Delayed Radiation-Therapy-Induced Cerebral Demyelination
Images


Case Summary
A 41-year-old man with no significant medical history presented to the emergency department with new persistent headache. The examination was notable for acromegalic features and right homonymous superior quadrantanopia. A brain MRI scan and laboratory findings were suggestive of growth hormone-secreting pituitary macroadenoma. A 2-stage neurosurgical approach was completed without periprocedural complications. The final diagnosis was consistent with a prolactin and growth hormone-secreting pituitary macroadenoma (Ki67 labeling index 3%). Due to invasive adenoma with residual disease, intensity-modulated radiation therapy was started 4 months after the second surgery, following an informed discussion with the patient (total dose of 5040 cGy in 28 fractions with good tolerance). Three months later, the patient developed vertical diplopia, decreased sensation in the left lower face, slurred speech, tongue numbness, and bilateral upper extremity ataxia. The patient refused hospitalization, but subsequently developed left-sided hemiparesis and was admitted. An updated examination showed dysarthria, binocular horizontal nystagmus in right lateral gaze, decreased hearing on the left, left uvular deviation, decreased elevation of the palate on the right, left tongue deviation, diffuse mild left arm weakness, and left arm ataxia. No vessel abnormalities were noted on head and neck computed tomography (CT) angiography, but a brain MRI scan was showing interval new multifocal lesions. A lumbar puncture was performed, and analyses showed pleocytosis (13 leukocytes per µL), predominantly mature lymphocytes on cytology, and mild protein elevation (50 mg /dL). Oligoclonal bands were not detected, and the IgG index value was 0.64 (0.00-0.61 as normal range). Additional tests including antinuclear antibody; extractable nuclear antigen antibodies panel; c- and p-antineutrophil cytoplasmic antibodies; complement components 3 and 4; C-reactive protein; hepatitis viral panel; blood cultures; spinal fluid bacterial, parasite, viral, and fungal analyses; human immunodeficiency virus panel; and toxoplasma antibodies were performed, but all were unrevealing of abnormalities. A contrasted chest, abdomen, and pelvis CT scan did not show concerning lesions. Ultimately, a stereotactic