Comprehensive care for the child or adolescent diagnosed with a childhood malignancy requiring palliative radiation therapy
Images



SA-CME credits are available for this article here.
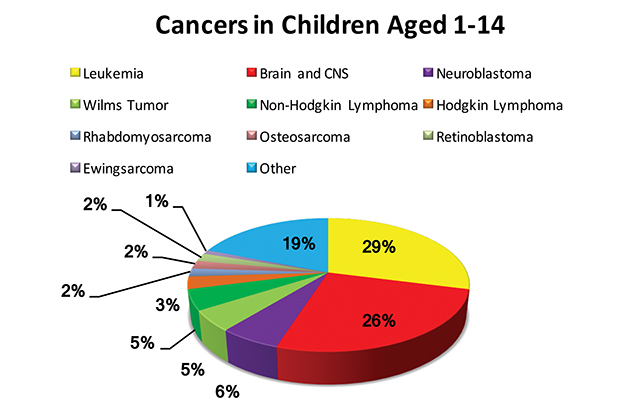
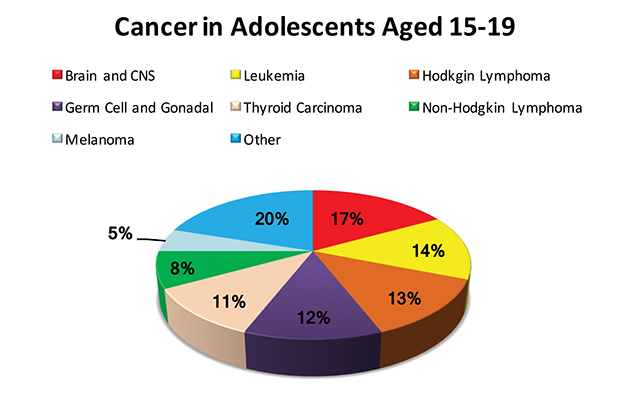
In the United States, an estimated 10 270 children ages birth to 14 years will be diagnosed with cancer in 2017, and 1190 children will die of cancer, the second leading cause of death for children following accidents.1 Five-year survival has improved for all childhood cancers from 63% in the mid-1970s to 83% today.2 The incidences of major childhood malignancies are shown in Figure 1A-B. Of these children, approximately 30% to 50%3,4 will require radiation therapy (RT) sometime during their disease course. And of children receiving RT, approximately 11% to 18%5-8 will require palliative radiation therapy (RT) to prevent or alleviate symptoms in the setting of incurable disease to optimize their quality of life (QOL).
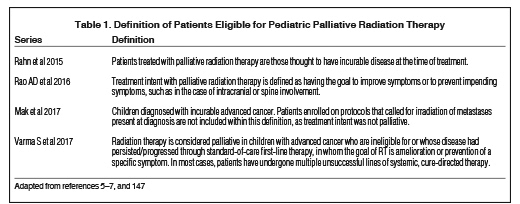
In contrast to adults diagnosed with a malignancy, the need for palliative RT is exceptionally low; most likely underestimated. Reporting differs among institutions, highlighting the variability in the definition of “palliative intent,” especially within the pediatric population (Table 1). Radiation therapy has been initiated in the setting of “preventive palliation,” where progression of uncontrolled disease could negatively impact QOL. For instance, children diagnosed with diffuse infiltrating pontine glioma (DIPG) are treated to definitive doses with the goal of achieving symptomatic relief and optimizing disease control, with cure unlikely.
Adult randomized controlled trials have demonstrated the efficacy of palliative RT in the setting of progressive primary or metastatic disease.9-11 Because of challenges in obtaining abundant quality-controlled data, there is no consensus in the standard of care for palliative RT for pediatric and adolescent patient malignancies. Current pediatric practice is extrapolated from adult palliative literature, but controversy persists about whether current adult regimens are appropriate.
