Patient education in radiation oncology: Evolution and innovation
Images
SA-CME credits are available for this article here.
Patient education is a dynamic and evolving area of medicine, with important applications for patient care, compliance, and comprehension of health information. Improving patients’ understanding of treatment nuances and intricacies can, in turn, potentially boost their adherence to treatment. There is also a significant emotional dimension to patient education, particularly in alleviating stress, uncertainty, and fear associated with treatment.1 Patient education is also critical in encouraging active patient participation and shared decision-making.2 Moreover, the role of patient education has become increasingly critical in the context of medicine’s paradigm shift in decision-making, in which patients take a more active role in treatment decisions. Thus, adequate knowledge and an understanding of treatment complexities are necessary to ensure effective patient participation in this decision-making process.3
Radiation oncology is a particularly complex treatment modality, encompassing several components and extensive care coordination between different professionals.4 Many patients present at first consultation with little knowledge and understanding of the role of radiation treatment in multimodal cancer therapy.4 Moreover, misconceptions exist regarding radiation—including the belief that radiation causes, rather than treats, cancer—providing an additional role for education in this field.5 Features of radiation treatment considered significant for incorporating into patient education material include technical information about radiation, side effects of treatment, emotional dimensions and self-care, follow-up, and design and implementation of a wellness plan.6 Furthermore, adequate knowledge and understanding of radiation treatment is critical for effective patient participation in decision-making. In particular, information about the benefits and potential long-term side effects of radiation is considered essential for making well-informed decisions regarding treatment. Patient education is a vector to deliver such information, ultimately empowering patients to take an active role in their care.7,8 This article will discuss the evolution of patient education in radiation oncology, examining education tools and practices, as well as new innovations and future directions.
Background
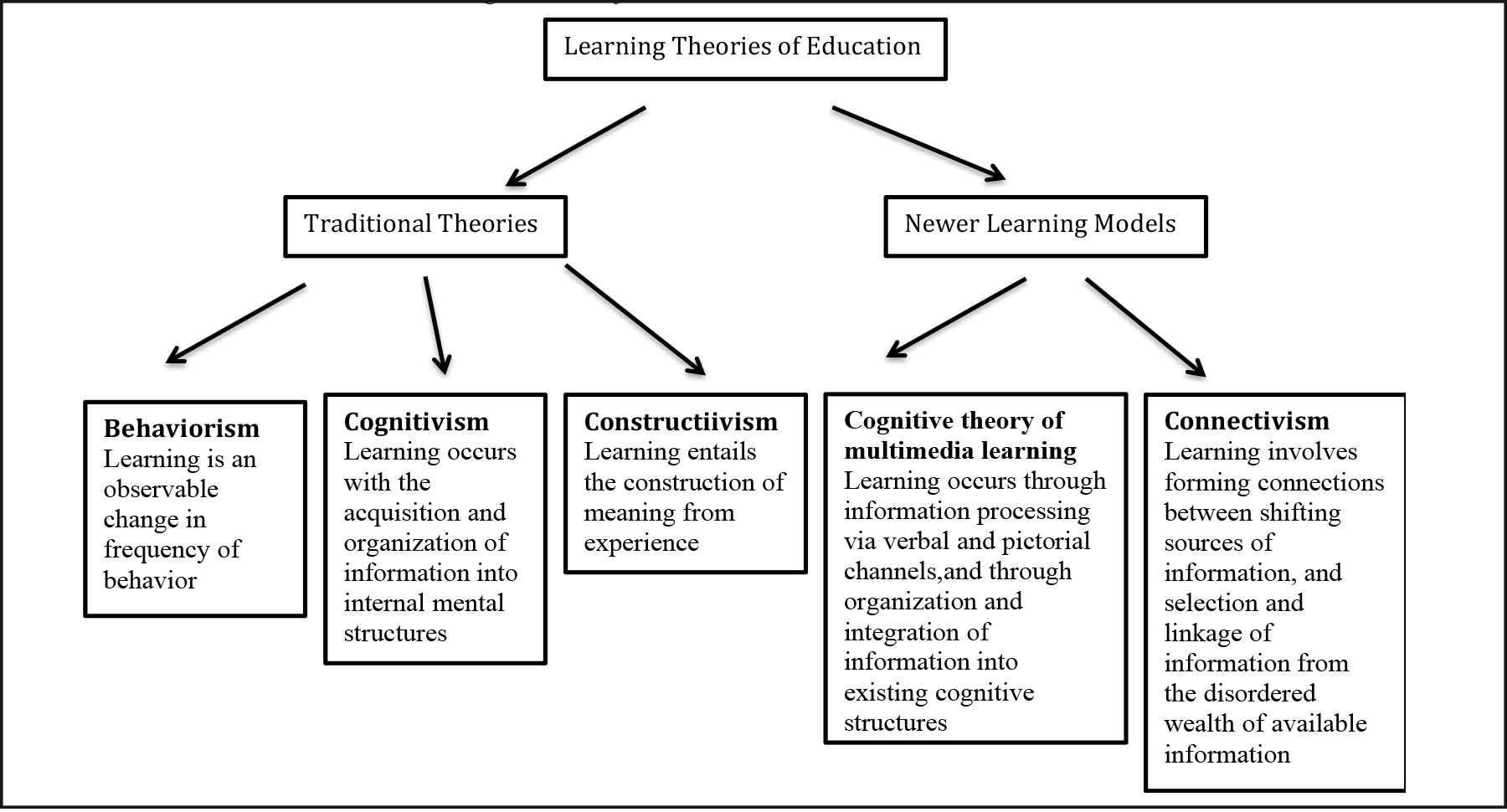
