: Is there an advantage as compared to intensity modulated radiotherapy or by adding a partial arc? Technol Cancer Res Treat. 2012;11:211-220.
- Clark GM, Popple RA, Young PE, et al. Feasibility of single-isocenter volumetric modulated arc radiosurgery for treatment of multiple brain metastases. Int J Radiat Oncol Biol Phys. 2010;76:296-302.
- Hsu F, et al. Whole brain radiotherapy with hippocampal avoidance and simultaneous integrated boost for 1-3 brain metastases: A feasibility study using volumetric modulated arc therapy. Int J Radiat Oncol Biol Phys. 2010;76:1480-1485.
- Awad R, Fogarty G, Hong A, et al. Hippocampal avoidance with volumetric modulated arc therapy in melanoma brain metastases -the first Australian experience. Radiat Oncol. 2013;8:62.
- Bedford JL, Convery HM, Hansen VN, Saran FH. Paraspinal volumetric modulated arc therapy. Br J Radiol. 2012;85:1128-1133.
- Lee YK, Bedford JL, McNair HA, Hawkins MA. Comparison of deliverable IMRT and VMAT for spine metastases using a simultaneous integrated boost. Br J Radiol. 2013;86:20120466.
- Wu QJ, Yoo S, Kirkpatrick JP, et al. Volumetric arc intensity-modulated therapy for spine body radiotherapy: Comparison with static intensity-modulated treatment. Int J Radiat Oncol Biol Phys. 2009;75:1596-1604.
- Navarria P, Mancosu P, Alongi F, et al. Vertebral metastases reirradiation with volumetric-modulated arc radiotherapy. Radiother Oncol. 2012;102:416-420.
- Bertelsen A, Hansen CR, Johansen J, Brink C, et al. Single arc volumetric modulated arc therapy of head and neck cancer. Radiother Oncol. 2010;95:142-148.
- Johnston M, Clifford S, Bromley R, et al. Volumetric-modulated arc therapy in head and neck radiotherapy: A planning comparison using simultaneous integrated boost for nasopharynx and oropharynx carcinoma. Clin Oncol (R Coll Radiol). 2011;23:503-511.
- Stieler F, Wolff D, Schmid H, et al. A comparison of several modulated radiotherapy techniques for head and neck cancer and dosimetric validation of VMAT. Radiother Oncol. 2011;101:388-393.
- Lu SH, Cheng JC, Kuo SH, et al. Volumetric modulated arc therapy for nasopharyngeal carcinoma: A dosimetric comparison with TomoTherapy and step-and-shoot IMRT. Radiother Oncol. 2012;104:324-330.
- Neubauer E, Dong L, Followill DS, et al. Assessment of shoulder position variation and its impact on IMRT and VMAT doses for head and neck cancer. Radiat Oncol. 2012;7:19.
- Oliver M, McConnell D, Romani M, et al. Evaluation of the trade-offs encountered in planning and treating locally advanced head and neck cancer: intensity-modulated radiation therapy vs dual-arc volumetric-modulated arc therapy. Br J Radiol. 2012;85:1539-1545.
- Bedford JL, Nordmark Hansen V, McNair HA, et al. Treatment of lung cancer using volumetric modulated arc therapy and image guidance: a case study. Acta Oncol. 2008;47:1438-1443.
- Brock J, Bedford J, Partridge M, et al. Optimising stereotactic body radiotherapy for non-small cell lung cancer with volumetric intensity-modulated arc therapy—a planning study. Clin Oncol (R Coll Radiol). 2012;24:68-75.
- McGrath SD, Matuszak MM, Yan D, et al. Volumetric modulated arc therapy for delivery of hypofractionated stereotactic lung radiotherapy: A dosimetric and treatment efficiency analysis. Radiother Oncol. 2010;95:153-157.
- Timmerman R, Paulus R, Galvin J, et al. Stereotactic body radiation therapy for inoperable early stage lung cancer. JAMA. 2010;303:1070-1076.
- Videtic GM, Stephans K, Reddy C, et al. Intensity-modulated radiotherapy-based stereotactic body radiotherapy for medically inoperable early-stage lung cancer: excellent local control. Int J Radiat Oncol Biol Phys. 2010;77:344-3449.
- Stephans KL, Djemil T, Reddy CA, et al. A comparison of two stereotactic body radiation fractionation schedules for medically inoperable stage I non-small cell lung cancer:The Cleveland Clinic experience. J Thorac Oncol. 2009;4:976-82.
