Radiation Therapy-Induced Toxicity in a Breast Cancer Patient With Variance of Unknown Significance in the Ataxia Telangiectasia Gene
Applied Radiation Oncology — Vol. 12, Issue 3, pp. 1-3
Published: September 1, 2023
1 Department of Internal Medicine, Cooper University Healthcare, Camden, NJ
2 Plastic Surgery Arts of New Jersey and Saint Peters University Hospital, New Brunswick, NJ
3 Department of Radiation Oncology, Saint Peter’s University Hospital, New Brunswick, NJ
* Corresponding author: Akshay Nilesh Desai (desai-akshay@cooperhealth.edu)
Abstract
Keywords
ataxia telangiectasia, telangiectasias, fibrosis, breast radiation, radiation pneumonitis, dermatitis, toxicity, side effects
Case Summary
A 51-year-old woman presented in 2018 after a screening mammogram discovered asymmetry in the right subareolar region with a 15 × 13 × 14 mm mass on ultrasonography. Breast biopsies revealed triple-positive infiltrating ductal carcinoma. She had no history of collagen vascular diseases or prior radiation. Genetic testing revealed a heterozygous variance of unknown significance (VUS) in the ataxia telangiectasia (ATM) gene (c.3158A>T(p.Asp1053Val)) and negative BReast CAncer gene (BRCA) testing. She underwent neoadjuvant chemotherapy with Adriamycin and cyclophosphamide, followed by Taxol, Herceptin, and pertuzumab. Subsequent right partial mastectomy showed grade 2 residual invasive ductal carcinoma. She received a total dose of 5000 cGy of 3D radiation therapy to the right breast and the supraclavicular and axillary lymph nodes with a boost.
The patient developed cutaneous symptoms, which progressed to telangiectasias and significant fibrosis (Figure 1). In addition, she developed radiographically detected asymptomatic radiation pneumonitis (Figure 2A-B).
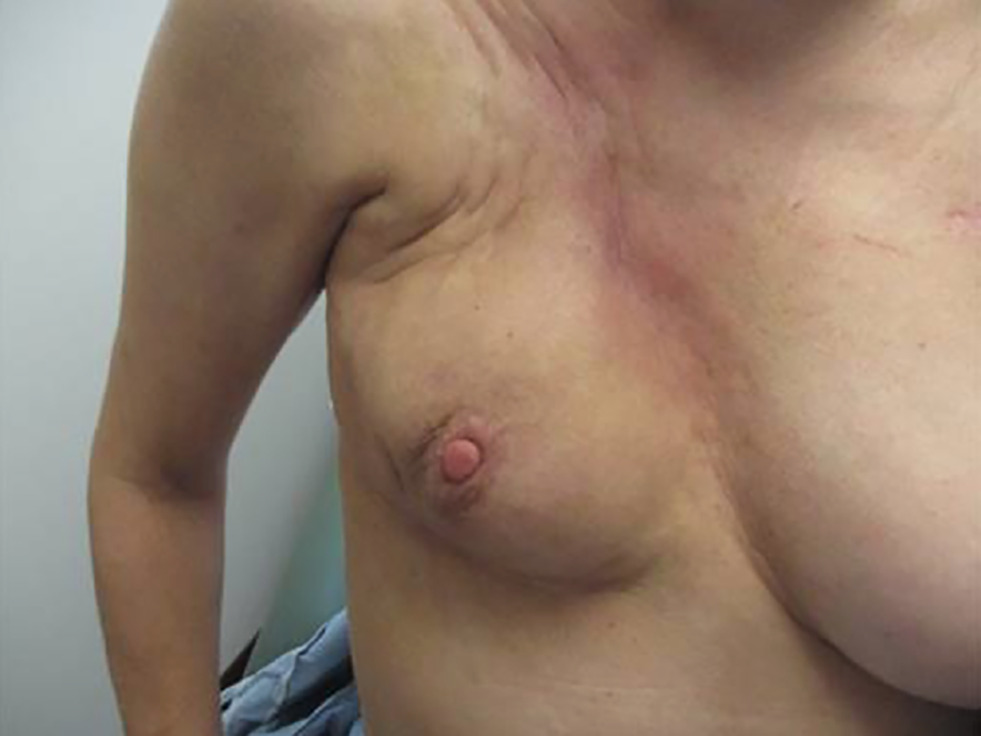
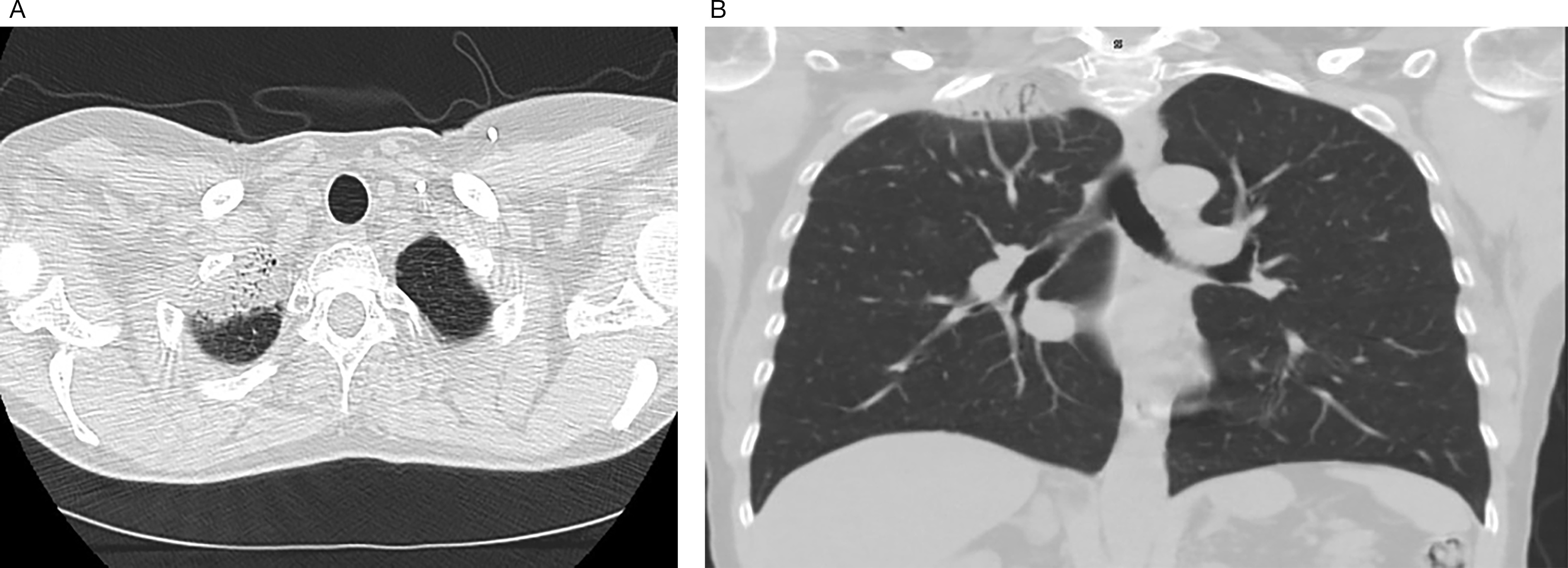
Platelet-rich infusions, used for fibrosis treatment, were ineffective. The patient subsequently underwent a mastectomy.
Discussion
By facilitating DNA double-stranded breaks, ionizing radiation is known to cause damage to both malignant and nonmalignant cells. In patients with mutant ATM genes, DNA repair via nonhomologous DNA end-joining is impaired, which raises concern for an increased sensitivity to radiation therapy1,2. The data regarding increased toxicity from radiation therapy in heterozygous carriers of ATM mutations are unclear. Furthermore, it is also unclear whether there is a correlation between VUS mutations and an increased sensitivity to radiation. An extensive database regarding VUS mutations across several genes is available on the ClinVar website. Of the 8945 submitted variants of the ATM gene, more than 50% (4742) were deemed to be VUS mutations.3