In determining the most effective methods and tools for patient education in radiation oncology, one must consider how patients best learn. Attention to learning theories of education is helpful in this regard (Figure 1). The major traditional learning theories include constructivism, which emphasizes the construction of meaning from experience; cognitivism, which focuses on the acquisition and organization of information into internal mental structures; and behaviorism, which considers learning to be an observable change in frequency of behavior.9 From a behaviorist perspective, patients will have exhibited adequate learning when they demonstrate changed patterns of behavior. In the context of radiation, this can be seen through changes in patient behaviors such as improved management of treatment side effects (eg, consistent use of a vaginal dilator in pelvic radiation), or greater adherence to treatment recommendations (eg, bladder or bowel emptying prior to daily radiation). The cognitivist theory of learning can help us understand how patients acquire and assimilate information presented through educational tools into their existing cognitive structures.
Moreover, newer theories of learning continue to emerge, including models that consider the growing influence of technology in people’s lives. In particular, the cognitive theory of multimedia learning explains how people learn from words and pictures through information processing using two channels—one for verbal and one for pictorial material.10 In this model, effective learning consists of proper cognitive processing, which includes attention to relevant information and organizing such information into a coherent cognitive structure. This also requires activating long-term memory by integrating new information with existing knowledge. Given the trend in radiation oncology toward more engaging patient educational tools that employ increasing visual components, this theory has significant applications to the design and implementation of patient education tools. In addition, online sources of information, including web pages and social media forums, are an emerging and increasingly significant form of patient education tools, as will be discussed. A newer learning theory of education—connectivism, which focuses on integrating knowledge and forming connections between shifting and evolving sources of information—helps one understand how these tools can shape learning.11 Selecting and linking information into a network from the expansive, complex, and disordered wealth of information from which to draw—the connection of knowledge—is a key concept in this theory. In the context of patient education, this theory helps us understand how patients can learn from, and ultimately integrate information between, multiple and dynamic sources of information, some of which are nonhuman.