Palliative Radiation Therapy: Differences Between Pediatric and Adult Patients
Pediatric malignancies have distinctive presenting symptoms, and diverse prognostic implications, treatment options, and subsequent responses. Compared with adults, children and adolescents are more likely to present with oncologic emergencies such as spinal cord compression (SCC) and superior vena cava syndrome (SVCS) earlier in the disease process at the time of diagnosis.12,13 For example, in a child, SCC or a mediastinal mass is frequently a sign of a new primary malignancy. It has been documented that sarcomas account for approximately 43% to 65% of SCC cases in children.13,14 Adults develop SCC more commonly as metastatic lesions from primary lung, prostate, and breast cancer.15,16 In the setting of SCC and paraplegia, children tend to have a more “forgiving” central nervous system (CNS) and are more likely to recover and regain ambulation with initiation of treatment compared with adults.17-21
Palliative RT is often not the first-line therapy in children and adolescents at the time of diagnosis, especially in those presenting with symptomatic spinal or mediastinal disease, as these tumors tend to be more chemo-sensitive compared to adult malignancies. Unlike with adults, the utilization of RT is focused more on relieving life-threatening problems, rather than palliation of unwanted symptoms.
Comprehensive Management for Children Diagnosed with Advanced Malignancies
Children with high-risk cancer and their families endure significant physical symptoms, psychosocial issues, and spiritual challenges, which impact QOL detrimentally.22-25 Because the “hope for cure” often remains a priority, children may undergo aggressive cancer-directed therapy, overlooking the comforts and supports necessary throughout a child’s illness.26 comprehensive pediatric oncology teams collaborate with the child/family to execute high-quality care and support from initial diagnosis, throughout palliation of symptoms, and beyond the child’s death.
A personalized and often creative approach is required to optimize care in managing these patients, incorporating the interdisciplinary team so patient/family needs and goals of care are appropriately met.27-29 Pediatric palliative care (PPC) is a specialty that has gained accolades by providing an evolving backbone of support for children/families with life-threatening or life-limiting illness. It embodies total care through management of pain, complex symptoms, psychosocial and spiritual needs, coordination of care, medical decisions, and interaction with an interdisciplinary team.26,30-34 These specialists work closely with the patient/family to enhance function, and improve QOL.30,35,37 The World Health Organization (WHO) promotes pediatric palliative care (PPC) as an approach dedicated to “active total care of the child’s body, mind, and spirit, and support for the family” (Table 2).
Clinical Indications for Pediatric Palliative Radiation Therapy
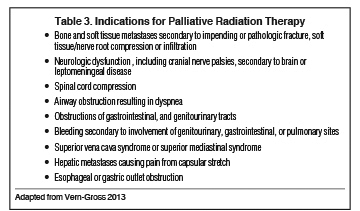
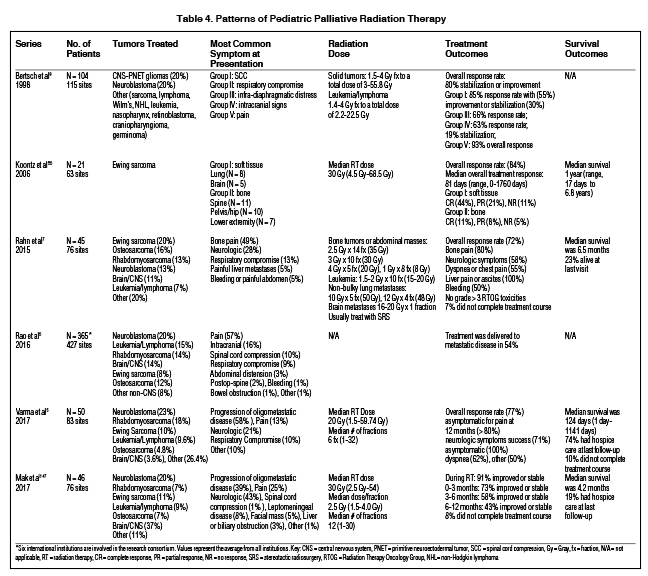
Palliative RT is more valuable in the setting of recurrence or metastatic disease progression, after multiple unsuccessful systemic therapies, than at initial diagnosis. The indications for palliative RT are similar for both pediatric and adult patients, depending on location, involvement of surrounding structures, overall prognosis, and ultimately patient/family goals of care (Table 3). Because treatment is guided to minimize acute and late toxicities, systemic therapy continues to be the optimal first-line therapy, especially in children with chemo-sensitive spinal cord tumors (eg, neuroblastoma, Ewing sarcoma, and lymphoma) in the absence of neurologic deficits.38-43 When palliative RT is initiated, treatment focuses on reducing acute toxicities (eg, radiation dermatitis, esophagitis) and anesthesia requirements by decreasing RT dose and treatment days. Despite attempts to accurately prognosticate, children may outlive initial survival predictions, underscoring the importance of always considering the implications of long-term toxicities.44 Although most radiotherapeutic techniques are extrapolated from the adult literature, several pediatric series have reported effective outcomes of palliative RT for various pediatric indications (Table 4).
