Virtual Radiation Oncology Resident Rotations: Preserving Learning During a Pandemic
Images

Amidst the coronavirus 2019 (COVID-19) pandemic, residents in graduate medical education (GME) face unique challenges. Radiation oncology (RO) residents must balance caseload requirements, board exams, and personal obligations. Decreased clinic volumes and social distancing measures have necessitated new adaptations such as virtual learning.
The American Council on GME (ACGME) allows for “participating sites” in addition to a “sponsoring institution.”1 Even before COVID-19, smaller RO residencies may rely on external rotations to meet ACGME requirements and achieve clinical competency. Survey-based data reveals that 38% of RO residency programs require external rotations.2
In the face of an unprecedented global pandemic, institutions may implement varying policies regarding visiting residents. RO residency program directors (PDs) and the participating site directors (PSDs) must balance resident education with patient safety and institutional policies. We report our initial experience in rapidly converting a visiting rotation into a virtual resident rotation (VRR).
Methods
The goal of the VRR was to preserve the in-person experience, requiring a dynamic re-thinking of how to incorporate the key components of patient encounters, simulation, contouring, treatment planning, and didactics. VRR was piloted by 2 of 6 RO residents between April and July 2020. An example of a typical schedule is in Table 1. This study did not require internal review board (IRB) submission as deemed by authors according to institutional policy.
Remote Access
Residents were responsible for operability of a virtual private network (VPN) to access on-site resources.
Patient Encounters
Residents participated in patient encounters over telehealth software to include initial consultation, on-treatment visits (OTV), and follow-ups. Residents pre-wrote the consultation note. Participating actively in the patient encounter was dependent on their ability to maintain a professional home environment (suitable for patient interaction). They could join the actual consultation or conduct a postconsult review session, which focused on relevant findings and learning points.
Residents participated in OTVs and follow-ups based on level of training. Generally, salient learning points for all cases were discussed at the end of each day to prevent disruption to clinic flow. To augment learning, residents reviewed each case in advance (to include treatment plans) in detail.
Simulation
Residents discussed simulation techniques prior to the encounter and reviewed any relevant findings after simulation. Residents also coordinated the fusion of relevant imaging.
Contouring
Residents contoured all normal structures and target volumes using the treatment planning system (TPS) over VPN. All contours were reviewed jointly using screen share capabilities of a virtual meeting platform.
Treatment Planning
All patients contoured had their treatment planning and evaluation coordinated with dosimetry/physics virtually, including use of screen share and video-enabled calls. All treatment plans were evaluated jointly using a virtual meeting platform.
Didactics
Residents had residency didactics, which were converted to a virtual format. Additionally, residents participated in informal, Socratic-method-based teaching. This included review of relevant clinical trials and case-based learning. In addition, a “mini-journal club” was held once weekly.
Results
In our small residency of 6 residents, 2 participated in the VRR experience at a single participating institution. A post-VRR survey was conducted assessing the VRR and included 3 of 4 attending physicians at the participating site, and 2 of 2 rotating residents. Contouring, treatment planning, and didactics/teaching were reported to have the same learning value as an in-person rotation, while patient encounters were reported to have less learning value than an in-person rotation. The time commitment for teaching/learning was reported to be less or the same as compared to an in-person rotation for both staff and residents. The level of existing technology infrastructure was unanimously felt to be adequate to support the VRR. All participants reported a positive overall experience with the VRR, and all participants felt that it could be implemented for access to unique learning opportunities (such as global health, proton therapy experiences, etc.).
Discussion
While there have been several recent efforts to implement a virtual curriculum for medical students3 and incoming RO residents,4 there are no reports in the literature regarding RO visiting resident rotations. While 38% of residency programs require external rotations 1-12 months in duration, there was no policy governing external rotations at 30% of these programs.2 The burden of these required external rotations likely falls disproportionately on smaller training programs. These programs already face the challenge of balancing resident time and caseload, as they have less protected nonclinical time.5
The most analogous situation is the implementation of a virtual medical student RO clerkship.3 Pollom et al implemented a 2-week virtual rotation conducted in small teams, which allowed for virtual patient interaction, multidisciplinary didactics, and exposure to treatment planning. In their early report, they felt the virtual clerkship broadened the reach of an RO clerkship, particularly in the era of COVID-19.3 These endeavors are being continued in a multi-institutional effort called Radiation Oncology Virtual Education Rotation (ROVER).
