Health Disparities in Radiation Oncology: Our Call to Action
Images
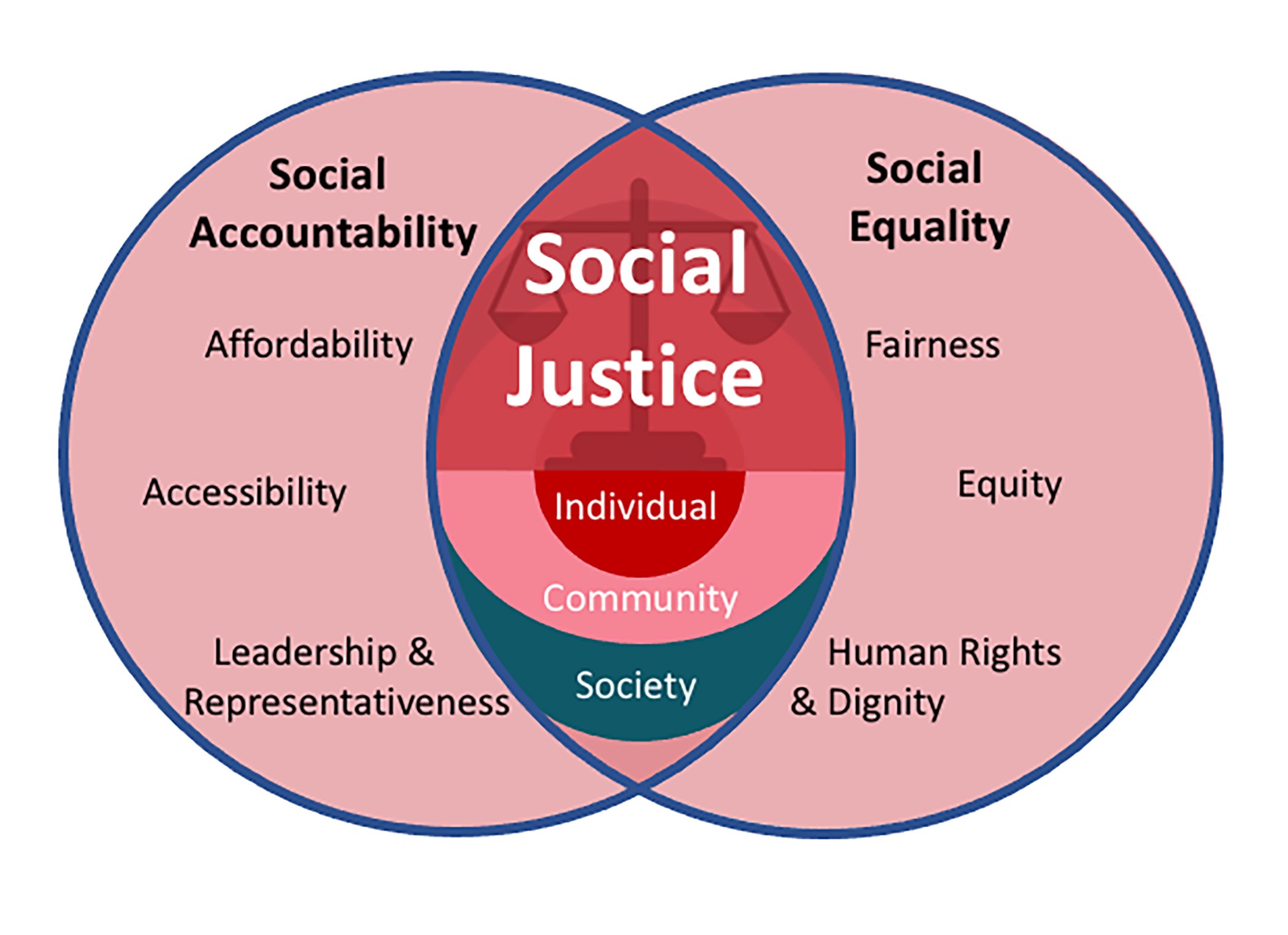
Radiation oncology has made tremendous strides to establish itself as a vital discipline for the cure and palliation of cancer. However, as society has demonstrated increasing demands for fairness, equity, and dignity, we have lagged behind the forefront of these movements. Historically, our social accountability has been to those with means for the right care. From the perspective of the next generation of clinicians, we attempt to address these disparities and highlight potential ways our specialty can experience progress in these domains moving forward.