Patient education can also serve as a sign of quality care. The Centers for Medicare & Medicaid services (CMS) implement guidelines to ensure its recipients receive quality health care, defined by efficacy, safety, efficiency, patient-centeredness, equitability, and timeliness.12 “Health Promotion and Education” is among the CMS-mandated quality metrics. Moreover, several other CMS quality care measures also incorporate education, such as through preventive health education, education for in-hospital stays, and discharge instructions, further highlighting its critical role in quality care. In radiation oncology, patient education can have important implications in defining high-quality care. It can serve as one indicator of provider time spent with the patient and the degree of patient-centeredness of a clinic visit. Furthermore, the use of educational tools in a clinical setting can be standardized with instruction to provide an objective criterion for equitable physician-patient communication. Robinson et al reviewed characteristics and measures of patient-centered care, reporting patient education, patient involvement in care, shared decision-making, and communication as critical components.13 They found patient-centered interactions to be associated with increased adherence to treatment and physician recommendations, as well as improved health outcomes. Patient education also plays an important role in patient safety.14
Tools and Practices
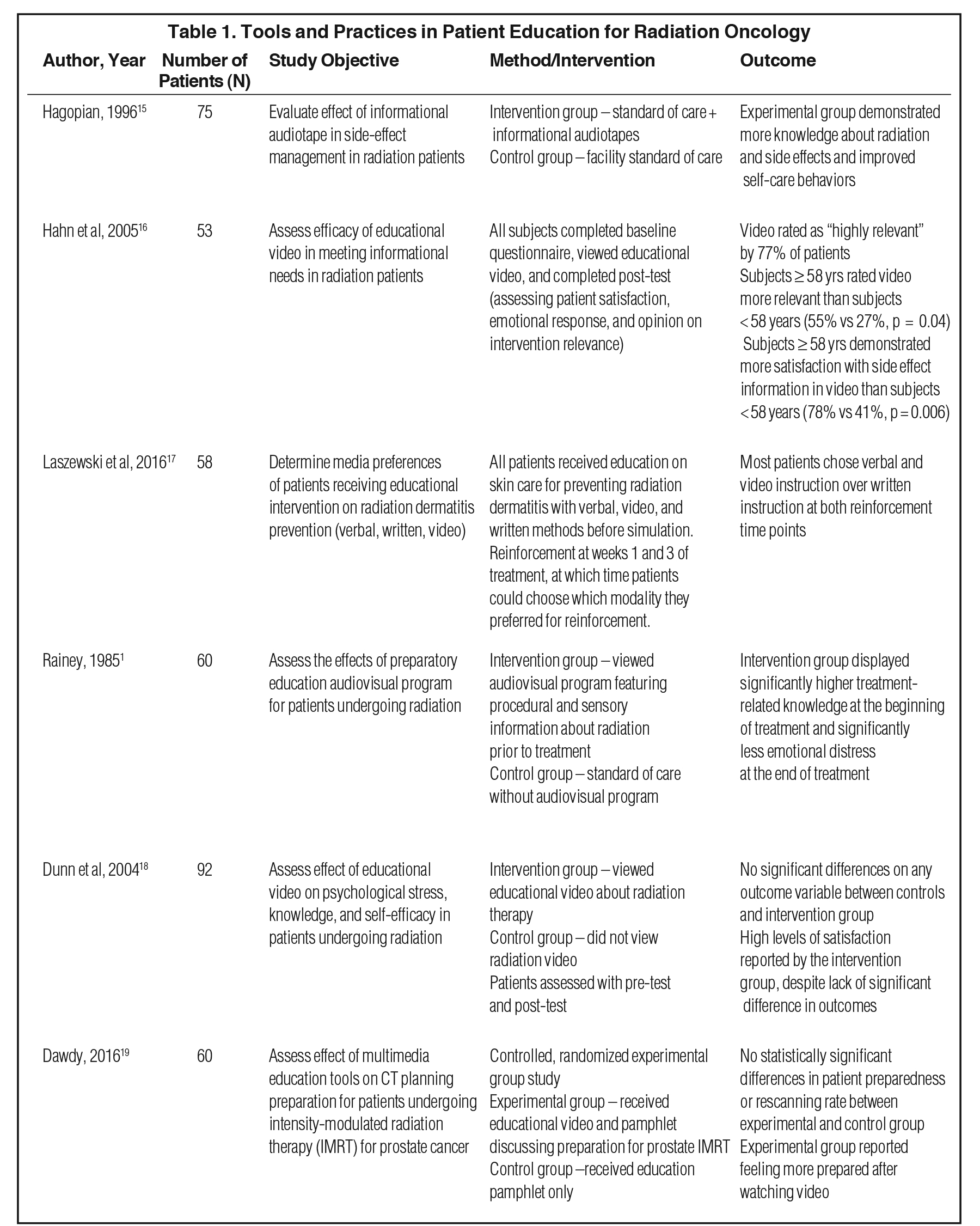
Different forms of patient education tools have been utilized in the clinical setting, with varying degrees of efficacy in radiation therapy (Table 1). In addition to direct verbal education from providers, earlier tools have included pamphlets and printed materials. However, educational materials soon evolved to incorporate different modalities, engaging patients more actively and providing information more effectively. For example, a study assessing the potential benefit of educational audiotapes in patients undergoing radiation found that audiotapes discussing radiation treatment and the management of side effects resulted in improvements across several outcome measures compared to the facility’s standard of care. These included demonstrated knowledge of radiation and its potential side effects, and the use of more beneficial self-care practices.15
With the regular use of computers during the patient visit, education videos became, and remain, a popular and effective tool for providing information about radiation treatment and improving patient comprehension. The use of these videos in a clinical setting has been associated with high patient satisfaction. For example, a prospective study evaluating the efficacy of an educational video in 53 radiation oncology patients reported that 77% of participants found the video to be highly relevant, and more than 90% were highly satisfied with video information describing simulation and radiation treatment.16 Additionally, older patients reported greater satisfaction with the video compared to younger patients, indicating a potential additional benefit to audiovisual forms of education in this patient population. Many patients may prefer audiovisual education materials compared to verbal and/or written materials as well. In an analysis of patient preference for educational reinforcement concerning radiation dermatitis, Laszewski et al found that patients prefer video education tools and verbal reinforcement compared to written materials.17 Moreover, some studies have found that audiovisual aids are more successful in helping patients better understand the complexities of radiation treatment compared to verbal and/or written materials alone. In a study by Rainey et al, patients who viewed an audiovisual program featuring procedural and sensory information about radiation prior to treatment displayed significantly higher treatment-related knowledge at the beginning of treatment, and significantly less emotional distress at the end, compared to patients who received standard of care without the audiovisual program.1 Their results also highlight the critical emotional role of education in alleviating fear and uncertainty patients feel in anticipation of treatment.