Importance of biopsy prior to emergency treatment
On a new patient presentation, it is critical to obtain a tissue diagnosis to identify the primary disease and to rule out a benign or malignant process, which may require a specific treatment course. Patients may not require palliative RT, but rather a multidisciplinary approach that guides definitive treatment. If a tissue diagnosis cannot be established secondary to anesthesia risk, absence of marrow involvement, or lack of peripheral lymphadenopathy, systemic chemotherapy should be considered as initial therapy to stabilize the mediastinal mass and prevent further respiratory compromise.45 While initiation of chemotherapy often is concordant with the primary malignancy, administering radiation prior to obtaining a biopsy may compromise accurate identification of the primary disease.45,46
Superior Vena Cava Syndrome and Superior Mediastinal Syndrome
Children and adolescents diagnosed with mediastinal tumors are at risk for developing SVCS and superior mediastinal syndrome (SMS) (12%), as a result of major vessel or airway compromise.46-49 Acute lymphoblastic leukemia and non-Hodgkin lymphoma (NHL) are the most common causes of SVCS in children, whereas lung cancer is the chief cause in adults.50 With a primary diagnosis of leukemia or lymphoma, which are curable and sensitive to chemotherapy, palliative RT for SVCS or SMS is often not the first line of treatment. Palliative RT is indicated for dyspnea secondary to a malignant process in the chest or mediastinum resulting in SVCS or SMS, usually in the setting of known recurrent or relapsed disease that is otherwise resistant to systemic chemotherapy.12 RT is delivered in either standard fractionation or hypofractionation using a 3-dimensional conformal radiation therapy (3DCRT) technique. Because treatments are often based on adult literature, maintaining perspective and acknowledging the differences between child and adult is essential, especially when attempting to achieve disease control. Minimizing treatment times, reducing fractions, and using anesthesia are important considerations to decrease treatment-related toxicity.
Bone and Soft-tissue Metastases
Bone and soft-tissue metastases are one of the more common indications for palliative RT in pediatrics to reduce discomfort secondary to infiltrative lesions, tumor obstruction, and surrounding structures stretch.51,52 Most pediatric radiation oncologists extrapolate from adult landmark studies such as the Dutch Bone Metastasis Study, the Bone Pain Trial Working Party Study, and most recently the American Society for Radiation Oncology (ASTRO) guidelines.9,53-55 Although the benefits of palliative RT have been observed, a standardized fractionation scheme has not been established because of the variable tumor histologies and treatment responses.5,44,55-58 One study reported characteristics of unsuccessfully completed palliative RT courses on clinical outcomes and patterns of care in children diagnosed with advanced cancer.5 There was no difference in success rates of RT courses prescribed in ≤ 10 fractions (84%) compared with >10 fractions (94%), P = 0.43; the most unsuccessful median total dose delivered was 800 cGy. For children who are earlier in their disease trajectory, a short course of palliative RT can provide symptomatic relief without significant burden on the child or family. In the setting of widely disseminated or rapidly progressive disease, where life expectancy is unpredictable, the potential benefit of palliative RT may be quickly lost. Single fraction treatments of 800 cGy x 1 fraction to address an intractable focal symptom should still be considered in select situations. When anesthesia is required to deliver therapy, single-fraction courses are especially favorable to optimize comfort and to ensure appropriate immobilization during treatment. In terms of radiation treatment, fractionation schemes of 1-5 fractions are preferred to optimize QOL, especially in the setting of anesthesia requirements. Dose responses of ≥ 15 Gy and ≥ 20 Gy have been more effective in treating soft-tissue and bone metastases, respectively.44,58
