Concurrent management of low-risk prostate cancer and localized small lymphocytic lymphoma
Images
Prostate cancer (PC) is the most common non-cutaneous malignancy in the United States, with an anticipated incidence of 239,000 cases and 29,700 deaths in 2013.1 Since the advent of prostate-specific antigen (PSA) based screening, approximately 80% of PC cases are now detected because of an elevated PSA level. Although the detection of PC has increased considerably since the introduction of PSA-testing in1989, randomized screening studies have suggested that PSA screening can lead to both over-diagnosis and over-treatment.2 Moreover, after a median follow-up of 10 years, the Prostate Cancer Intervention versus Observation Trial demonstrated no differences in prostate-cancer specific mortality (PCSM) or all-cause mortality among men with low risk disease3 who were observed versus those treated with a radical prostatectomy (RP).4 However, given the association of increasing risk of high grade PC with advancing age and the higher likelihood of under-staging by biopsy given increasing prostate gland volume with advancing age, screening for PC in older men who are in excellent health and expected to live at least 10 years should be considered to rule out the possibility that a high-grade PC exists. If low-risk disease is confirmed (ie, PSA ≤10, Gleason score ≤6 and clinical tumor (T) category 1c or 2a), the options of active surveillance5 versus definitive treatment with either RP or dose-escalated RT6,7 should be discussed along with the potential side-effects of each treatment, with the expectation that PSA recurrence-free survival rates approximate 90% at 7 years following treatment.8
While PC is the most prevalent non-cutaneous solid malignancy in the United States, CLL/SLL represents the most common leukemia in the Western world, accounting for 30% of all leukemias.9 CLL/SLL is a chronic lymphoproliferative disorder, heralded by the monoclonal accumulation of mature, functionally-deficient B-lymphocytes. The majority of patients present with a lymphocytosis of >5000 B-lymphocytes/uL, diagnostic of CLL. A smaller number of patients present with lymphadenopathy caused by cells with an identical immunopheno type as CLL, but with <5,000 B-cells/uL in the peripheral blood, diagnostic of SLL. Patients with either SLL or CLL in the absence of splenomegaly or cytopenias are considered to have early stage disease. FISH can provide important prognostic information. Trisomy-12occurs in ~16% of patients and is generally a favorable indicator.10 The management of early stage SLL is dependent upon the presence of disease-related symptoms, threatened end-organ dysfunction or bulky disease. Close monitoring remains an option in the absence of these indications, although locoregional radiotherapy can be curative in early stage disease.11