Clinical investigations attempting to assess the link between VUS and increased radiation sensitivity have been unclear, with different studies yielding contradictory results. In a study assessing 91 evaluable carriers of ATM variants, of whom 23 harbored a pathological variant while 68 harbored VUS, researchers determined no evidence of increased radiation-associated toxicity among carriers of pathogenic ATM germline variants.4 Another study assessed 357 pan-cancer patients who received a cumulative total of 727 courses of radiation therapy, determining that genetic inactivation of ATM was associated with an improved radiotherapeutic efficacy.5
However, one case series demonstrated that patients with heterozygous germline ATM mutations can have widely varying clinical responses to radiation therapy, ranging from benign to severe,6 as was seen in our patient’s case. Moreover, the landmark WECARE study discovered increased contralateral breast cancers in radiated patients possessing otherwise nonpathologic ATM variants.7
ATM heterozygotes make up approximately 1% of the general population, and it has been shown in epidemiologic studies that this mutation confers a 3- to 5-fold increase in the risk of developing breast cancer. However, understanding the clinical significance of VUS in the ATM gene is vital for patients undergoing radiation treatment. While it has been discussed that VUS should be considered normal and should not confer increased radiosensitivity to patients,8 our patient’s severe cutaneous toxicity serves as a reminder that adverse radiation-induced effects can be seen in patients with VUS. Recent guidelines recommend that radiation therapy should be offered when clinically indicated for women with breast cancer who are carriers of an ATM mutation.9 Therefore, more investigation is needed into VUS mutations to determine the significance of single-nucleotide alterations. We present this case so that it can be added to the ClinVar website and future patients could be counseled and avoid the severe side effects seen in this patient.