It should be noted, however, that the literature is mixed regarding the efficacy of videos over more traditional forms of patient education materials in terms of improved objective response measures. Some studies have found that even when patients report satisfaction with videos, they may fail to show significantly increased knowledge or modification of behaviors targeted by the education materials than patients who receive pamphlets and handouts alone.18,19 Nevertheless, given that the majority of these studies found significantly higher patient satisfaction and feelings of preparedness for treatment, there are clear benefits to audiovisual modality use even in the absence of strictly “educational” improvements—especially in the context of anxiety and uncertainty associated with radiation treatment.
Considering Online Sources of Information
In addition to educational resources presented in the clinical setting, patients now have access to a wealth of online information about radiation. A 2001 multi-institutional study assessing internet utilization by patients receiving radiation found that 42% of patients presenting at academic centers and 29% of patients presenting at community centers used the internet to find information about cancer, with 62% of patients treated at academic centers owning a computer in the home.20 Additionally, a survey study evaluating the impact of media and internet on oncology patients and providers in Canada found that 50% of patients actively search for information related to their illness using the internet; additionally, access to the internet was one predictor of higher rates of information seeking. These percentages have likely increased substantially in recent years with the growing number of patients with direct internet and computer access.
There are clear benefits to patient internet use—particularly, in supplementing educational materials presented in clinic with additional information that cannot be provided during a short doctor’s appointment. However, there are also concerns regarding the accuracy of online information, as well as patients’ ability to understand and interpret such information as it relates to their illness and care. In Chen and Siu’s analysis, most oncologists believe that patients have difficulty interpreting online medical information accurately.21 YouTube has become a popular platform to access free educational and instructional videos in a variety of areas; medical treatment topics, including radiation therapy, are no exception. Prabhu et al assessed the quality of brachytherapy educational videos on YouTube by comparing the video content with respect to information provided in the brachytherapy informed consent guidelines.22 Only 3.6% of videos met standards, while half were below standards. Moreover, only half of the videos were uploaded to the site by physicians, hospitals, or private practices. Given how frequently these videos were viewed (median views were 4482.5, with a range of 212 to 415 007), there is a critical need to ensure the accuracy and comprehensiveness of content in these easily accessible patient education tools.