CASE SUMMARY
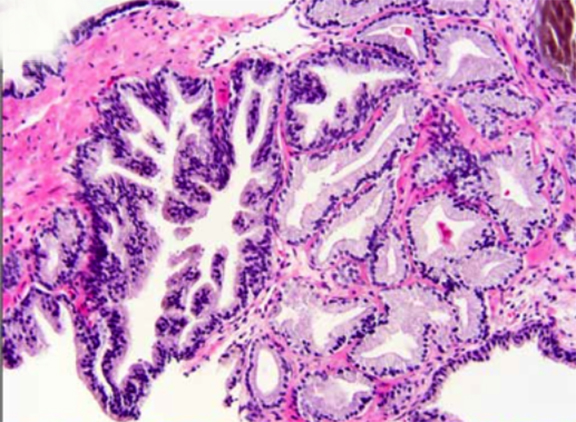
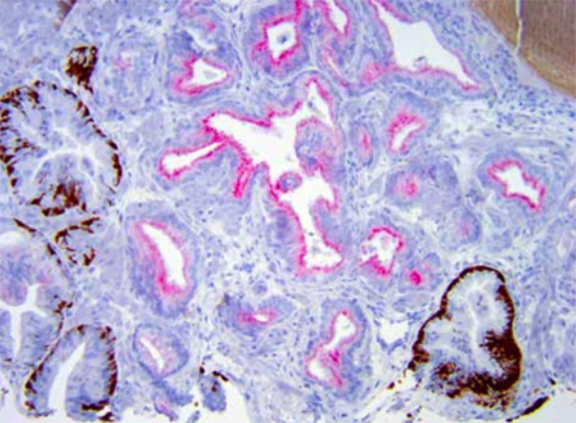
A 79-year-old male presented with a prostate-specific antigen (PSA) that rose from 2.5 to 7.2ng/mL over 22 years, prompting biopsies,which showed chronic prostatitis. In 2013, a digital rectal examination (DRE) demonstrated an enlarged prostate, and the PSA increased from7.2ng/mL to 9.2ng/mL over 14 months without confounders.12 This prompted rebiopsy of a prostate gland, which measured 148cc on transrectal ultrasound (PSA density = 0.06ng/mL/cc), revealing prostatic adenocarcinoma, Gleason score 3 + 3 = 6 in one of six right-sided prostate needle biopsy (PNB) cores involving <5% of the specimen; and Gleason score 3 + 3 = 6 in two of six left-sided PNB cores involving 10% and 15% of these cores (Figure 1). The remainder of the physical examination revealed no lymphadenopathy in Waldeyer’s ring or peripherally, and there was no splenomegaly. The history did not elicit any B symptoms or significant lower urinary tract symptoms.
IMAGING FINDINGS
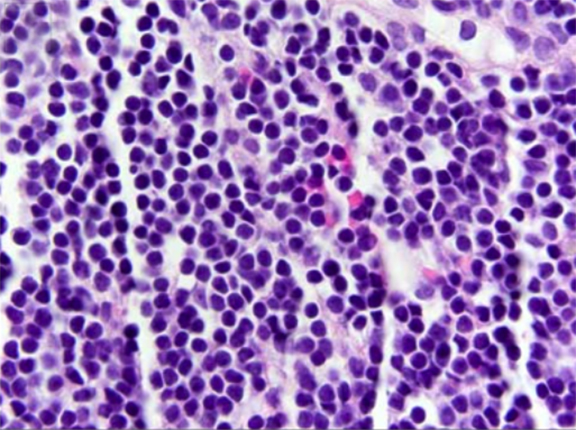
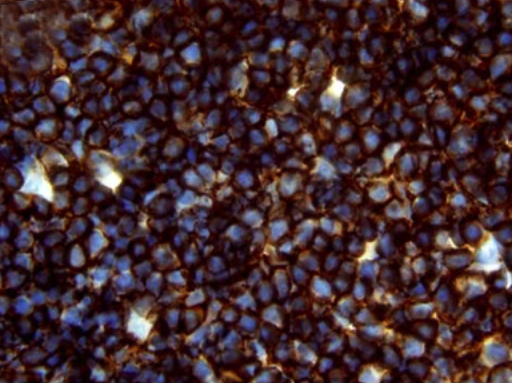
Given the rapid rise in PSA (PSA velocity = 1.7ng/mL/year), staging with an endorectal and pelvic MRI was obtained showing enlarged pelvic side-wall lymph nodes bilaterally. Percutaneous biopsy of a right-sided lymph node revealed an atypical lymphocytic population. By immunohistochemistry and flow cytometry, this population expressed B-cell markers CD19 and CD20, co-expressed CD5 and CD23,demonstrated monotypic expression of surface immunoglobulin lambda, and lacked cyclin D1 expression, consistent with the histologic diagnosis of chronic lymphocytic leukemia / small lymphocytic lymphoma (CLL/SLL) (Figure 1). Although the complete blood count was unremarkable, interphase fluorescence in situ hybridization (FISH) of peripheral blood showed trisomy 12 in 6% of cells, characteristic of CLL/SLL. CT of the chest, abdomen, and pelvis revealed no distant foci of disease.
The patient was otherwise in excellent health with a history of gastroesophageal reflux disease and hypercholesterolemia. His medications included atorvastatin, omeprazole, and tamsulosin.
