Mediastinal Epithelioid Hemangioendothelioma in a Patient With Concurrent Early Stage Right Breast Cancer
Images


CASE SUMMARY
A 47-year-old woman initially presented with cancer in her right breast, detected during screening. A core biopsy was suspicious for intraductal carcinoma. She underwent a guide-wire localized lumpectomy, which unexpectedly showed at least 10 tumors ranging 0.5 to 32 mm, grade 2 invasive ductal carcinoma with positive margins, and no lymphovascular space invasion. Re-excision with sentinel lymph node biopsy achieved clear margins and revealed 1 out of 5 sentinel lymph nodes containing 8 isolated tumor cells. Hormone receptors were strongly positive while HER 2 was 1+ and DISH was negative. The final pathological staging was multifocal pT2N0 (i+).
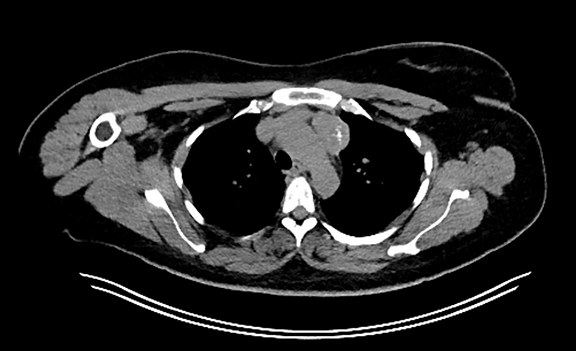
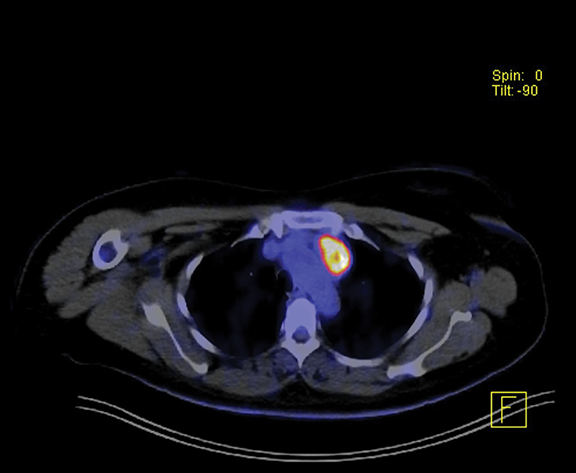
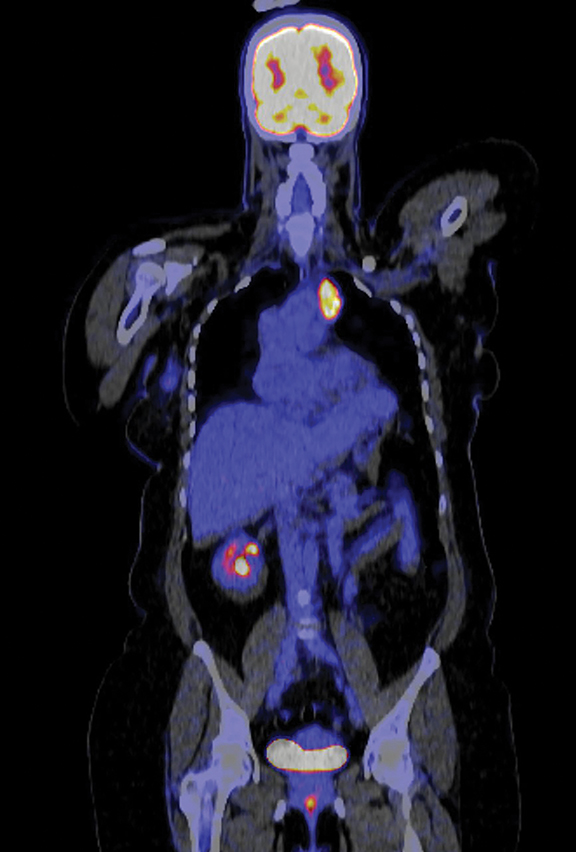
Staging computed tomography (CT) revealed a left anterior mediastinal mass with intense fluorodeoxyglucose (FDG) avidity on subsequent FDG positron emission tomography (PET) (Figure 1 A-C). Tumor markers including alpha-fetoprotein and beta human chorionic gonadotropin were negative. CT-guided biopsy of the mediastinal mass revealed epithelioid hemangioendothelioma (EHE).