brain biopsy of right cerebellar hemispheric lesions was performed. Findings were suggestive of a noninfectious inflammatory process compatible with acute demyelination. Notably, family history was unremarkable for autoimmune or demyelinating diseases. Pulse intravenous methylprednisolone (1g/day) was given for 3 consecutive days, followed by oral dexamethasone (4 mg twice daily).
Imaging Findings
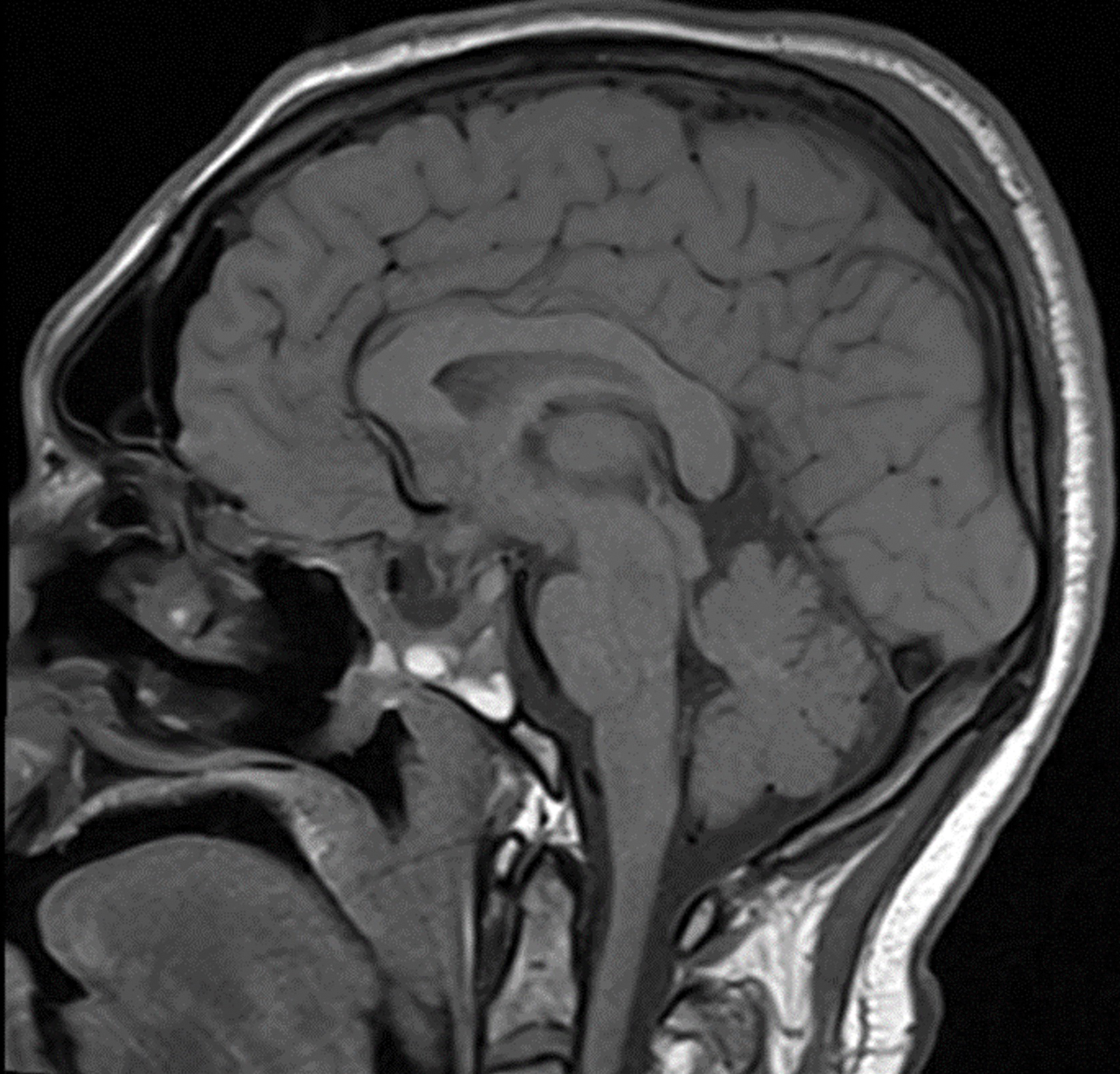
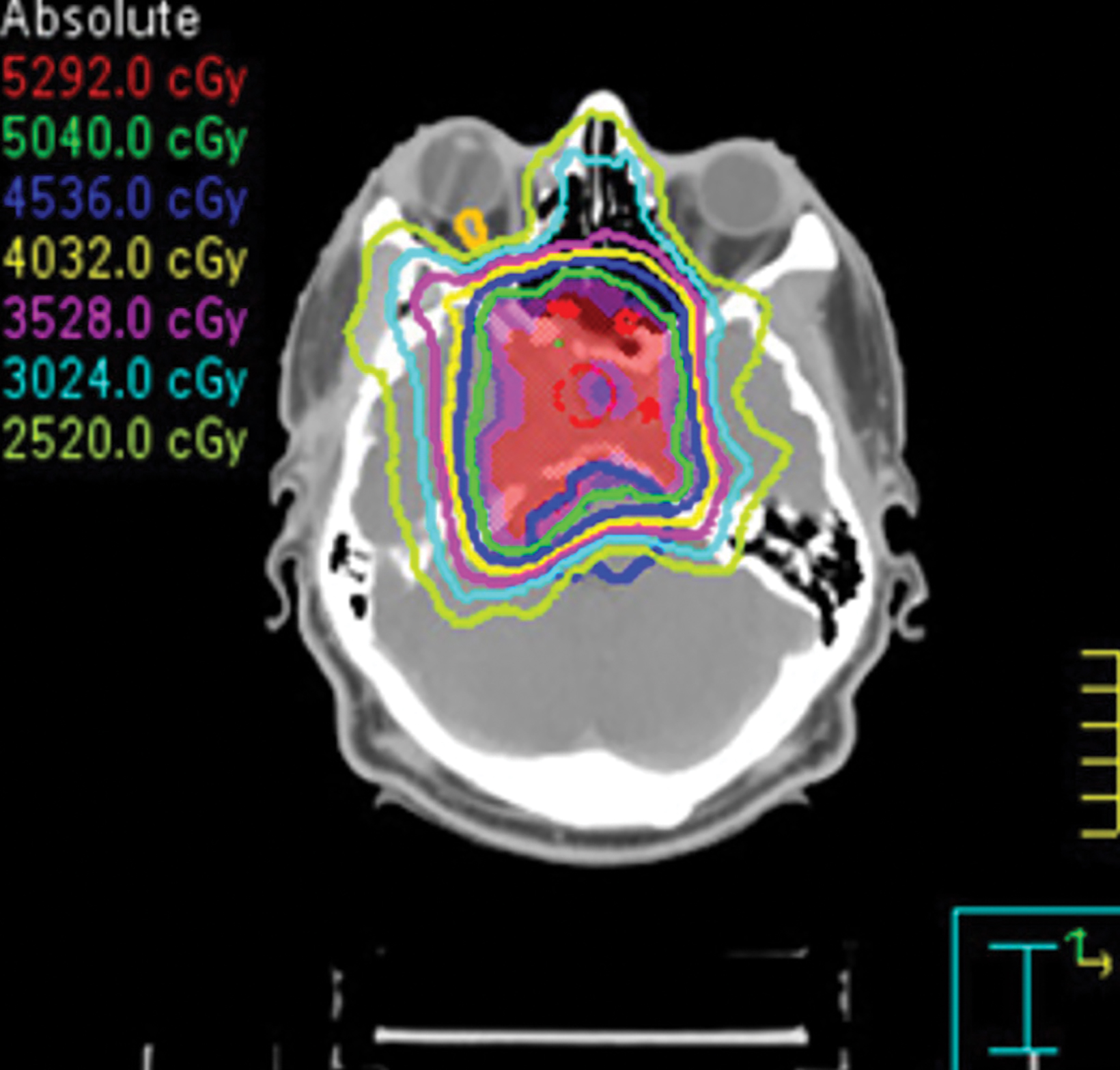
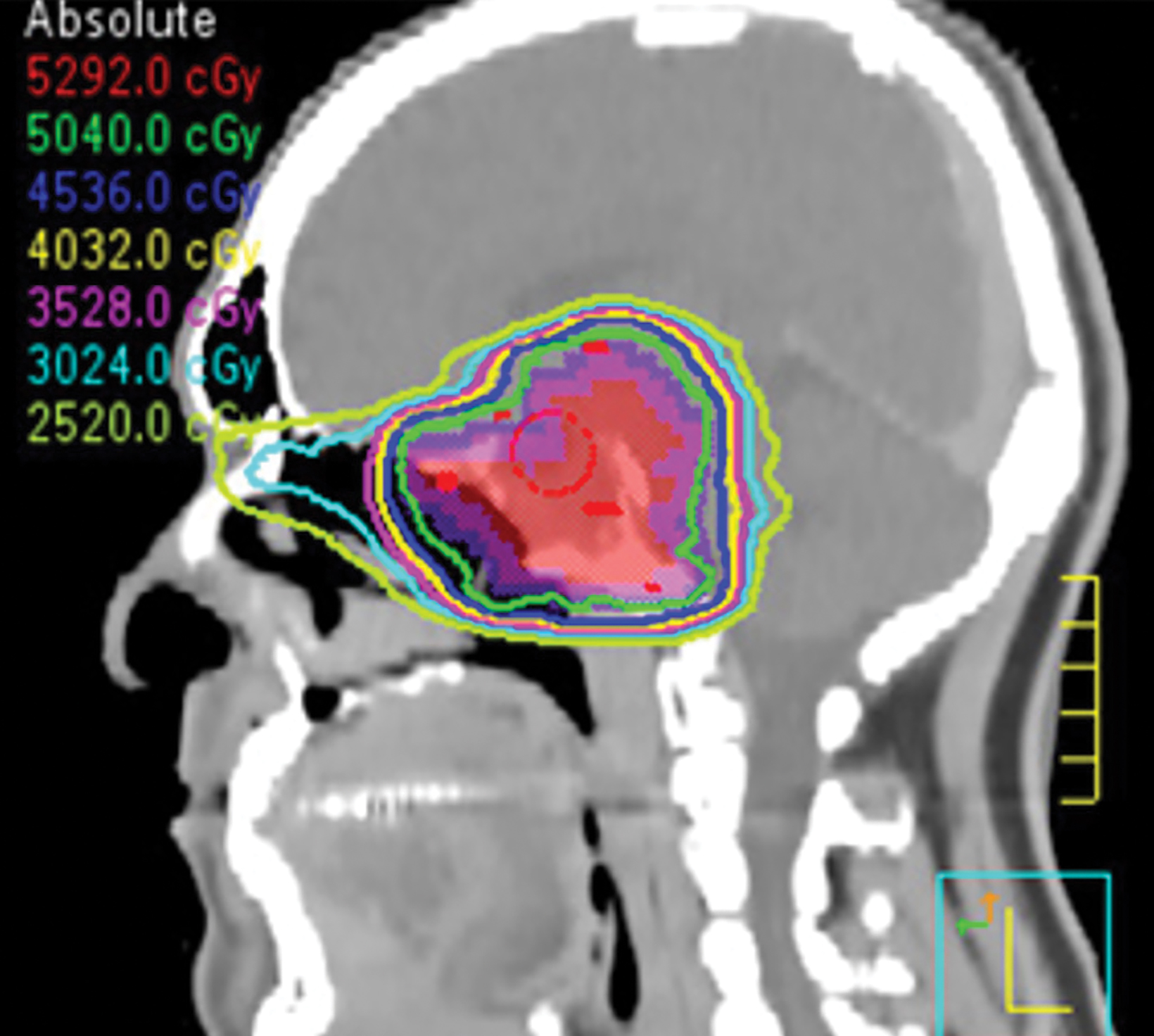
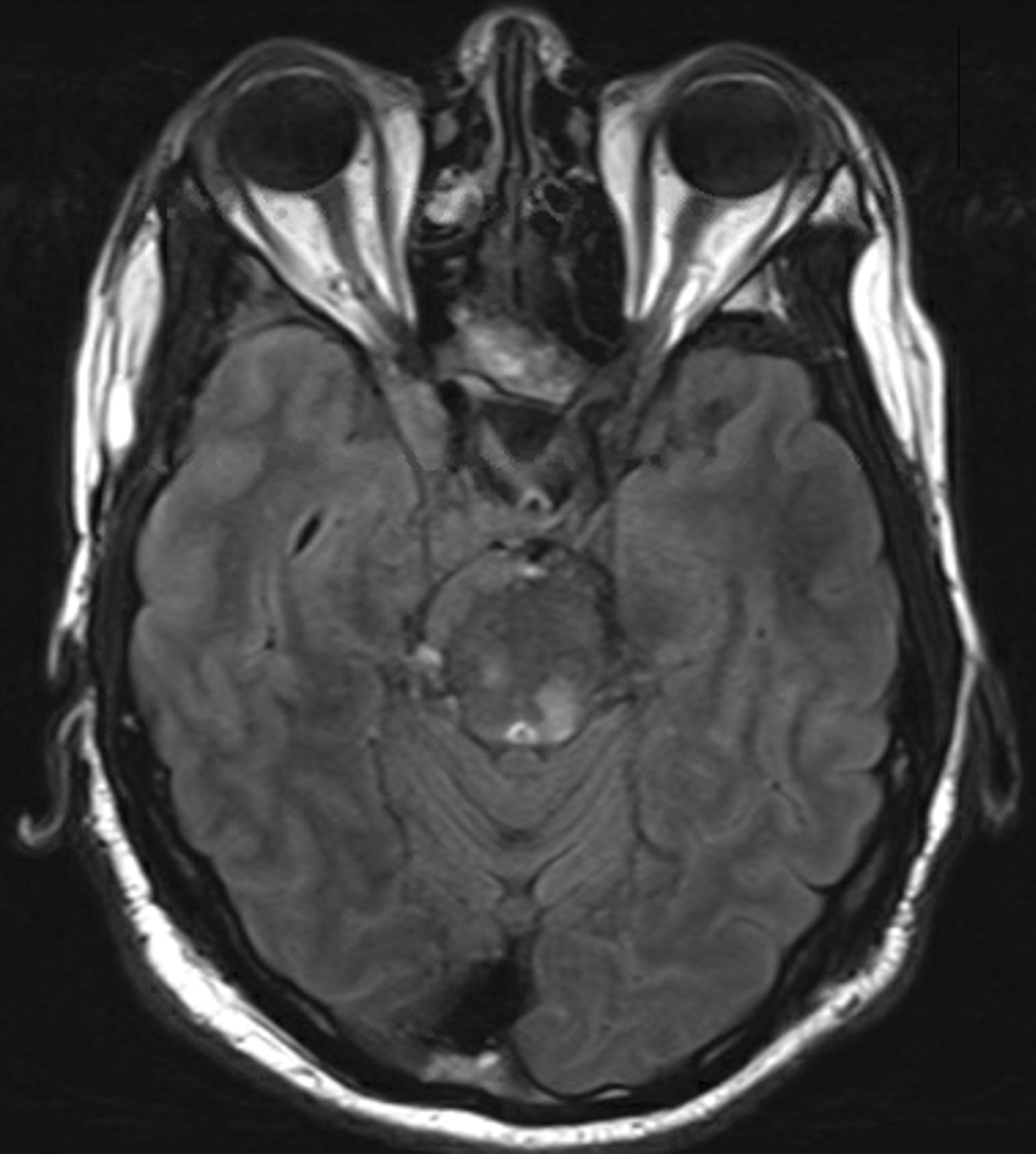
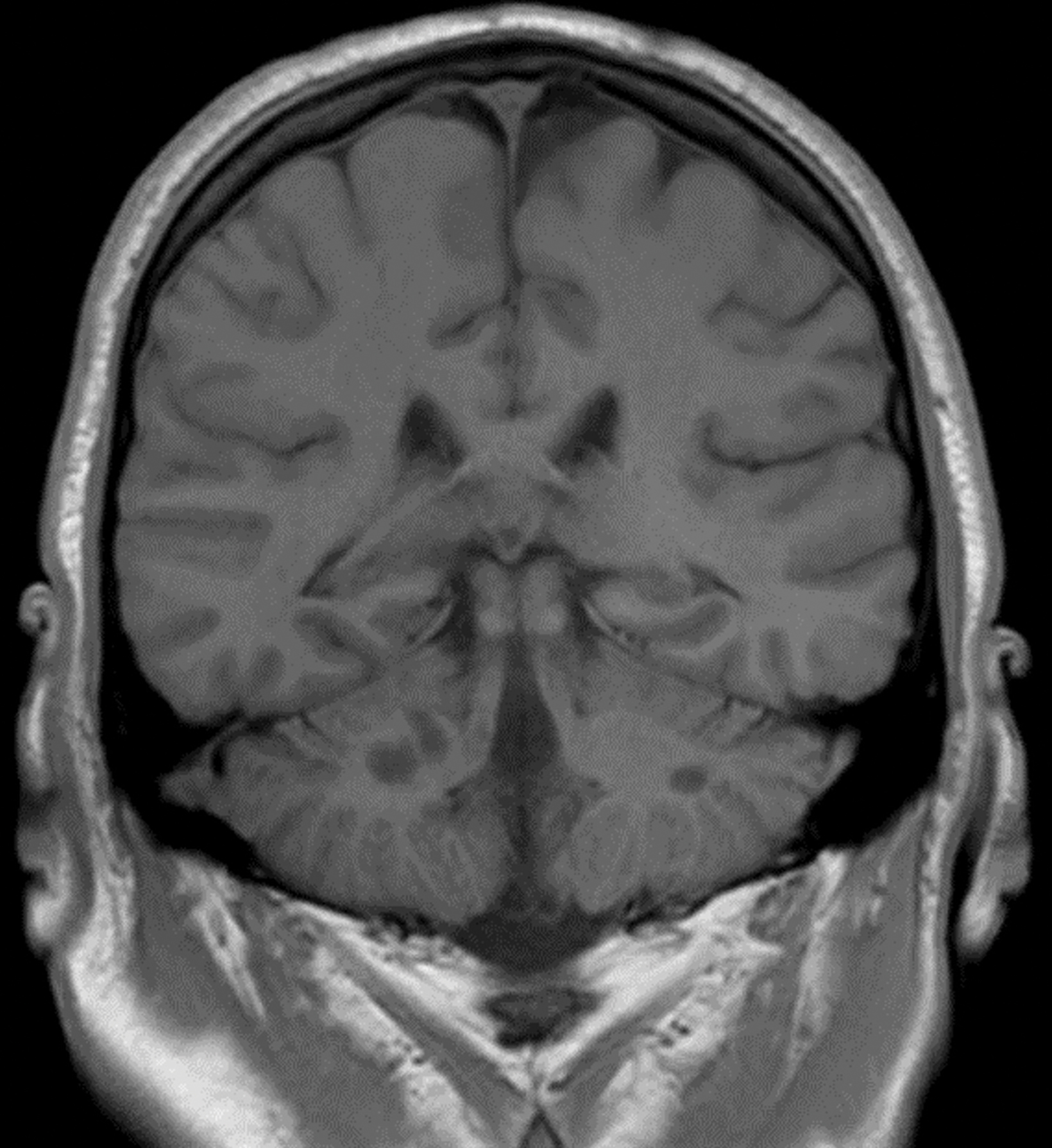
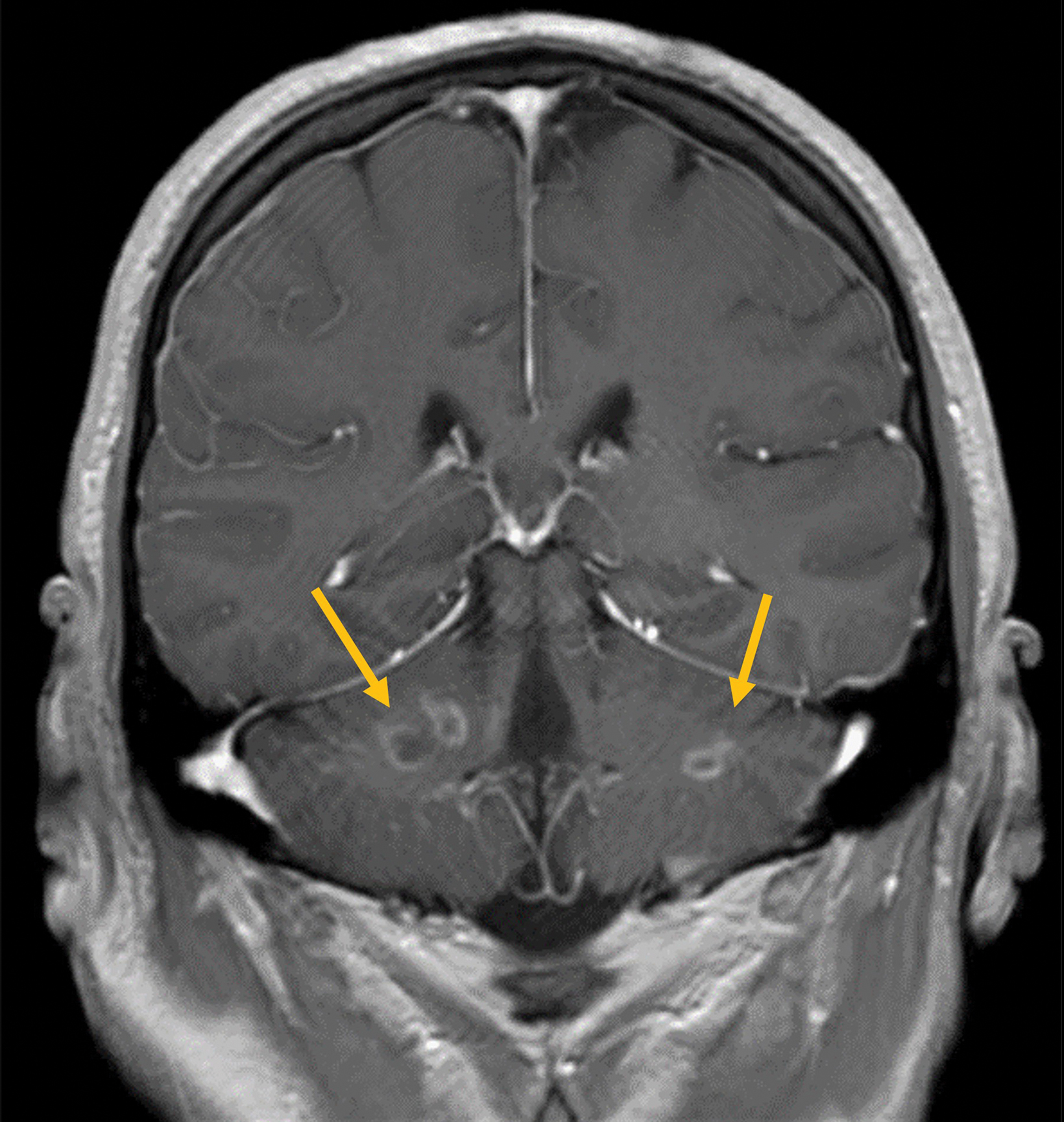
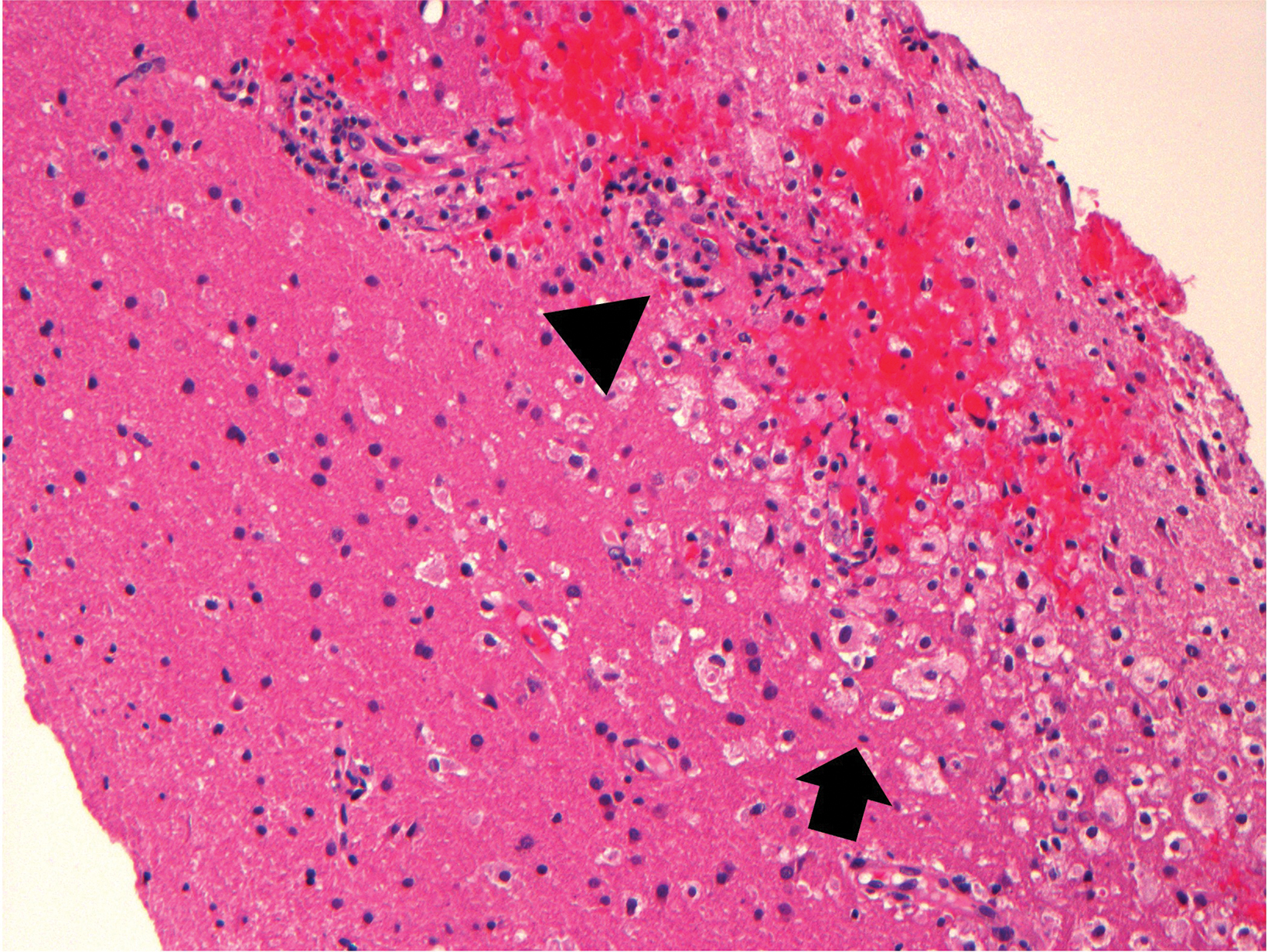
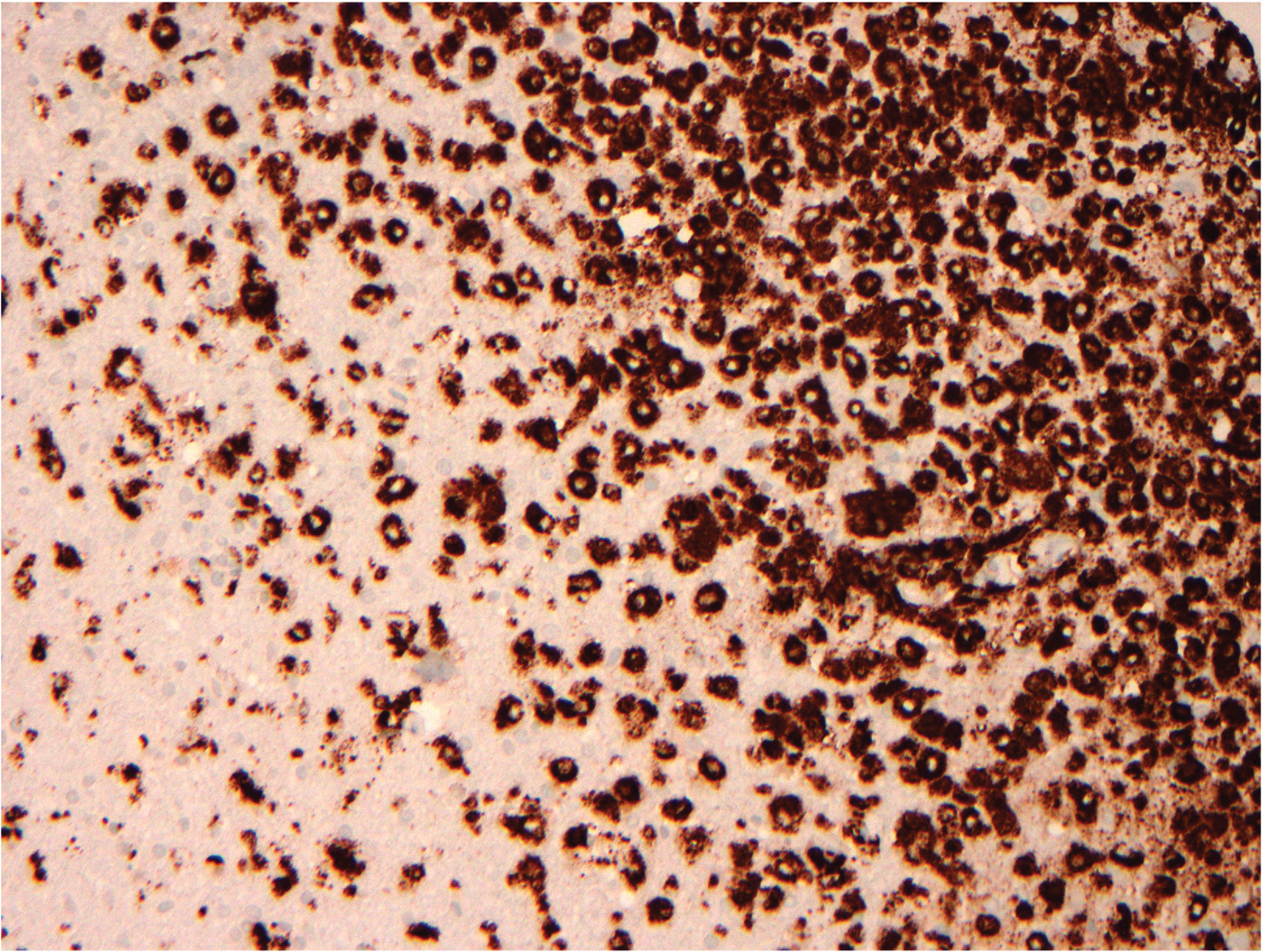
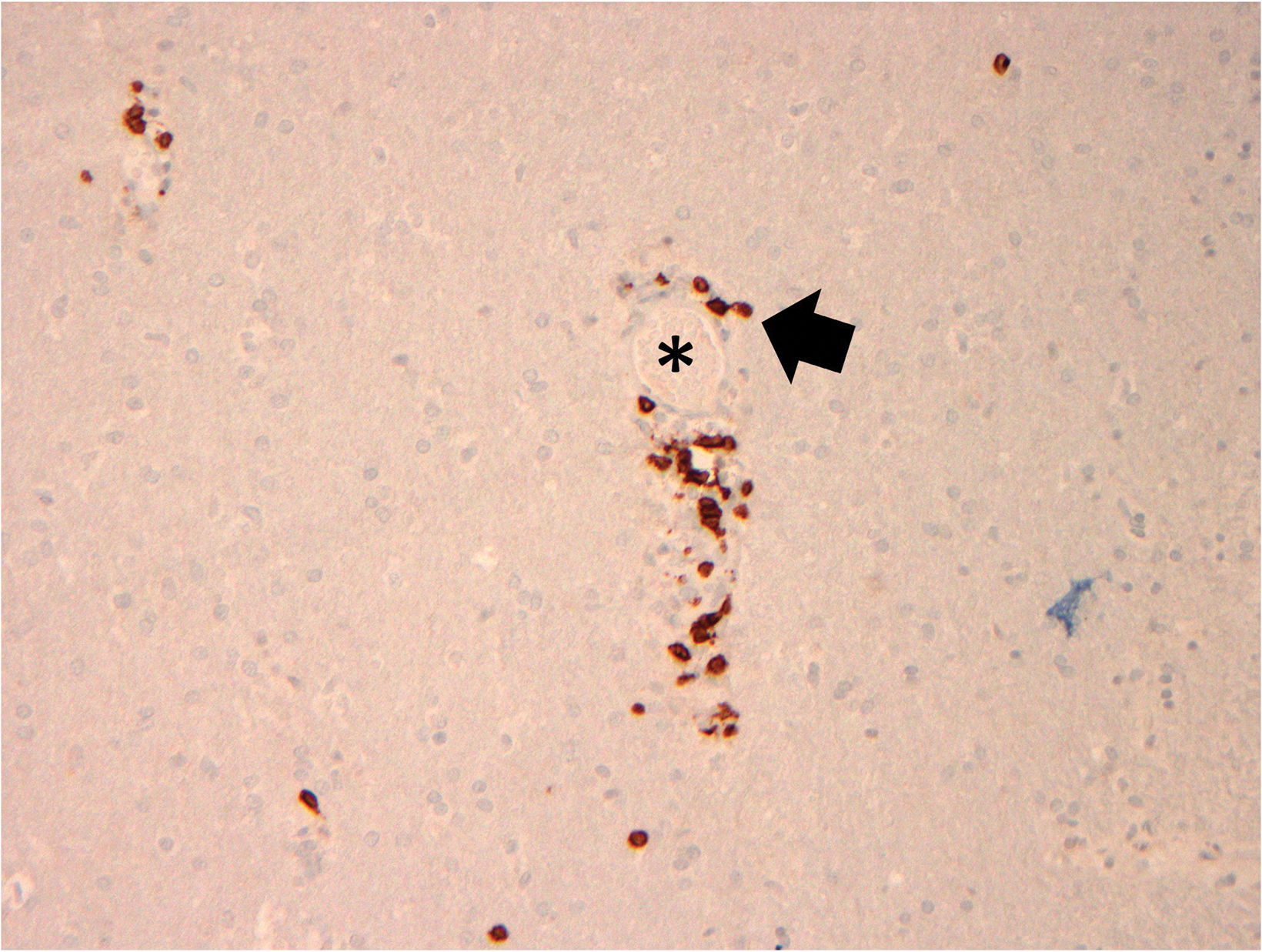
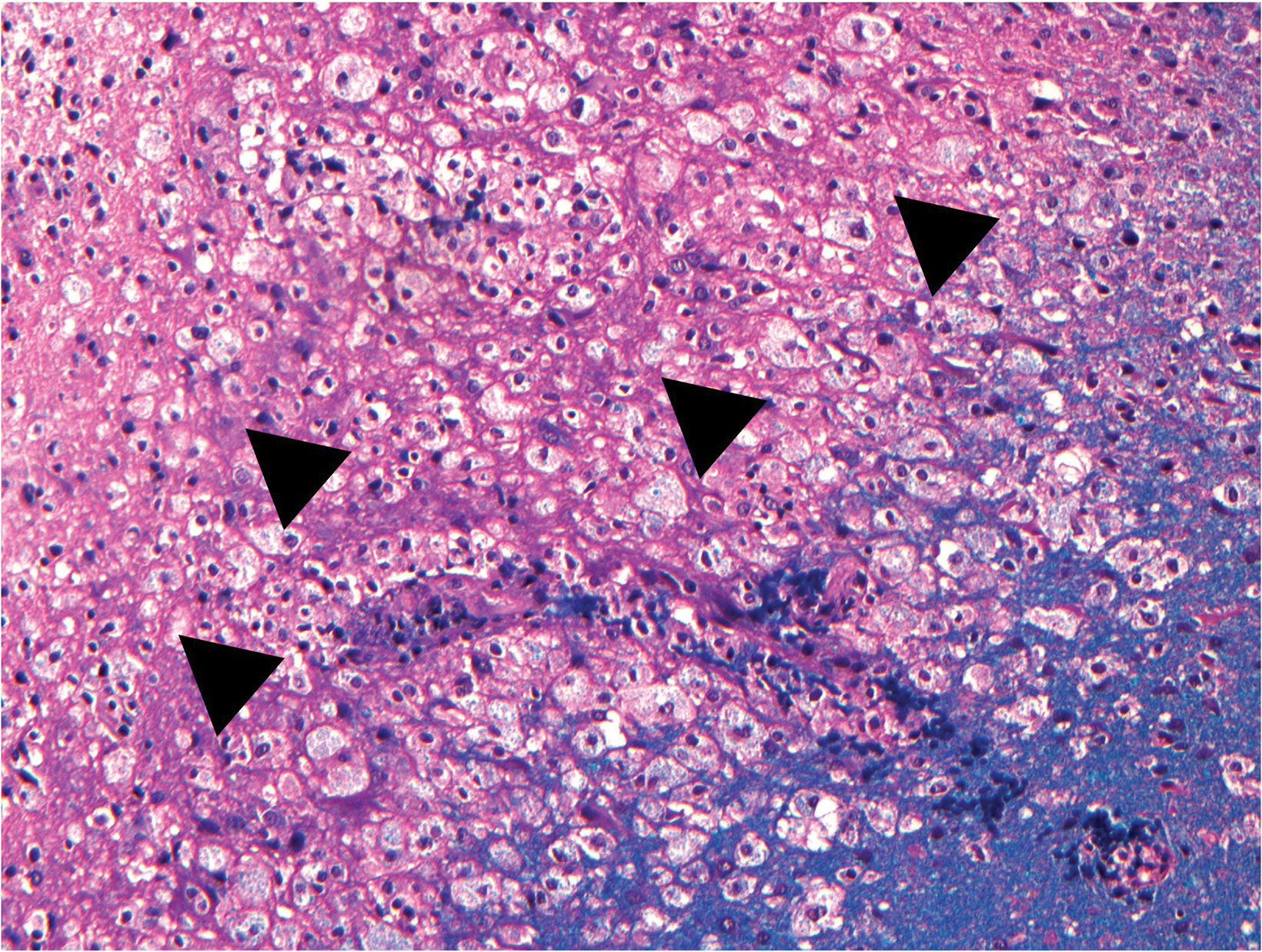
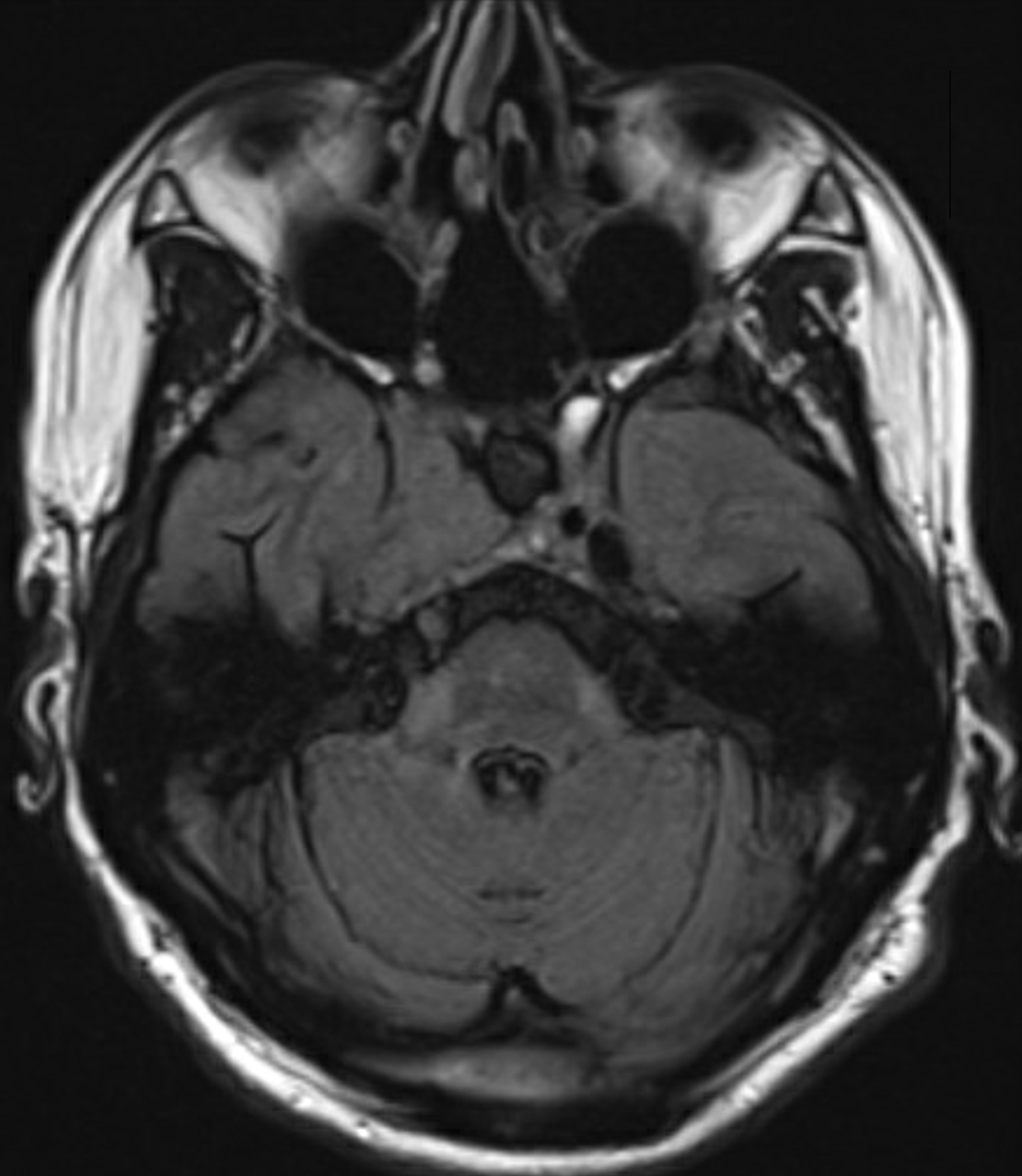
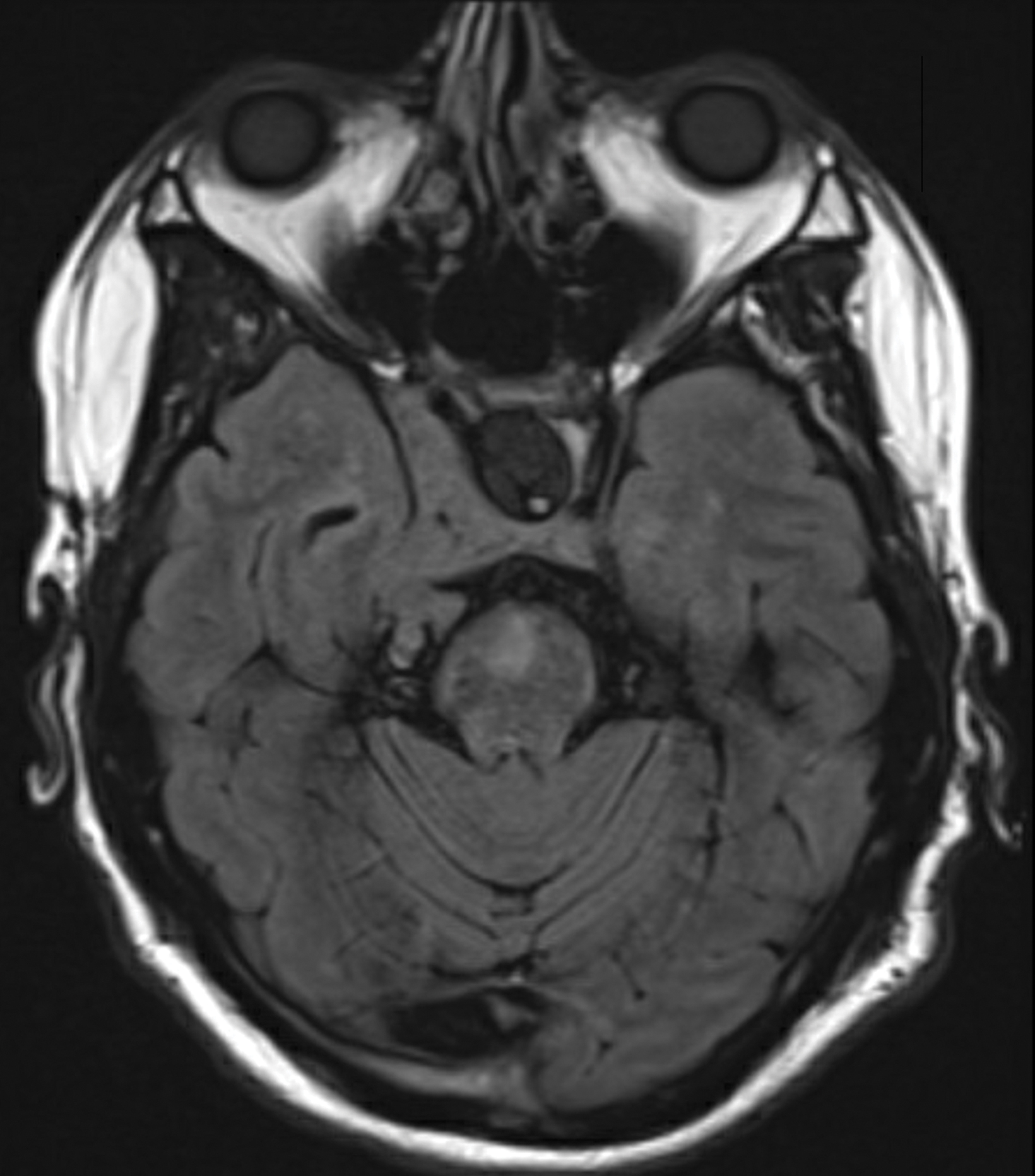
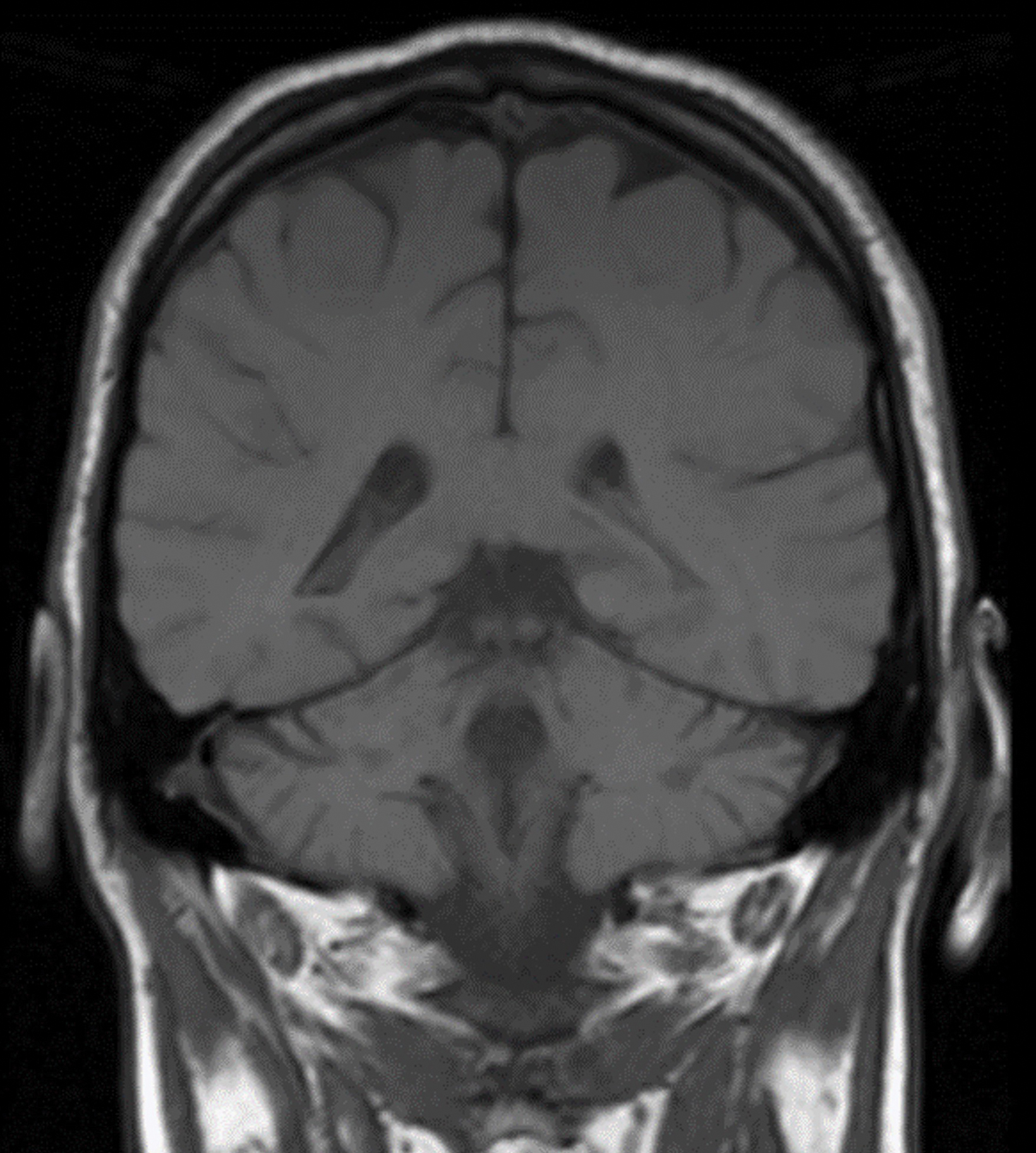
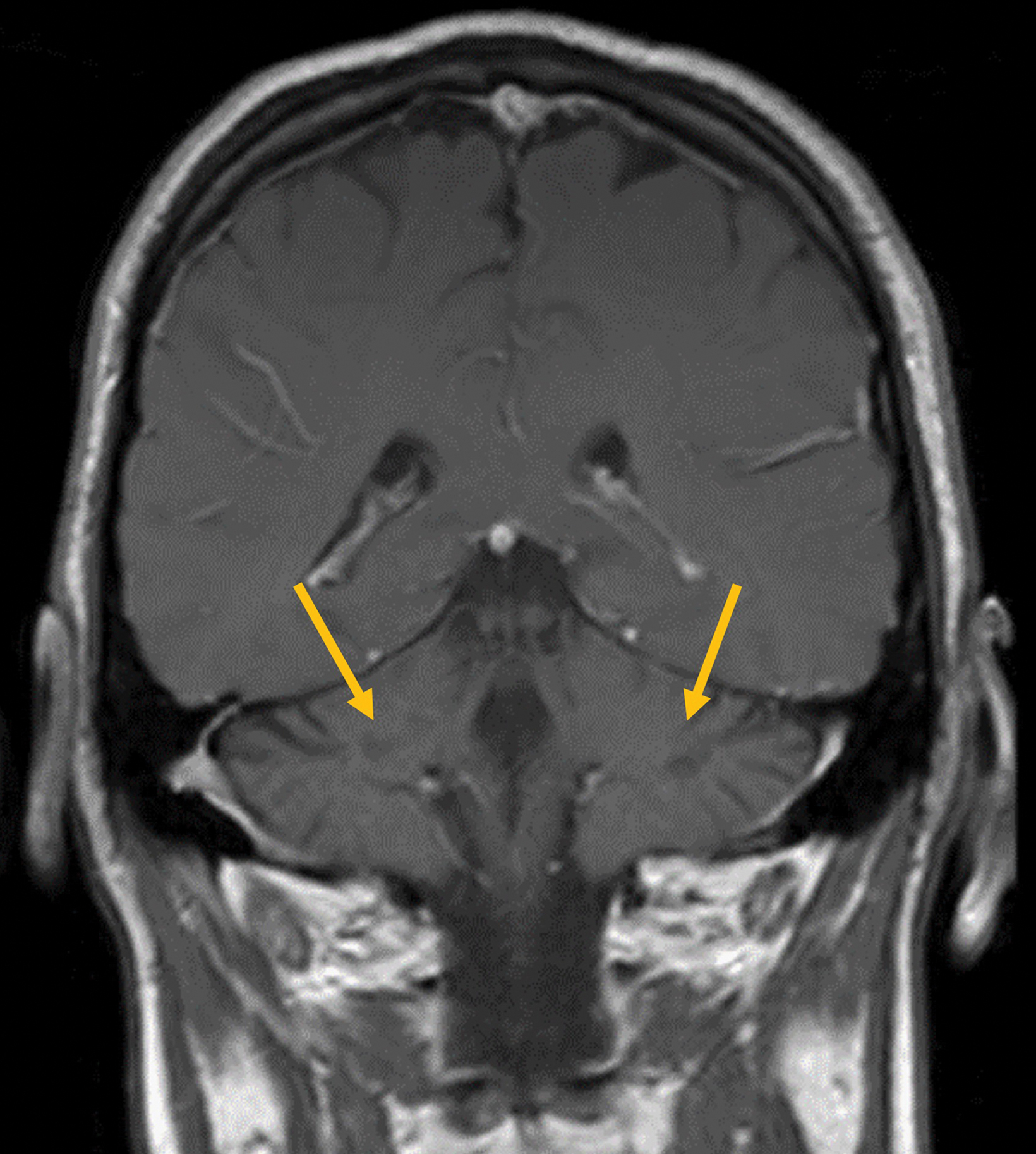
Preoperative (Figure 1A) and postoperative (Figure 1B) MRI brain scans demonstrate debulking of tumor from surgery, yet with residual disease. Radiation treatment was pursued following surgery (Figures 1C and 