Conclusions
The ATM gene is a critical regulator of DNA double-strand breaks and ensures appropriate mismatch repair. We present a case of a patient with triple-positive breast cancer and a VUS ATM gene, who developed significant fibrosis and cutaneous scarring following radiation therapy. Certainly, it is possible that there is a subset of VUS in which some patients may develop more deleterious side effects than others. Nevertheless, our case underscores the need for further analysis of VUS mutations and appropriate patient counseling, determining the risk of radiation toxicity in these patients.
References
- Dosani M, Schrader K, Nichol A. Severe late toxicity after adjuvant breast radiotherapy in a patient with a germline ataxia telangiectasia mutated gene: future treatment decisions. Cureus. 2017;9(7). doi:doi:10.7759/cureus.1458.
- Ho A, Fan G, Atencio D. Possession of ATM sequence variants as predictor for late normal tissue responses in breast cancer patients treated with radiotherapy. Int J Radiat Oncol Biol Phys. 2007;69(3):677-684. doi:doi:10.1016/j.ijrobp.2007.04.012.
- Hosoya N, Miyagawa K. Implications of the germline variants of DNA damage response genes detected by cancer precision medicine for radiological risk communication and cancer therapy decisions. J Radiat Res. 2021;62(supplement_1):i44-i52. doi:doi:10.1093/jrr/rrab009.
- Modlin L, Flynn J, Zhang Z. Tolerability of breast radiotherapy among carriers of ATM germline variants. JCO Precis Oncol. 2021;5. doi:doi:10.1200/PO.20.00334.
- Pitter K, Casey D, Lu Y. Pathogenic ATM mutations in cancer and a genetic basis for radiotherapeutic efficacy. J Natl Cancer Inst. 2021;113(3):266-273. doi:doi:10.1093/jnci/djaa095.
- Mullins B, Gupta G. Increased radiation toxicity with germline ATM variant of uncertain clinical significance. Rep Pract Oncol Radiother. 2019;24(6):672-680. doi:doi:10.1016/j.rpor.2019.09.008.
- Reiner A, Robson M, Mellemkjær L. Radiation treatment, ATM, BRCA1/2, and CHEK2*1100delC pathogenic variants and risk of contralateral breast cancer. J Natl Cancer Inst. 2020;112(12):1275-1279. doi:doi:10.1093/jnci/djaa031.
- Bergom C, West C, Higginson D. The implications of genetic testing on radiation therapy decisions: a guide for radiation oncologists. Int J Radiat Oncol Biol Phys. 2019;105(4):698-712. doi:doi:10.1016/j.ijrobp.2019.07.026.
- McGuire K, Mamounas E. Management of hereditary breast cancer: ASCO, ASTRO, and SSO guideline. Ann Surg Oncol. 2020;27(6):1721-1723. doi:doi:10.1245/s10434-020-08396-8.
Disclosures
The authors have no conflicts of interest to disclose. None of the authors received outside funding for the production of this original manuscript and no part of this article has been previously published elsewhere. The patient has provided informed consent for the publication of this case report.
Citation
. Radiation Therapy-Induced Toxicity in a Breast Cancer Patient With Variance of Unknown Significance in the Ataxia Telangiectasia Gene. Applied Radiation Oncology. 2023;12(3):1-3. doi:10.37549/ARO-D-23-00015.