Gene Blocks Progression of AML in Mice
 An early-stage study by experts from Cincinnati Children’s Hospital, NYU and Japan has found that the gene TRAF6 can block progression from pre-leukemia to acute myeloid leukemia (AML).
An early-stage study by experts from Cincinnati Children’s Hospital, NYU and Japan has found that the gene TRAF6 can block progression from pre-leukemia to acute myeloid leukemia (AML).
Daniel Starczynowski, PhD, a cancer research expert at Cincinnati Children's, along with research teams around the globe, has been hunting for years to find ways to improve the odds of surviving AML. While nearly 70% of children with AML survive at least five years, the five-year survival rate for adults lingers at a disappointing 26%.
Based on discoveries he published in 2019, the start-up company Kurome Therapeutics was launched to pursue new ways to prevent AML from adapting so easily to existing chemotherapies. Now, a new study in collaboration with Iannis Aifantis, PhD, and his team at NYU, published Jan. 18, 2022, in Cell Stem Cell, sheds even more light on the chain reactions that can lead from a state of pre-leukemia to full-blown disease.
A large number of scientists have described how people can acquire gene mutations in blood-forming cells during their lives that lack initial evidence of disease but make them increasingly likely to develop AML. These precursor conditions have been described as clonal hematopoiesis of indeterminant potential – "CHIP." However, much has remained unknown about exactly how CHIP becomes full-blown leukemia.
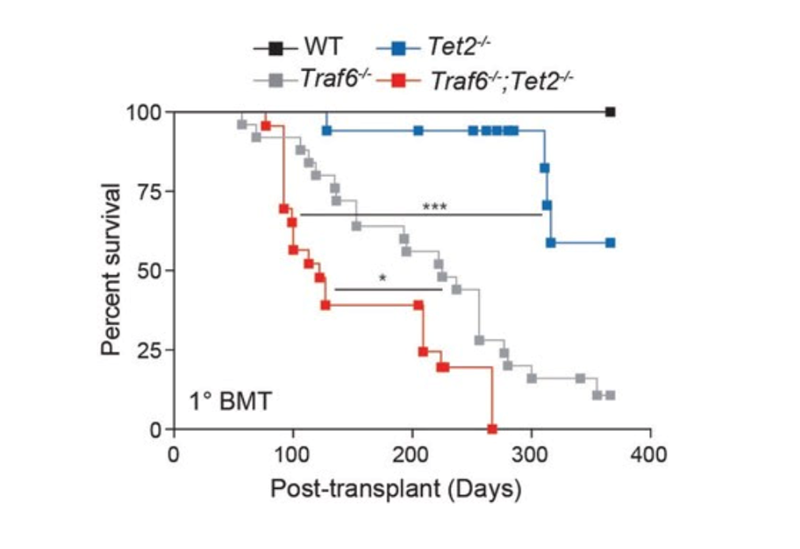
The new study reports that the gene TRAF6 plays a crucial—and unexpected—cancer-regulating role amid a complex set of interactions between cellular mechanisms that govern blood cell production and innate immune-related pathways, including toll-like receptors (TLR). Too much TRAF6 activity can lead to certain types of cancer risk. Not enough TRAF6 activity clearly increases the risk of developing myeloid malignancies, such as myelodysplastic syndromes (MDS) and certain subtypes of AML. Having a balanced level of activity prevents the disease, and restoring that balance appears to improve survival once the disease appears—at least in mice.
"The role of TRAF6 has been investigated for its role in immune cell biology. However, more recently it has come to the forefront as a complex and key player in cancer. Some research indicates that it acts as a tumor suppressor, while others have reported that it can cause cancer," Dr. Starczynowski says. "Our findings confirm that TRAF6 can, in fact, have opposite effects depending on the context of its environment. But we also found that its activity can be regulated through activation of certain toll-like receptors – evolutionarily conserved pathogen detectors in our immune systems that have been hijacked by the AML cell."
The new information, based on an extensive series of mouse studies, remains in the early stages. Potential novel therapies and clinical trials based on these finding remain years away.
However, the research team has identified novel mechanisms underlying the stepwise progression of certain subtypes of AML, and in doing so may have zeroed in on a gene target that could bring the emerging field of inflammation-targeted therapies to bear against a notoriously hard-to-treat condition.
"Our current studies primarily focused on mouse models, however more extensive work on human AML is warranted," Dr. Starczynowski says. "Moreover, we are now launching into a series of experiments to help us understand the mechanistic basis for why TRAF6 can function both as a tumor suppressor and an oncogene. Through these studies, we hope to uncover novel therapeutic opportunities that will exploit the unique functions of TRAF6 in myeloid malignancies."