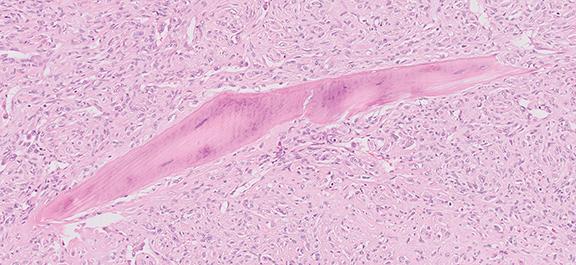
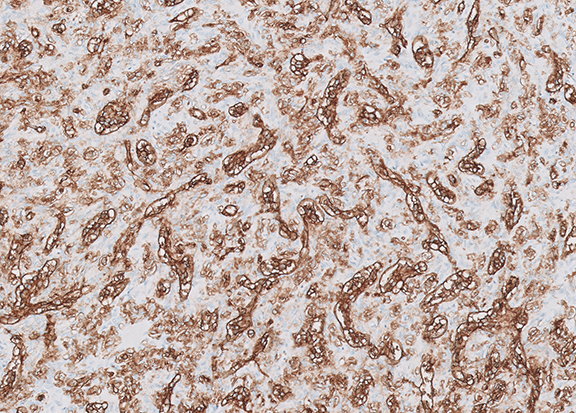
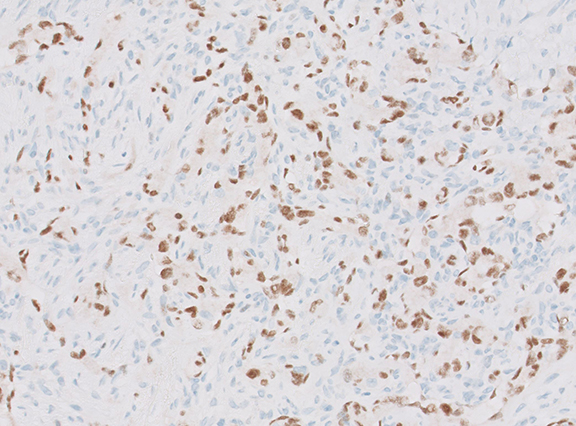
Upper hemisternotomy and en bloc resection revealed involvement of the left brachiocephalic vein and left phrenic nerve. It was suspected on the preoperative imaging, which demonstrated an elevated left hemi-diaphragm with a clinical manifestation in mild dyspnea. Histopathological examination revealed a 45-x-25-mm tumor composed of round to spindle-shaped cells with eosinophilic cytoplasm and intracytoplasmic vacuolation in hyalinized stroma (Figure 2A). The tumor showed positive staining for endothelial and vascular markers CD31, CD34 and ERG on immunohistochemistry (Figure 2B and 2C). The tumor cells exhibited 4 mitoses per 50 high-power field with no severe atypia. There were no features of an epithelioid angiosarcoma.
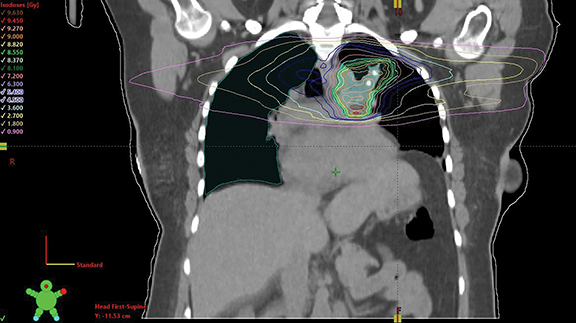
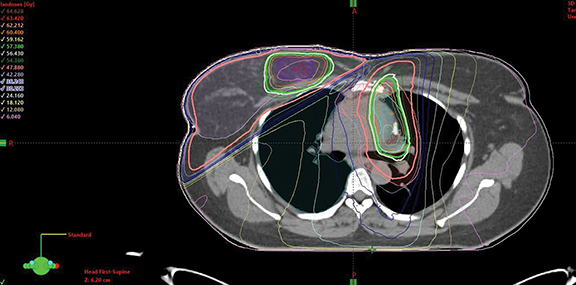
Due to the prolonged time post breast surgery and the need for adjuvant radiation therapy (RT) for both EHE and breast cancer, adjuvant chemotherapy for breast cancer was omitted and endocrine therapy was initiated. Complex planning of adjuvant RT to two adjacent anatomical sites with two distinct malignancies was undertaken using 2-dimensional (2D) tangential and partial arc volumetric-modulated arc therapy (VMAT). Phase I delivered 50.4 Gy in 28 fractions to the right breast and anterior mediastinum. Phase II delivered further 10 Gy in 5 fractions to the surgical cavity in the breast and 9 Gy in 5 fractions to the surgical bed within the anterior mediastinum.