Financial Toxicity: When Less Really Can Be More
Increasing financial costs for our treatments, especially for our most vulnerable patients, limits quality of life, compliance, and survival.1,2 Financial toxicity (FT) impacts multiple domains by hindering ability to access medications, attend appointments, afford living expenses, and adhere to recommendations for care. This disproportionately impacts patients with cancer3 and nearly 1 in 6 undergoing radiation therapy (RT) experience moderate or severe FT.4,5 FT follows racial and ethnic divides – 1 in 20 Black or Latina women with early stage breast cancer lose their home as a consequence and nearly half of these patients cut back on basic needs such as food.6 Simple solutions may go a long way toward bridging this gap, starting at measuring the problem and increasing FT awareness for patients and providers.1 More dynamic interventions can include increased cost transparency and accessibility to financial counseling, as well as sustainable policies to incentivize cost reduction.
Improving Access to Quality Care
Financial cost may only be the tip of the iceberg – there are also large disparities in the delivery of quality cancer care. African Americans with prostate cancer experience a longer time from diagnosis to treatment, even after controlling for socioeconomic factors.7 Palliative care, integral to quality cancer care, is disproportionately utilized by Black patients who are 20% to 30% less likely to receive palliative RT.8 Black pediatric patients are also less likely to receive proton therapy, despite equal enrollment in national prospective trials.9 These data highlight that systemic and structural racism ingrained in society is experienced by our patients throughout the spectrum of cancer care.
Moreover, other socioeconomic barriers impede quality cancer care. It has been well-established that rural and remote communities have decreased rates of RT utilization;10 however, even urban urban populations lack access to newer technologies, especially among those with less insurance, lower socioeconomic status, and less education.11 In the realm of research, younger, poorer, underinsured, non-White patients are underrepresented in cancer trial enrollment.12 Dishearteningly, African American and Hispanic cancer trial enrollment has actually decreased over the past several decades.13 Potential avenues to solvency include expanding trial access to underrepresented communities, guaranteeing insurance coverage for all standard-of-care treatment, and responsible financial incentives and assistance to defray costs. A targeted increase in accessibility to patient navigation programs has also shown promise in achieving quality cancer care.14
Leading Change
A diverse oncology workforce helps meet the complex needs of all Americans. Regrettably, diversity within our specialty does not reflect the populations we need to serve. The gender gap and its drivers continue to be an issue as women persistently face an uphill climb toward gender equity.15 Underrepresented minorities (URMs) are also underrepresented in radiation oncology at the trainee (6.9%) and faculty levels (7.2% to 8.1%).16.17 This is critical because racial and ethnic representativeness improves outcomes.18 African American patients treated by physicians of the same race have more active shared decision making and improved overall satisfaction.19 Similar results are seen among Latinx20 and indigenous communities.21 In addition, sociocultural-based programs involving Native Hawaiian physicians that leveraged shared language, culture, and values forged strong patient-physician relationships and improved cancer screening in rural and medically underserved areas.22
Ethnic and racial differences between physician and patient are well-defined barriers to care. Implicit bias may unintentionally dictate their relationship and undermine trust.18 Well-intentioned providers have unknowingly incorporated their biases to limit person-centered care. Although the evidence base is growing for the benefit of increasing URMs in oncology, many groups are left out including LGBTQ populations and individuals with disabilities. Cultural sensitivity can be adopted through recruitment and retention with pipeline programs, but also inculcated through conscientious unlearning to eliminate unconscious bias. This grassroots effort will also require proactive development and recognition of diverse faculty and young leaders at all levels.
The Way Forward
Cancer control can only be achieved for all by addressing health disparities. For our most vulnerable populations, there are interventions that no medication, radiation treatment, or technology can achieve, yet will have the unseen impact of strengthening our society. We must demand more social accountability from our policy makers, institutions, and ourselves. We must create solutions that address it at its roots including affordability, accessibility, and lack of leadership and representativeness in our workforce. Social justice in radiation oncology is not achieved until we achieve social accountability and social equality for all.