It is important to note that a significant limitation of radiation oncology patient education materials involves the readability and complexity of terminology used, particularly in online materials.23 An evaluation published in 2016 of patient education materials from the websites of the American Society for Radiation Oncology (ASTRO), American Association of Physicists in Medicine (AAPM), American Brachytherapy Society (ABS), RadiologyInfo.org, and Radiation Therapy Oncology Group (RTOG) found nearly all articles to be written at an education level higher than that recommended by the National Institutes of Health (NIH) and American Medical Association (AMA).24 The majority of the information in these materials, therefore, may not be fully understood by patients who read them.
New Innovations and Future Directions
New directions in patient education for radiation attempt to bypass the need for patients to conceptualize complex medical jargon and instead provide a virtual, 3-dimensional (3D) experience. Innovative multimodal patient education tools are being increasingly explored as new options for improving understanding and engaging patients undergoing radiation therapy (Table 2). This realm uses technology to engage a generation of patients with access to a host of devices and platforms, including virtual reality, social media and apps. In particular, interest is rapidly expanding in the use of virtual reality to foster understanding of complex aspects of radiation therapy and visualizing radiation treatment, which remains nebulous and difficult for many patients to picture.25
Williams et al demonstrated the potential benefits of incorporating 3D visualization into radiation oncology patient education tools.26 In their survey analysis, patients were shown a video about the treatment process that included real footage and 3D animations before receiving their first fraction. The majority of patients (98%) found the video useful in meeting informational needs, and a third of patients reviewed the videos again, mostly to help explain radiation therapy to family/friends, indicating a potential use for visualization tools to expand education beyond the patient.
The 3D visualization applications of patient education have expanded to immerse patients in a full virtual reality system. The Virtual Environment for Radiotherapy Training system (VERT) is a simulation tool that utilizes virtual reality to help train radiation therapy practitioners; however, it has recently been used for patient education applications in several studies.27 Jimenez et al studied VERT as part of an education program for breast cancer patients, which included content on radiation immobilization, computed tomography (CT) simulation, treatment planning, and treatment delivery.27 The authors found high levels of patient satisfaction with the 3D features of VERT and with program comprehensiveness, highlighting the benefit of visualization in the tools used to convey information about radiation. Flockton also found benefits associated with VERT for patient education purposes.28 In a study of patients with prostate cancer, VERT was used to simulate the delivery of radiation to the prostate, and to visually demonstrate the importance of a full bladder and empty rectum consistently during treatment. Participants found that VERT helped them better understand radiation therapy (including its technologies) and visualize the treatment process, ultimately improving feelings of preparedness for treatment. The patients also reported that VERT helped them better understand why a full bladder and empty rectum are required for treatment. This latter finding also highlights the significant implications that emerging patient education tools have for patient compliance in radiation oncology.28
The use of VERT also has important applications for better addressing the emotional dimensions of undergoing radiation therapy. Visual familiarity with the treatment process prior to receiving the first fraction can better prepare patients for what to expect, reducing fear of the unknown and anxiety associated with treatment. These benefits have already been demonstrated in studies using 3D visualization and/or VERT. In Williams et al’s study, nearly half of all patients reported feeling less anxious and scared about treatment after watching the video with 3D animation.26 Marquess et al found that in patients with prostate cancer who participated in VERT, anxiety significantly decreased, specifically about the in-treatment experience, daily x-rays, radiation dose to the prostate, movement of the accelerator close to the patient, and regarding overall treatment precision.29
Social media and apps are also potential innovative vehicles for patient education in radiation oncology, harnessing the growing influence of technology in everyday lives. For example, Twitter has been shown to be effective in providing education and support to patients with breast cancer.30 In 206 patients with breast cancer who participated in the Breast Cancer Social Media Twitter support community, the majority of patients reported increased overall knowledge about breast cancer, metastatic disease, research and clinical trials, treatment options, imaging, radiation oncology, and more. Moreover, participation in this social media support group not only increased knowledge, but also changed behaviors and follow-up actions. For example, 31.2% of patients sought a second opinion or presented additional information to their providers following participation, while 71.9% stated they would now engage in outreach and advocacy for breast cancer. Moreover, 67% of patients reported decreased anxiety after participation, highlighting the emotional impact of social media tools in radiation oncology.