Our initial experience demonstrates the adaptability of RO GME in the face of an unprecedented pandemic. As virtual platforms are now used routinely in RO clinical care, we were able to rapidly restructure a rotation using existing virtual technologies. This experience may also be beneficial in other contexts, such as those facing financial difficulty in travel, increasing accessibility to global health RO experiences, etc. Common applications could include proton therapy VRRs and rotations in subsites where case numbers may be limited (eg, pediatric malignancies).
Global health has gained interest in RO as a career opportunity; nonetheless, it has been shown to have little formalized training and restricted leadership opportunities.6 Recent efforts to establish a global health track6 include offering a competency profile7 and multiple perspectives on how to increase trainee engagement.8,9 Leveraging such technologies amidst COVID-19 show the possibilities of creating an analogous experience to increase accessibility to global RO.
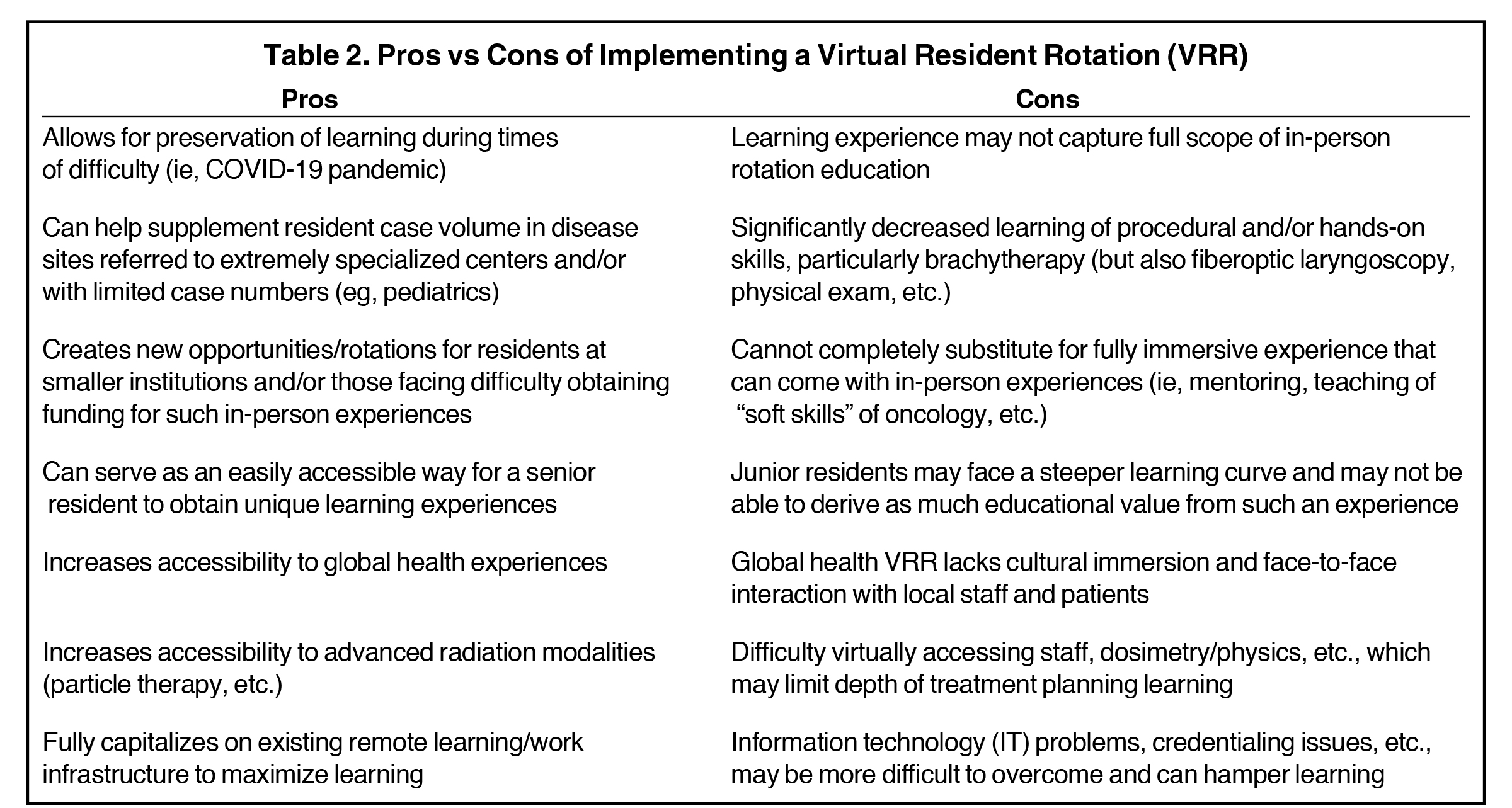
The residents who participated in the VRR focused most of their time on head and neck cancer, genitourinary cancer, and breast cancer. It was largely felt that most of the learning related to external-beam radiation therapy (EBRT) treatment planning was preserved for rotating residents on the VRR. Due to COVID-19, no brachytherapy was conducted; however, this is a shortfall of the VRR. While many institutions rely on external rotations to gain brachytherapy experience, especially in prostate and gynecologic cancers, a VRR would not adequately substitute for this learning experience. Table 2 provides a comprehensive list of VRR pros and cons.