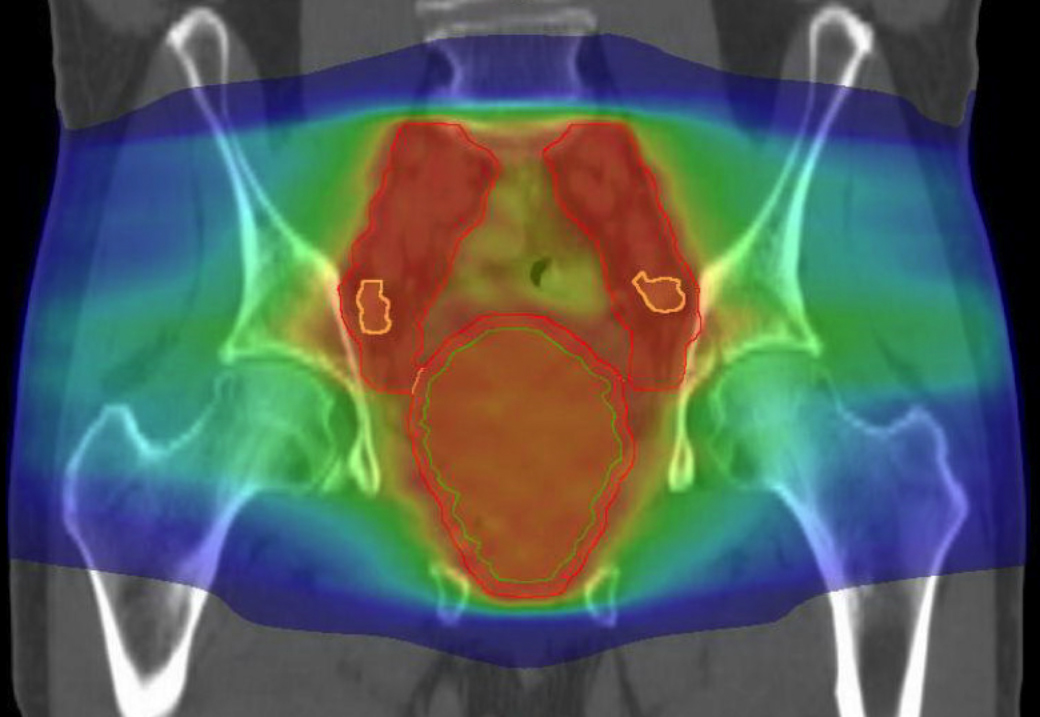
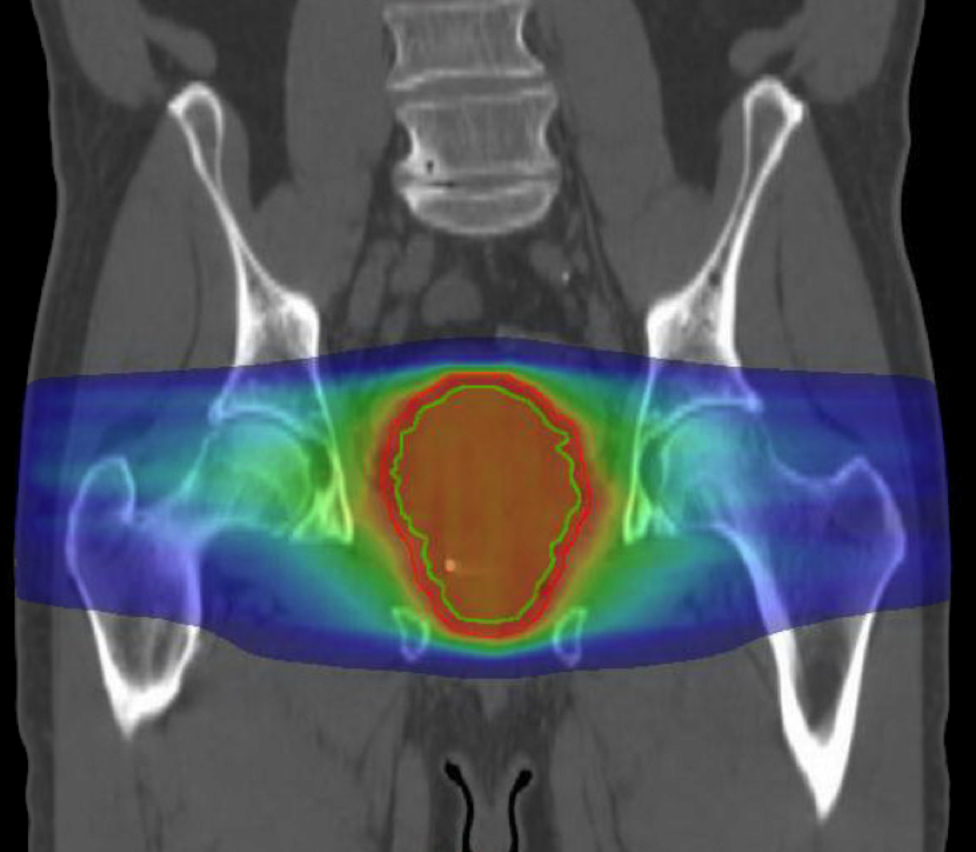
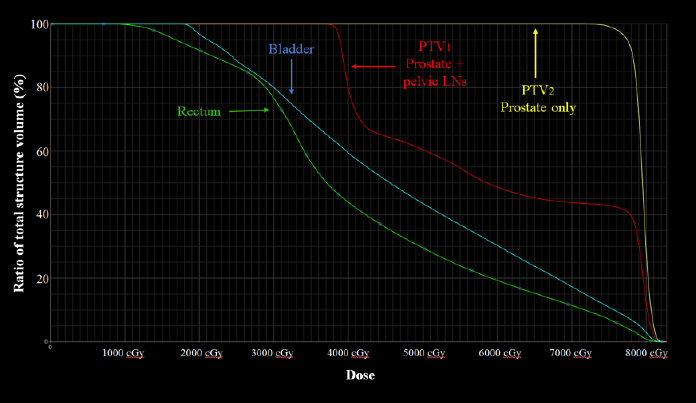
In the setting of anatomically-adjacent synchronous primary tumors, multidisciplinary discussion concluded that concurrent definitive treatment of both lesions was the optimal approach given the patient’s desire to undergo treatment rather than surveillance, and his excellent underlying health with a remaining life expectancy (RLE) exceeding 10 years (RLE = 8.62 years, based on social security administration tables. +50% based on clinical indicators to suggest top quartile of health). To that end, image-guided radiotherapy (IGRT) was employed to encompass the prostate along with the bilateral internal iliac lymph nodes to a dose of 3,960 cGy in 22 fractions (Figure 2). Upon reaching this curative dose for stage II SLL (highest local control rates for SLL are approached at ~40Gy), the treatment volume was reduced andan additional 3,600 cGy was delivered in 20 fractions to the prostate alone (Figure 2) for a total definitive dose of 7,560 cGy to the prostate gland (Figure 3). The patient completed definitive therapy without significant bowel or bladder toxicity. He did not report diarrhea, nausea,weight loss, or change in bowel habits. Tamsulosin was increased from 0.4 mg daily to 0.4 mg twice per day to manage increased nocturia attributed to radiation urethritis, although this resolved within 2 weeks following the completion of treatment, and after tamsulosin was discontinued.