IMAGE FINDINGS
CT/FDG-PET revealed a well-defined 3.8-×-2.3-cm partially calcified soft-tissue mass in the left anterior upper mediastinum with a standard uptake value max of 11.1 (Figure 1).
DIAGNOSIS
EHE with R0 resection and multifocal pT2N0 (i+) right breast cancer (ER 90%, PR 95%, HER2 DISH negative)
DISCUSSION
EHE is a rare malignant vascular tumor representing < 1% of all vascular tumors and has been reported to occur in a variety of locations including the mediastinum, head and neck, lungs, liver, breast and bone.1-3 EHE is composed of epithelioid endothelial cells with distinctive myxohyaline stroma and a characteristic WWTR1-CAMTA1 fusion as described in the 2013 WHO classification.3 Although reported rates of recurrence, metastasis and tumor-related death vary, most soft-tissue EHE has an indolent course in contrast to angiosarcoma.4,5 EHE involving soft-tissue sites have overall better prognosis than skeletal, hepatic or pulmonary EHE.6
Due to its rarity, there are no management guidelines for EHE. Surgical excision is generally considered first if lesions are localized and surgically resectable with functional preservation and acceptable morbidity.1 Adjuvant RT has been utilized to reduce the risk of local recurrence. With more recent advancements in radiation delivery techniques, definitive RT use has increased.7 Optimal dose and fractionation for resected and unresected EHE still remain controversial, and various RT protocols have been described.7-12
A case described by Drazin et al9 delivered adjuvant RT to a total dose of 59.4 Gy in 33 fractions for subtotally resected recurrent EHE of the mastoid, and the patient was alive with no evidence of recurrence at 8 years.
Scott et al7 reviewed 14 patients with hemangioendothelioma treated with RT at a single institution. Surgical resection followed by postoperative RT (PORT) was performed in 4 patients while 10 received definitive RT. The median dose for PORT was 62.2 Gy (range 60 to 64.8 Gy). Two patients were treated with 60 Gy in 30 fractions while the other two were treated using a hyperfractionated approach of 1.2 Gy twice daily to a total dose of 64.8 Gy. None of the 4 patients showed recurrent disease over their follow-up periods, ranging 5.1 to 28 years.
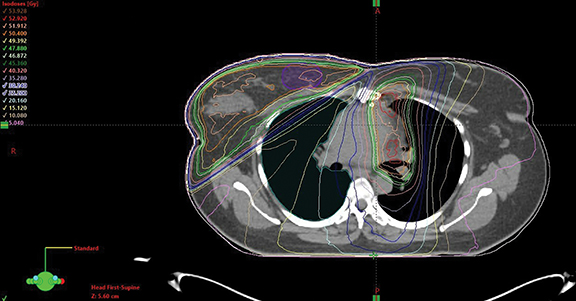
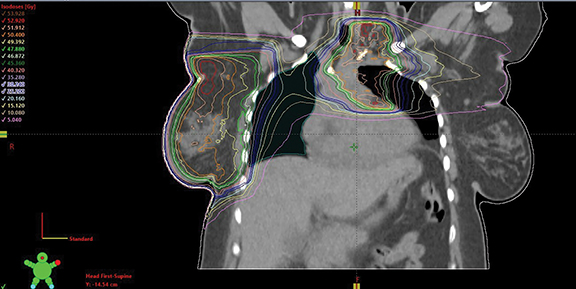
Our case presented additional complexity in treatment planning due to the concurrent adjuvant RT aimed for right breast cancer. Phase I was planned with a 2D-tangential technique for the right breast and partial-arc volumetric-modulated arc therapy (VMAT) technique for the mediastinum using 10 MV photons and delivering 50.4 Gy. Phase II utilized 12 MeV electron beams for the breast boost, delivering an additional 10 Gy in 5 fractions. The partial-arc VMAT technique was again used for the mediastinal boost volume, delivering another 9 Gy in 5 fractions. Acceptable coverage of planning target volumes was achieved (Figure 3). Mean doses of esophagus, heart and lung were 25.4 Gy, 7.3 Gy (V25 < 10%), and 17 Gy, respectively, achieving their dose constraints. Dose constraints also were met for the spinal cord and bilateral brachial plexuses.