References
- Chino F. My unfortunate introduction into the financial toxicity of cancer care in America-march forth. JAMA Oncol. 2018;4(5):628-629. doi:10.1001/jamaoncol.2017.4436
- de Souza JA, Yap BJ, Wroblewski K, et al. Measuring financial toxicity as a clinically relevant patient-reported outcome: the validation of the COmprehensive Score for financial Toxicity (COST). Cancer. 2017;123(3):476-484. doi:10.1002/cncr.30369
- Bernard DS, Farr SL, Fang Z. National estimates of out-of-pocket health care expenditure burdens among nonelderly adults with cancer: 2001 to 2008. J Clin Oncol. 2011;29(20):2821-2826. doi:10.1200/JCO.2010.33.0522
- D’Rummo KA, Miller L, TenNapel MJ, Shen X. Assessing the financial toxicity of radiation oncology patients using the validated comprehensive score for financial toxicity as a patient-reported outcome. Pract Radiat Oncol. 2020;10(5):e322-e329. doi:10.1016/j.prro.2019.10.005
- Palmer JD, Patel TT, Eldredge-Hindy H, et al. Patients undergoing radiation therapy are at risk of financial toxicity: a patient-based prospective survey study. Int J Radiat Oncol Biol Phys. 2018;101(2):299-305. doi:10.1016/j.ijrobp.2018.03.014
- Jagsi R, Ward KC, Abrahamse PH, et al. Unmet need for clinician engagement regarding financial toxicity after diagnosis of breast cancer. Cancer. 2018;124(18):3668-3676. doi:10.1002/cncr.31532
- Stokes WA, Hendrix LH, Royce TJ, et al. Racial differences in time from prostate cancer diagnosis to treatment initiation: a population-based study. Cancer. 2013;119(13):2486-2493. doi:10.1002/cncr.27975
- Murphy JD, Nelson LM, Chang DT, Mell LK, Le QT. Patterns of care in palliative radiotherapy: a population-based study. J Oncol Pract. 2013;9(5):e220-e227. doi:10.1200/JOP.2012.000835
- Bitterman DS, Bona K, Laurie F, et al. Race disparities in proton radiotherapy use for cancer treatment in patients enrolled in children’s oncology group trials. JAMA Oncol. Published online August 06, 2020. doi:10.1001/jamaoncol.2020.2259
- Gillan C, Briggs K, Goytisolo Pazos A, et al. Barriers to accessing radiation therapy in Canada: a systematic review. Radiat Oncol. 2012;7:167. doi:10.1186/1748-717X-7-167
- Shen CJ, Hu C, Ladra MM, Narang AK, Pollack CE, Terezakis SA. Socioeconomic factors affect the selection of proton radiation therapy for children. Cancer. 2017;123(20):4048-4056. doi:10.1002/cncr.30849
- Chino F, Zafar SY. Financial toxicity and equitable access to clinical trials. Am Soc Clin Oncol Educ Book. 2019;39:11-18. doi:10.1200/EDBK_100019
- Duma N, Vera Aguilera J, Paludo J, et al. Representation of minorities and women in oncology clinical trials: review of the past 14 years. J Oncol Pract. 2018;14(1):e1-e10. doi:10.1200/JOP.2017.025288
- Rodday AM, Parsons SK, Snyder F, et al. Impact of patient navigation in eliminating economic disparities in cancer care. Cancer. 2015;121(22):4025-4034.
- Holliday EB, Siker M, Chapman CH, et al. Achieving gender equity in the radiation oncology physician workforce. Adv Radiat Oncol. 2018;3(4):478-483.
- Deville C, Hwang WT, Burgos R, Chapman CH, Both S, Thomas CR Jr. Diversity in graduate medical education in the United States by race, ethnicity, and sex. JAMA Intern Med. 2015;175(10):1706-1708. doi:10.1001/jamainternmed.2015.4324
- Chapman CH, Hwang WT, Deville C. Diversity based on race, ethnicity, and sex, of the US radiation oncology physician workforce. Int J Radiat Oncol Biol Phys. 2013;85(4):912-918. doi:10.1016/j.ijrobp.2012.08.020
- Cooper-Patrick L, Gallo JJ, Gonzales JJ, et al. Race, gender, and partnership in the patient-physician relationship. JAMA. 1999;282(6):583-589. doi:10.1001/jama.282.6.583
- Johnson RL, Roter D, Powe NR, Cooper LA. Patient race/ethnicity and quality of patient-physician communication during medical visits. Am J Public Health. 2004;94(12):2084-2090. doi:10.2105/ajph.94.12.2084
- Mitchell JA, Perry R (2020) Disparities in patient-centered communication for Black and Latino men in the U.S.: cross-sectional results from the 2010 health and retirement study. PLoS ONE15(9) e0238356. doi:10.1371/journal.pone.0238356
- Guadagnolo BA, Cina K, Helbig P, et al. Medical mistrust and less satisfaction with health care among Native Americans presenting for cancer treatment. J Health Care Poor Underserved. 2009;20(1):210-226. doi:10.1353/hpu.0.0108
- Gellert K, Braun KL, Morris R, Starkey V. The ‘Ohana Day Project: a community approach to increasing cancer screening. Prev Chronic Dis. 2006;3(3):A99.
Citation
AR C, R B, MC L, K T, I F, A G, B L, IJ P. Health Disparities in Radiation Oncology: Our Call to Action. Appl Radiat Oncol. 2020;(4):6-8.
December 24, 2020