DISCUSSION
Although patients with early-stage SLL are often observed, involved-field radiotherapy alone without systemic treatment may be pursued with curative intent. This approach is based on data extrapolated from the management of other indolent NHLs13 along with retrospective series showing the efficacy of radiation alone.14 In one such study, 54 patients with SLL were treated with variable regimens of chemotherapy and radiotherapy. Among 14 patients with early stage disease who received radiation without systemic treatment, 10-year freedom from recurrence (FFR) was 62% to 80%, demonstrating a prolonged endpoint and potential “cure” for the majority of these patients.15 Consensus recommendations for localized SLL include involved-site radiotherapy to a dose of 24 Gy to 30 Gy targeting the involved lymph nodes.14
The management of multiple primary cancers has long represented a clinical challenge with few data to guide therapy. Synchronous primary tumors have been described with varying frequency and are generally thought to arise from genetic predisposition (eg,Li-Fraumeni syndrome, BRCA1/2, etc.), environmental exposures (eg, tobacco, radiation, etc.), adverse treatment effects (eg, carcinogenic chemotherapy or radiotherapy), or combinations of these factors. Patients with CLL/SLL may be particularly susceptible to second malignancies, potentially due to impaired immune surveillance of tumor cells.16
After an assessment of competing risks, initial therapy is typically directed at the most life-threatening condition with the goal of prolonging disease free and overall survival while attempting to minimize the impact of therapy on quality of life. Typically, due to the cumulative toxicity of combining differing therapies for distinct cancers, the treatment approach necessitates focusing on one malignancy while delaying treatment for the other. Occasionally, however, synchronous tumors share common treatment strategies and are amenable to concurrent definitive therapy, as in this report. In addition, if the RLE is long in comparison to the natural history of symptomatic progression of the cancer, treatment should be offered. Therefore, given the absence of competing risks to shorten life expectancy in the case presented, and the favorable toxicity profile of treating the prostate and bilateral internal iliac lymph-nodal chains with IGRT (ie, 7% risk of acute Grade 2rectal or bladder toxicity, with no report of Grade 3 or higher toxicity17), unimodality treatment with IGRT was designed and implemented simultaneously for both cancers. Moreover, the anatomic proximity of the two cancers allowed for both to be encompassed within a single radiation treatment field. Evidence-based dose-constraints for the rectum were achieved, including a V75 of 7.5% and V70 of 11.5% (per guidelines V75 ≤15% and V70 ≤20%) [16]. The bladder had a V75 of 11% and V70 of 17.5% (per guidelines V75 ≤25% and V70 ≤ 5%).19 Similarly, the small bowel was not within the treatment field and a tolerance of V45 ≤195cc was achieved.20 The treatment was well tolerated without clinically-significant bowel or bladder toxicity.
The routine post-treatment monitoring for low-risk PC consists of a DRE and PSA testing every 6 months for 5 years and annually thereafter.21 The routine follow-up care for localized SLL includes follow-up at semi-annual visits for disease-related symptoms (fatigue, night sweats, unexplained weight loss, etc.) along with hematologic surveillance for leukocytosis, anemia, or thrombocytopenia.14
One challenge with post-therapy follow-up is that survivors of certain cancers may receive lower quality care for non-oncologic competing risks than matched controls without a prior cancer diagnosis.22 Specifically, survivors of PC were found to be less likely than controls to receive quality acute care for non-cancer-related illnesses (odds radio 0.75). While further studies are needed to determine why certain cancer survivors receive suboptimal care, there is clearly a need for greater vigilance when it comes to the health care of this population; otherwise, the benefit gained in cancer-specific survival via curative treatment may not translate into an overall survival benefit due to inter-current death from a neglected competing risk.
CONCLUSION
Thus, a case is presented of an elderly yet healthy man with synchronous cancers amenable to curative treatment with a single therapeutic modality and minimal risk of toxicity, affording ~60% chance of long-term cancer control. When selecting patients of advanced age for curative therapy of synchronous cancers where multiple treatments may be indicated, the patient’s wishes should be considered following appropriate education about the risks and benefits of treatment(s), discussion of competing risks and RLE, and review of appropriate follow-up care. These considerations should be aimed at maximizing cancer control while minimizing the impact of treatment on quality of life.
REFERENCES
- Siegel R, Naishadham D, Jemal A. Cancer statistics, 2013. CA Cancer J Clin 2013, 63:11-30.
- Chou R, Croswell JM, Dana T, et al. Screening for prostate cancer: a review of the evidence for the US Preventive Services Task Force. Ann Intern Med. 2011;155:762.