1D). Three months after completion of radiation treatment, and in the setting of new neurological deficits, a brain MRI scan showed multiple new cerebellar and brainstem contrast-enhancing and T2/FLAIR-hyperintense lesions (Figure 2A-D). Brain biopsy revealed perivascular parenchymal macrophage and lymphocyte infiltration, with decreased myelin staining and some preservation of neurofilament staining, but without granulomas or infectious stigmata (Figure 3A-D). Follow-up imaging, 11 months after diagnostic biopsy, showed resolved features of demyelination, with some residual changes (Figure 4A-D).
Diagnosis
Acute demyelination remote to the maximally targeted therapeutic field of radiation.
Follow-up
Following diagnostic biopsy, a 3-month follow-up brain MRI scan showed interval increase in the T2/FLAIR-hyperintense pontine lesions, but improvement in the known cerebellar ones. Clinical examination improved with noted residual left arm dysmetria and mild left hemiparesis. The next quarterly follow-up brain MRI scan showed a decrease in size of the known lesions without any contrast enhancement. The examination was stable and dexamethasone was being tapered. Subsequent follow-up, 11 months after the diagnosis, demonstrated stable imaging and examination. Multiple endocrinopathies associated with the primary tumor and subsequent treatments have also been addressed and tracked with clinical and laboratory assessments. Euthyroid state has been achieved with levothyroxine, and testosterone injections are administered periodically. Somatostatin has been continued since the diagnosis. Insulin-like growth factor 1 (IGF-1) levels have decreased, dropping from initial value >1200 ng/mL to 525 ng/mL by the time of the most recent follow-up (84-270 ng/mL as normal range).
Discussion
Acute demyelination remote to the maximally targeted field remains a rare or under-recognized entity. The initial case was described in the setting of proton radiation therapy for optic nerve meningioma.1 In a larger pediatric case series with the same treatment modality, several patients with asymptomatic white matter changes outside of the targeted area are mentioned, but additional diagnostics were not pursued.2 A case of a decade- long, relapsing demyelinating process following whole-brain radiation showed findings suggestive of a demyelinating process on repeated