The patient completed adjuvant RT to her right breast and mediastinum with moderate toxicities including skin erythema and desquamation of her right breast and moderate odynophagia. She recovered from these toxicities approximately 1 month after RT. Our patient remained well with no clinical or radiological evidence of recurrence at 12 months after completion of adjuvant RT. She will continue ongoing surveillance for both EHE and breast cancer.
CONCLUSION
In conclusion, we have presented the management of a patient with mediastinal EHE in the presence of concurrent early stage breast cancer. Our patient received adjuvant RT to the mediastinum and right breast concurrently. We have outlined the complex planning for radiation therapy to 2 adjacent anatomical sites. While some evidence suggests the benefit of adjuvant RT to improve local control, heterogeneous dose and fractionation regimens are reported for EHE. Future collaborative studies are needed to further define the role, dose and fractionation of PORT for EHE with active participation in rare cancer databases such as Rare Cancer Australia, European RareCareNet, and the US-based rarediseases.org.
REFERENCES
- Sardaro A, Bardoscia L, Petruzzelli MF, et al. 1pithelioid hemangioendothelioma: an overview and update on a rare vascular tumor. Oncol Rev. 2014;8(2):259.
- Weiss SW, Enzinger FM. Epithelioid hemangioendothelioma: a vascular tumor often mistaken for a carcinoma. Cancer. 1982;50(5):970-981.
- Bridge J, Hogendoorn P. WHO Classification of Tumours of Soft Tissue and Bone. Lyon: International Agency for Research on Cancer (IARC) (UN); 2013. p155.
- Mentzel T, Beham A, Calonje E, et al. Epithelioid hemangioendothelioma of skin and soft tissues: clinicopathologic and immunohistochemical study of 30 cases. Am J Surg Pathol. 1997;21(4):363-374.
- Weiss SW, Ishak KG, Dail DH et al. Epithelioid hemangioendothelioma and related lesions. Semin Diagn Pathol. 1986;3(4):259-287.
- Habeeb O, Rubin BP. The molecular diagnostics of vascular neoplasms. Surg Pathol Clin. 2019;12(1):35-49.
- Scott M, Indelicato D, Morris C, et al. Radiation therapy for hemangioendothelioma: the University of Florida experience. Am J Clin Oncol. 2014; 37(4):360-363.
- Van Kasteren MEE, van der Wurff AAM, Miserè JFMM, et al. Epithelioid hemangioendothelioma of the lung: clinical and pathological pitfalls. Eur Respir J. 1995;8:1616-1619.
- Drazin D, Gandhi R, Boulos AS, et al. Epithelioid hemangioendothelioma of the mastoid: resection for recurrence and adjuvant radiation with 8-year follow up. Case Rep Surg. 2013;2013:469201.
- Gherman CD, Fodor D. Epithelioid hemangioendothelioma of the forearm with radius involvement. Case report. Diagn Pathol. 2011;6:120.
- Aquilina K, Lim C, Keohane C, et al. Epithelioid hemangioendothelioma of the spine. J Neurosurg Spine. 2005;3:393-399.
- Schattenberg T, Kam R, Pfannschmidt J, et al. Pulmonary epithelioid hemangioendothelioma: report of three cases. Surg Today. 2008;38:844-849.
Citation
M B, Z A, M B, P S, A P. Mediastinal Epithelioid Hemangioendothelioma in a Patient With Concurrent Early Stage Right Breast Cancer. Appl Radiat Oncol. 2020;(4):52-55.
December 24, 2020