- Holt A, van Vliet-Vroegindeweij C, Mans A, et al. Volumetric-modulated arc therapy for stereotactic body radiotherapy of lung tumors: a comparison with intensity-modulated radiotherapy techniques. Int J Radiat Oncol Biol Phys. 2011;81:1560-1567.
- Bortfeld T, Jokivarsi K, Goitein M, et al. Effects of intra-fraction motion on IMRT dose delivery: Statistical analysis and simulation. Phys Med Biol. 2002;47:2203-2220.
- Scorsetti M, Biegnardi M, Alongi F, et al. Stereotactic body radiation therapy for abdominal targets using volumetric intensity modulated arc therapy with RapidArc: Feasibility and clinical preliminary results. Acta Oncol. 2011;50:528-538.
- Gong GZ, Yin Y, Xing LG, et al. RapidArc combined with the active breathing coordinator provides an effective and accurate approach for the radiotherapy of hepatocellular carcinoma. Strahlenther Onkol. 2012;188:262-268.
- Palma D, Vollans E, James K, et al. Volumetric modulated arc therapy for delivery of prostate radiotherapy: Comparison with intensity-modulated radiotherapy and three-dimensional conformal radiotherapy. Int J Radiat Oncol Biol Phys. 2008;72:996-1001.
- Yoo S, Wu QJ, Lee WR, Yin FF. Radiotherapy treatment plans with RapidArc for prostate cancer involving seminal vesicles and lymph nodes. Int J Radiat Oncol Biol Phys. 2010;76:935-942.
- Wolff D, Stieler F, Welzel G, et al. Volumetric modulated arc therapy (VMAT) vs. serial tomotherapy, step-and-shoot IMRT and 3D-conformal RT for treatment of prostate cancer. Radiother Oncol. 2009;93:226-233.
- Pardo-Montero J, Fenwick JD,.Tomotherapy-like versus VMAT-like treatments: A multicriteria comparison for a prostate geometry. Med Phys. 2012;39:7418-7429.
- Myrehaug S, Chan G, Craig T, et al. A treatment planning and acute toxicity comparison of two pelvic nodal volume delineation techniques and delivery comparison of intensity-modulated radiotherapy versus volumetric modulated arc therapy for hypofractionated high-risk prostate cancer radiotherapy. Int J Radiat Oncol Biol Phys. 2012;82:e657-62.
- Aydogan B, Yeginer M, Kavak GO, et al. Total marrow irradiation with RapidArc volumetric arc therapy. Int J Radiat Oncol Biol Phys. 2011;81:592-599.
- Han C, Schultheisss TE, Wong JY. Dosimetric study of volumetric modulated arc therapy fields for total marrow irradiation. Radiother Oncol. 2012;102:315-320.
- Mancosu P, Navarria P, Castagna L, et al. Anatomy driven optimization strategy for total marrow irradiation with a volumetric modulated arc therapy technique. J Appl Clin Med Phys.. 2012; 13:3653.
- Surucu M, Yeginer M, Kavak GO, et al. Verification of dose distribution for volumetric modulated arc therapy total marrow irradiation in a humanlike phantom. Med Phys. 2012;39:281-288.
- Ali AN, Dhabaan AH, Jarrio CS, et al. Dosimetric comparison of volumetric modulated arc therapy and intensity-modulated radiation therapy for pancreatic malignancies. Med Dosim. 2012;37:271-275.
- Pasler M, Georg D, Bartelt S, Lutterbach J. Node-positive left-sided breast cancer: Does VMAT improve treatment plan quality with respect to IMRT? Strahlenther Onkol.2013;189:380-386.
- Popescu CC, Olivotto IA, Beckham WA, et al. Volumetric modulated arc therapy improves dosimetry and reduces treatment time compared to conventional intensity-modulated radiotherapy for locoregional radiotherapy of left-sided breast cancer and internal mammary nodes. Int J Radiat Oncol Biol Phys. 2010;76:287-295.
- Qiu JJ, Chang Z, Wu QJ, et al. Impact of volumetric modulated arc therapy technique on treatment with partial breast irradiation. Int J Radiat Oncol Biol Phys. 2010;78:288-296.
- Shaffer R, Vollans E, Vellani R, et al. A radiotherapy planning study of RapidArc, intensity modulated radiotherapy, three-dimensional conformal radiotherapy, and parallel opposed beams in the treatment of pediatric retroperitoneal tumors. Pediatr Blood Cancer. 2011;56:16-23.