- D’Amico AV, Whittington R, Malkowicz SB, et al. Biochemical outcome after radical prostatectomy, external beam radiation therapy, or interstitial radiation therapy for clinically localized prostate cancer. JAMA. 1998;280:969-974.
- Wilt TJ, Brawer MK, Jones KM, et al. Radical prostatectomy versus observation for localized prostate cancer. NEJM> 2012;367:203-213.
- Klotz L, Zhang L, Lam A, et al. Clinical results of long-term follow-up of a large, active surveillance cohort with localized prostate cancer. J Clin Oncol. 2010;28:126-131.
- Cooperberg MR, Lubeck DP, Meng MV, et al. The changing face of low-risk prostate cancer: trends in clinical presentation and primary management. J Clin Oncol. 2004;22:21412149.
- Peeters ST, Heemsbergen WD, Koper PC, et al. Dose-response in radiotherapy for localized prostate cancer: results of the Dutch multicenter randomized phase III trial comparing 68 Gy of radiotherapy with 78 Gy. J Clin Oncol. 2006;24:1990-1996.
- Zelefsky MJ, Yamada Y, Fuks Z, et al. Long term results of conformal radiotherapy for prostate cancer: impact of dose escalation on biochemical tumor control and distant metastases-free survival outcomes. Int J Rad Oncol Bio Phys. 2008;71:1028-1033.
- Siegel R, Naishadham D, Jemal A. Cancer statistics, 2012. CA Cancer J Clin 2012;62:10-29.
- Döhner H, Stilgenbauer S, Benner A, et al. Genomic aberrations and survival in chronic lymphocytic leukemia. NEJM. 2000;343:1910-1916.
- National Comprehensive Cancer Network Inc. NCCN Guidleines Version 1.2014 CLL/SLL. http://www.nccn.org/professionals/physician_gls/pdf/nhl.pdf. Accessed January 20, 2014.
- Park JJ, Chen M-H, Loffredo M, D’Amico AV. Prostate-Specific Antigen Velocity Before and After Elimination of Factors That Can Confound the Prostate-Specific Antigen Level. Int J Rad Oncol Bio Phys. 2012;82:1217-1221.
- Haas R, Poortmans P, De Jong D, et al. High response rates and lasting remissions after low-dose involved field radiotherapy in indolent lymphomas. J Clin Oncol. 2003;21:2474-2480.
- Zelenetz A, Abramson J. NCCN: Non-Hodgkin’s lymphoma. NCCN Guidelines 2013.
- Morrison WH, Hoppe RT, Weiss LM, et al. Small lymphocytic lymphoma. J Clin Oncol. 1989;7:598-606.
- Wiernik PH. Second neoplasms in patients with chronic lymphocytic leukemia. Current treatment options in oncology 2004;5:215-223.
- Chung HT, Xia P, Chan LW, et al. Does image-guided radiotherapy improve toxicity profile in whole pelvic-treated high-risk prostate cancer? Comparison between IG-IMRT and IMRT. Int J Rad Oncol Bio Phys. 2009;73:53-60.
- Michalski JM, Gay H, Jackson A, et al. Radiation dose–volume effects in radiation-induced rectal injury. Int J Rad Oncol Bio Phys. 2010;76:S123-S129.
- Viswanathan AN, Yorke ED, Marks LB, et al. Radiation dose–volume effects of the urinary bladder. Int J Rad Oncol Bio Phys. 2010;76:S116-S122.
- Kavanagh BD, Pan CC, Dawson LA, et al. Radiation dose–volume effects in the stomach and small bowel. Int J Rad Oncol Bio Phys. 2010;76:S101-S107.
- Mohler JL, Armstrong AJ. NCCN: Prostate Cancer. NCCN Guidelines 2013.
- Snyder CF, Frick KD, Herbert RJ, et al. Quality of Care for Comorbid Conditions During the Transition to Survivorship: Differences Between Cancer Survivors and Noncancer Controls. J Clin Oncol. 2013;31:1140-1148.