VRR has multiple limitations as a direct replacement to a critical clinical rotation. A VRR cannot incorporate all aspects of RO clinical care, such as hands-on clinical skills (eg, physical examination, fiberoptic laryngoscopy, real-time image verification, etc.), tools to run a busy clinic, etc. Additionally, the virtual nature places a burden on both the resident and attending to prioritize learning opportunities proactively. We therefore recommend that such experiences be pursued by senior residents, as junior residents may face a steep learning curve that may portend a suboptimal educational experience.
Limitations specific to this report include a small sample size (2 residents); however, this is a pilot experience from a small residency program. Additionally, no objective metrics were used to evaluate the VRR prospectively, and this may be the subject of future RO GME efforts.
Conclusions
Our initial experience of a VRR demonstrates how implementing the latest technology can preserve most aspects of clinical learning in RO resident education in light of COVID-19. In addition, it presents an exciting way to allow for broadened accessibility to global health experiences and advanced radiation modalities.
References
- ACGME Program Requirements for Graduate Medical Education in Radiation Oncology, American Council on Graduate Medical Education, 2020.
- Harris EE, Abdel-Wahab M, Spangler AE, Lawton CA, Amdur RJ. Results of the Association of Directors of Radiation Oncology Programs (ADROP) survey of radiation oncology residency program directors. Int J Radiat Oncol Biol Phys. 2009;74(2):327-337. doi:10.1016/j.ijrobp.2008.12.079
- Pollom E, Sandhu N, Frank J, et al. Continuing medical student education during the Covid19 pandemic: development of a virtual radiation oncology clerkship. Adv in Radiat Oncol. 2020;5(4):732-736. doi:10.1016/j.adro.2020.05.006
- Gunther JR, Jimenez RB, Yechieli RL, et al. Introductory radiation oncology curriculum: report of a national needs assessment and multi-institutional pilot implementation. Int J Radiat Oncol Biol Phys 2018;101 (5):1029-38. doi:10.1016/j.ijrobp.2018.04.020
- Parekh AD, Culbert MM, Brower JV, Yang GQ, Golden DW, Amdur RJ. Nonclinical time in U.S. radiation oncology residency programs: number of months and resident opinion of value. Int J Radiat Oncol Biol Phys 2020;106 (4):683-9. doi:10.1016/j.ijrobp.2019.11.030
- Rodin D, Yap ML, Grover S, et al. Global health in radiation oncology: the emergence of a new career pathway. Semin Radiat Oncol. 2017;27(2):118-123. doi:10.1016/j.semradonc.2016.11.003
- Oar A, Yap ML, Rodin D, McNiven A, Papadakos J, Giuliani M. Postgraduate global health competency profile for radiation oncology. Clin Oncol. 2018;30(12):810-816. doi:10.1016/j.clon.2018.08.019
- Elmore SNC, Royce TJ, Oladeru OT, et al. Global health perspectives among radiation oncology residency program directors: a knowledge, attitudes, and practices survey. Int J Radiat Oncol Biol Phys. 2020;107(3):419-425. doi:10.1016/j.ijrobp.2020.02.467
- Elmore SN, Sethi RV, Viswanathan AN, Efstathiou JA. Global radiation oncology from the trainee perspective: a view from beyond the bunker. Int J Radiat Oncol Biol Phys. 2016;94(3):438-439. doi:10.1016/j.ijrobp.2015.11.033
Citation
AR C, AK B, AJ W, D E, A T, BR P. Virtual Radiation Oncology Resident Rotations: Preserving Learning During a Pandemic. Appl Radiat Oncol. 2020;(4):21-23.
December 24, 2020