biopsy, but also concurrent coagulation necrosis with the initial one.3 A report of 2 patients with acute demyelination following radiation therapy for glioma was published, although unlike our patient, oligoclonal bands were seen in the cerebrospinal fluid (CSF) to establish this diagnosis.4 Although the process was initially thought to be radiation necrosis in the currently presented case, it was clinically inconsistent with such a diagnosis given the short time frame and since much of the noted enhancement and edema were outside of the high-dose radiation field, though within the region receiving 2000 cGy. Biopsy confirmed demyelination rather than necrosis. All other reported cases with similar clinical-radiological features had negative diagnostics for primary demyelinating processes and responded well to steroids, with improvement on imaging and clinical examination.1,3 Pathophysiology may involve direct radiation-related toxic effects on myelin, damage to blood-brain barrier and secondary inflammatory reaction, damage to small vasculature, or a multifactorial process triggering an autoimmune reaction.5 Oligodendrocyte depletion is also speculated.6 The pathophysiological role of elevated IGF-1 as an immunostimulant in certain autoimmune diseases is being investigated,7 but current studies also point to its protective role in experimental autoimmune demyelination, possibly by enhancing the function of Treg lymphocyte subpopulations.8 In this currently reported case, IGF-1 has remained elevated throughout the course, but with a considerable downtrend following surgery, radiation, and medical management with somatostatin.
Conclusion
Delayed acute onset demyelination in the setting of brain radiation therapy, though remote to the maximally targeted area, should be considered as a differential diagnosis in an appropriate clinical scenario. A broad diagnostic workup would be warranted in such a case, with consideration of a biopsy as an ultimate clinical-pathological investigation. Immunosuppression with steroids appears to be an effective treatment, which is consistent with the findings from other series.
References
- Redjal N, Agarwalla PK, Dietrich J, et al. Remote acute demyelination after focal proton radiation therapy for optic nerve meningioma. J Clin Neurosci. 2015;22(8):1367-1369.