Traditionally, bone and soft-tissue metastases have been treated using 3D conformal RT. More advanced technologies have been incorporated into the management of metastatic lesions, including intensity-modulated radiation therapy (IMRT), stereotactic body radiation therapy (SBRT), stereotactic radiosurgery (SRS), radioisotopes, and radiofrequency ablation (RFA).59-63 SBRT has been used for metastatic tumors in the palliative, curative settings and re-irradiation settings. A median dose of 40 Gy in 5 fractions (range: 16 to 50 Gy in 1 to 10 fractions) provided successful outcomes for disease control and relief of painful metastatic and recurrent osteosarcoma lesions.61
University of San Diego demonstrated lower response rates in the treatment of bone metastases based on histology.7 Median dose for bone metastases treatment was 3 Gy with a median fraction of 10. Osteosarcoma had a lower response rate compared to other histologies (58% vs 87%, respectively; P = .048). As a result, larger palliative doses have been incorporated into practice of 6 Gy for 6 fractions.56
The most recent metastatic pediatric Ewing sarcoma protocol is finally evaluating SBRT for the definitive management of metastatic bone lesions.64 Treatment doses range from 3000 to 4000 cGy in 5 fractions at 600 to 800 cGy per daily fraction. Selection of these various modalities will depend on patient prognosis, physician preference, availability, tumor location, prior treatments and response.
Spinal Cord Compression
Also rare are children diagnosed with malignancies who are at risk of developing symptomatic SCC, presenting toward the end of life (EOL) or at initial diagnosis.65,66 Ewing sarcoma, primitive neuroectodermal tumors (PNET), soft-tissue sarcoma, and neuroblastoma are some of the most common causes of SCC in children and adolescents.67 Presenting signs and symptoms include, but are not limited to, back and radicular pain, motor and sensory deficits, sphincter dysfunction, and gait abnormalities.
Whether in an initial or recurrent setting, surgical intervention to prevent and/or restore neurologic deficits, initiation of systemic chemotherapy, and RT should be evaluated to optimize care management.68 Even in the setting of neurologic compromise, surgery is often reserved for children and adolescents with a poor response to chemotherapy or RT.69 Series have demonstrated that children presenting with disease that compromises motor function continue to be at risk for significant neurologic impairment, despite initial intervention.43,70 Palliative RT in cases of relapsed or refractory disease has been used alone and as an adjunct to surgery to alleviate symptoms, and restore and maintain function.65-67, 71-73
Brain Metastases
The incidence of brain metastases in children and adolescence is significantly lower compared to adults, described at rates of approximately 1.5% to 2.5% in children diagnosed with solid tumors.74-78 Tumors reported with the greatest metastatic potential include neuroblastoma, soft-tissue sarcoma, osteosarcoma, Ewing sarcoma, Wilm’s tumor, germ cell tumor, retinoblastoma, and melanoma.77,79,80 Depending on age, systemic disease burden, tumor histology, and prognosis, a standard treatment course of 30 to 36 Gy in 1.5 to 2.5 Gy fractions is appropriate. In the setting of previously irradiated tissue, SRS may be reasonable to consider to relieve symptom burden, optimize tumor control, and minimize risk of tissue toxicity.77,81,82
Symptoms and Distress in Pediatric Cancer
Children and adolescents are at risk of considerable distress as a result of tumor involvement, procedures, and treatment toxicities. Several pediatric series have demonstrated that symptoms and suffering at EOL are poorly controlled.27,29,83 Self-reporting measures have described pain, fatigue, loss of appetite, psychological distress, and nausea as the most common symptoms.84, 85, 87
Symptom management at EOL is an ongoing treatment obstacle for many clinicians. Pain is one of the most commonly studied symptoms, but most challenging to manage.84-87 An EOL study indicated that parents of dying children identified that 89% of the children suffered from at least one symptom, with pain, fatigue, and dyspnea as the most common; relief was only achieved in 27%.29 Another study reported that 94% suffered from ≥ 3 symptoms, whereas 76% had ≥ 5 or more symptoms at EOL.88 The most frequent complaint included pain (100%), nausea/vomiting (63%), constipation (57%), and anxiety (56%).88 Incorporating age-appropriate communication, assessment tools, integrative therapies, and modifying factors into child or adolescent care can help alleviate the level of discomfort and improve responses to pain.23,89-92