Apps have also been evaluated in the context of symptom management during radiation treatment, with potential applications for pre-treatment education.Langius-Eklof et al had patients undergoing radiation for prostate cancer report information about their symptoms daily using the Interaktor.31 Most of the patients consistently used the app, describing it as easy to use. Given today’s widespread app use and the apparent feasibility of treatment-related applications, apps can potentially enhance patient education in radiation oncology.
Contextual Considerations
It is important to note that these emerging education tools may not be the most suitable option for all patients. Age, among many factors, plays an important role. For example, in elderly patients perhaps less familiar with the technologies and online platforms of newer education tools, more traditional materials and methods may be more effective. Clotfelter reported successful outcomes with an educational video and accompanying booklet aimed at improving pain management in elderly patients with cancer.32 Patients who received the educational intervention had significantly lower cancer pain intensity compared to controls. Similarly, Jewitt et al assessed the efficacy of an educational pamphlet on stereotactic body radiation therapy (SBRT) for elderly patients with lung cancer.33 The pamphlet, specifically designed for elderly patients, was considered effective by 86% of the patients. Importantly, most of these patients preferred verbal or written forms of education materials (65% and 78%, respectively), to online information or educational classes. Moreover, attention must be given to the cognitive challenges in elderly cancer patients, which can be further compounded by chemotherapy-induced memory impairment and can impact treatment compliance.34 Educational tools that also consider the cognitive capacities of the patient are ideal.
Age is not the only factor affecting the dynamics of patient education interventions. A variety of social, contextual, and cultural factors play a significant role in shaping the responses to patient education tools. These include culture, race, education, and health literacy, among others.
Illness, and its treatment, is a culturally embedded experience; priorities and expectations of care are shaped by patients’ cultural values.35 Provider-patient communication, including that involved in educational interventions, must take into account a patient’s cultural background. One important component of these cultural dynamics is language barriers, which can pose significant challenges to health information accessibility. Inability to fully understand education materials has important implications for treatment compliance (a frequent target of patient education interventions) and patient satisfaction.35,36 This is especially critical in a field such as radiation oncology, in which treatment is complex and patients, regardless of cultural background, often are unfamiliar with radiation therapy. Multimedia tools in different languages may aid intervention in this regard. For example, Valdez et al evaluated the efficacy of an education intervention for Latina women with cervical cancer using interactive, multimedia kiosks.37 Patients who received the intervention demonstrated significantly improved knowledge about cervical cancer. Attention to cultural factors should be considered when designing education materials for patients undergoing radiation.
Race is another important factor in provider-patient communication, with implications for the development of and response to educational materials for patients.38 Communication factors resulting in inadequate access to health information and lack of shared decision-making play a significant role in unequal health outcomes among racial group.39 Evidence suggests that comprehensive interventions may be necessary to ensure greater equitability in communications and education across racial groups. Anderson et al conducted a pain education intervention in minority patients with cancer, using a culture-specific video and booklet.40 However, there were no significant differences in quality of life, perceived pain control, or functional status between groups that did and did not receive the intervention, suggesting that more comprehensive educational interventions may be required to significantly change outcomes.
Education level and literacy are also important considerations when designing educational tools. Low health literacy has been significantly associated with poorer health outcomes.41 Ensuring educational materials are accessible and understandable for patients with low health literacy is critical, particularly in radiation oncology, which requires strict adherence to daily treatment. Limiting educational objectives, focusing on behaviors, and presenting context initially can increase education material accessibility for patients with low health literacy.42 In addition, the use of audiovisual aids may be particularly important in this patient population by engaging multiple senses in learning.
Conclusion
Radiation oncology remains one of the more misunderstood treatment modalities in cancer care. Many patients know much less about radiation than chemotherapy or surgery, and many have difficulties in comprehending the more complex aspects of treatment. Thus, there is a particularly significant role for patient education in this field, improving knowledge and comprehension, and potentially improving behaviors related to treatment. There is also a significant emotional dimension to patient education, which has the potential to alleviate anxiety, uncertainty, and fear associated with treatment. Traditional education materials have included pamphlets and other written materials; however, audiovisual materials such as videos have been associated with greater patient satisfaction. New considerations have emerged in the Internet Era with patients having widespread access to a wealth of online education resources, many of which are not reviewed and approved by medical providers. Many of these resources are also written at a level beyond that recommended by the NIH and AMA. New tools in patient education attempt to bypass these issues by directly immersing the patient in a 3D virtual reality experience using VERT, helping patients better visualize the treatment process and understand the more complex aspects of radiation therapy at a visceral level. Future directions in patient education for radiation oncology are likely to continue exploring applications of innovative tools and technologies such as VERT, as well as social media platforms, to improve patient education.