- Bhattacharya D, Chhabda S, Lakshmanan R, et al. Spectrum of neuroimaging findings post-proton beam therapy in a large pediatric cohort. Childs Nerv Syst. 2020;37(2):435-446.
- Elkurd M, Hu N, Stevens J, Tornatore C. ACTRIMS 2019 - Posters - Poster 94. Mult Scler J. 2019;25(1_suppl):20-156.
- Milic M, Rees JH. Acute demyelination following radiotherapy for glioma: a cautionary tale. Pract Neurol. 2017;17(1):35-38.
- Katsura M, Sato J, Akahane M et al. Recognizing radiation-induced changes in the central nervous system: where to look and what to look for. RadioGraphics. 2021:41(1):224-248.
- Helson L. Radiation-induced demyelination and remyelination in the central nervous system: a literature review. Anticancer Res. 2018;38(9):4999-5002.
- Smith TJ. Insulin-like growth factor-I regulation of immune function: a potential therapeutic target in autoimmune diseases? Pharmacol Rev. 2010;62(2):199-236.
- Bilbao D, Luciani L, Johannesson B, Piszczek A, Rosenthal N. Insulin-like growth factor-1 stimulates regulatory T cells and suppresses autoimmune disease. EMBO Mol Med. 2014;6(11):1423-1435.
Citation
K T, VR K, ST C. Delayed Radiation-Therapy-Induced Cerebral Demyelination. Appl Radiat Oncol. 2021;(4):34-38.
December 28, 2021