References
- Rainey LC. Effects of preparatory patient education for radiation oncology patients. Cancer. 1985;56(5)1056-1061.
- Stacey D, Samant R, Bennett C. Decision making in oncology: a review of patient decision aids to support patient participation. CA Cancer J Clin. 2008;58(5):293-304.
- Ubel PA, Scherr KA, Fagerlin A. Empowerment failure: how shortcomings in physician communication unwittingly undermine patient autonomy. Am J Bioeth. 2017;17(11):31-39.
- Paulsson A, Braunstein SE. Patient communication prior to initial consultation for palliative radiotherapy. J Clin Oncol. 2016;34(26)(suppl):30-30.
- Peck A, Boland J. Emotional reactions to radiation treatment. Cancer. 1977;40(1):190-184.
- Wilcox, Barisic V, Lavergne C, Lemonde M. The perceptions of health care providers and cancer patients on educational needs at the end of radical radiation therapy treatment in a community-based cancer centre. J Med Imag Radiat Sci. 2017:48:S6.
- Wang S, Kelly G, Gross C. Information needs of older women with early-stage breast cancer when making radiation therapy decisions. Int J Radiat Oncol Biol Phys. 2017;15;98(4):733-740.
- Woodhouse KD, Tremont K, Vachani A. A review of shared decision-making and patient decision aids in radiation oncology. J Cancer Educ. 2017;32:238-245.
- Ertmer PA, Newby TJ. Behaviorism, cognitivism, constructivism: comparing critical features from an instructional design perspective. Perf Improv Q, 1993;6(4)50-72.
- Mayer RE. Applying the science of learning to medical education. Med Educ. 2010;44(6):543-549.
- Siemens G. Connectivism: a learning theory for the digital age. Int J Instruct Tech Dist Learn. 2005;2(1)3-10.
- CMS.gov. Centers for Medicare and Medicaid services. https://www.cms.gov/. Page last modified: 12/19/2017. Accessed February 10, 2018.
- Robinson JH, Callister LC, Berry JA et al. Patient-centered care and adherence: definitions and applications to improve outcomes. J Am Acad Nurse Pract. 2008;20(12):600-607.
- An J, Kim SJ, Park S, et al. The effects of patient education on patient safety: can we change patient perceptions and attitudes? Lessons from the Armed Forces Capital Hospital in Korea. Int J Qual Health Care. 2017;29(3)392-398.
- Hagopian GA. The effects of informational audiotapes on knowledge and self-care behaviors of patients undergoing radiation therapy. Oncol Nurs Forum. 1996;23(4):697-700.
- Hahn CA, Fish LJ, Dunn RH, Halperin EC. Prospective trial of a video educational tool for radiation oncology patients. Am J Clin Oncol. 2005;28:609-612.
- Laszewski P, Zelko C, Andriths L et al. Patient preference for instructional reinforcement regarding prevention of radiation dermatitis. Clin J Oncol Nurs. 2016;20(2)187-191.
- Dunn J, Steginga SK, Rose P, et al. Evaluating patient education materials about radiation therapy. Patient Educ Couns. 2004;52(3):325-332.
- Dawdy K, Bonin K, Russell S, et al. Developing and evaluating multimedia patient education tools to better prepare prostate-cancer patients for radiotherapy treatment (randomized study). J Cancer Educ. 2016; Aug 16. [Epub ahead of print].
- Metz JM, Devine P, DeNittis A, et al. A multi-institutional study of Internet utilization by radiation oncology patients. In: Proceedings from the American Society for Therapeutic Radiology and Oncology (ASTRO); November 4-8, 2001; San Francisco, CA.
- Chen X, Siu LL. Impact of the media and the internet on oncology: survey of cancer patients and oncologists in Canada. J Clin Oncol. 2001;19(23): 4291-4297.
- Prabhu AV, Horne Z, Glaser, S et al. YouTube as a source of patient information: assessing quality of information in brachytherapy education videos. Brachytherapy. 2017;16:S95.
- Rosenbergy SA, Francis DM, Hullet CR, et al. Online patient information from radiation oncology departments is too complex for the general population. Pract Radiat Oncol. 2017;7(1):57-62.
- Prabhu AV, Hansberry DR, Agarwal N, et al. Radiation oncology and online patient education materials: deviating from NIH and AMA recommendations. Int J Radiat Oncol Biol Phys. 2016; 96(3):521-528
- Jimenez YA, Lewis SJ. Radiation therapy patient education review and a case study using the Virtual Environment for Radiotherapy Training System. J Med Imag Radiat Sci. Available online 13 September 2017.
- Williams K, Blencowe J, Ind M, Willis D. Meeting radiation therapy patients’ informational needs through educational videos augmented by 3D visualisation software. J Med Radiat Sci. 2017;64:35-40.
- Jimenez YA, Wang W, Stuart K,, et al. Breast cancer patients’ perceptions of a virtual learning environment for pretreatment education. J Cancer Educ. 2017 Feb 10. doi: 10.1007/s13187-017-1183-x. [Epub ahead of print].
- Flockton A. Men’s experience of virtual simulation to aid patient education for radiation treatment to the prostate, J Med Radiat Sci. 2017;48(1)(suppl):S6-S7.
- Marquess M, Johnston SP, Williams NL, et al. A pilot study to determine if the use of a virtual reality education module reduces anxiety and increases comprehension in patients receiving radiation therapy. J Radiat Oncol. 2017;6(3):317-322.|
- Attai DJ, Cowher MS, Al-Hamadani M, et al. Twitter social media is an effective tool for breast cancer patient education and support: patient-reported outcomes by survey. J Med Internet Res. 2015;17(7):e188. doi:10.2196/jmir.4721.
- Langius-Eklöf A, Christiansen M, Lindström V, et al. Adherence to report and patient perception of an interactive app for managing symptoms during radiotherapy for prostate cancer: descriptive study of logged and interview data. JMIR Cancer. 2017;3(2):e18. doi: 10.2196/cancer.7599.
- Clotfelter CE. The effect of an educational intervention on decreasing pain intensity in elderly people with cancer. Oncol Nurs Forum. 1999;26:27-33.
- Jewitt N, Hope AJ, Milne R, et al. Development and evaluation of patient education materials for elderly lung cancer patients. J Cancer Educ. 2016;31(1):70-74.
- Lange M, Rigal O, Clarisse B, et al. Cognitive dysfunctions in elderly cancer patients: A new challenge for oncologists. Cancer Treat Rev. 2014;40(6):810-817.
- Chang M, Kelly AE. Patient education: addressing cultural diversity and health literacy issues. Urolog Nurs. 2007;27(5):411-417; quiz 418.
- Gil S, Hooke MC, Niess D. The limited English proficiency patient family advocate role: fostering respectful and effective care across language and culture in a pediatric oncology setting. J Pediatr Oncol Nurs. 2016;33(3):190-198.
- Valdez A, Napoles AM, Stewart SL, Garza A..A randomized controlled trial of a cervical cancer education intervention for latinas delivered through interactive, multimedia kiosks. J Cancer Educ. 2018;33(1):222-230.
- Siminoff LA, Graham GC, Gordon NH. Cancer communication patterns and the influence of patient characteristics: disparities in information-giving and affective behaviors. Patient Educ Couns. 2006;62(3):355-360.
- Kreps GL. Communication and racial inequities in health care. Am Behav Sci. 2006;49(6):60-774.
- Anderson KO, Mendoza TR, Payne R, et al. Pain education for underserved minority cancer patients: a randomized controlled trial. J Clin Oncol. 2004;22(24):4918-4925.
- Health literacy: report of the Council on Scientific Affairs. Ad Hoc Committee on Health Literacy for the Council on Scientific Affairs, American Medical Association. JAMA.1999;281(6):552-557.
- Treacy JT, Mayer DK. Perspectives on cancer patient education. Semin Oncol Nurs. 2000;16(1):47-56.
Citation
N S. Patient education in radiation oncology: Evolution and innovation. Appl Radiat Oncol. 2018;(1):43-49.
March 23, 2018