To accurately assess pain level, intensity, and treatment response, age-appropriate assessment tools and baseline parental assessments are valuable when caring for these patients. Unlike older children and adolescents who may express emotion, pain, and treatment-related discomfort, younger counterparts may demonstrate pain through withdrawal and decreased activity.89
An assessment of distress, which can be complex, may require a comprehensive evaluation. Several scales assess symptoms: PQ-Memorial Symptom Assessment Scale (PQ-MSAS),23,84,85 and Pediatric Quality of Life Inventory 4.0 Generic Core Scales (PedsQL 4.0).92
Early Integration of Comprehensive Pediatric Palliative Care Team
To provide a supportive network for the evolving needs of the patient/family, early initiation of palliative care is recommended at diagnosis for children and adolescents with advanced malignancies. PPC focuses on the integration of expectations of life extension and disease-directed therapy, while honoring goals of comfort and QOL. Early integration of palliative care, advanced end-of-life conversations, and systematic symptom management have demonstrated improved outcomes and enhanced QOL.30, 37
The American Academy of Pediatrics (AAP) has provided guidelines recommending early consultation of PPC to ensure that distressing symptoms are prevented and treated, and complicated decisions at initial diagnosis are facilitated when the goals of care focus on cure.34,93 Many patients receiving palliative RT are seeking disease-directed therapy or are enrolled in experimental therapy. A recent study from St. Jude reported that 79.4% of patients who received palliative care underwent experimental therapy, with 40.5% enrolled on a phase I trial.25 One-third of the patients (35.5%) received cancer-directed therapy during their last month of life. Delayed palliative care (PC) (< 30 days before death) led to higher odds of death in the intensive care unit compared to a home/hospice setting for patients who received earlier PC intervention (P < .0001).
In addition to initiation of earlier PPC involvement, one study described the clinical outcomes of 50 children who completed 83 courses of RT and their relationship with the palliative and hospice services.9 Of all treatment, 15 palliative RT courses were delivered to patients within the last 30 days of life, 7 of which were completed within the last 7 days of life. Treatment delivered within the last month of life had a lower success rate at palliation compared to courses delivered prior to 30 days, 28% vs 89%, respectively (P < .0001). Location of death for 7 patients who received palliative RT within the last 7 days of life were all within a hospital setting (inpatient floor or ICU) except for 1 patient for whom medical records were not available. Of the patients who received palliative RT, 28% already had PC involvement, whereas 60% were referred to the institutional PC team during their clinical course. Patients receiving palliative RT received supportive services: PC alone, hospice alone, both PC and hospice, or neither, at 14%, 18%, 46%, and 12%, respectively.9 The median time to hospice referral was 96 days following the last palliative RT treatment (range: 0 to 924 days). With the support of the PPC, advanced care planning can assist with early delivery of home services and ensure that death takes place in the preferred location of the child/family.88,94
Communication
Effective communication facilitates appropriate patient, parent and team knowledge, trust, and a common goal.95-98 Identifying the patient/family goals of care99,100 prior to initiating palliative RT will assist communication and future medical decision-making processes, identify necessary supports, and optimize QOL (Table 5). Specific to radiation oncology, it is critical to identify the patient/family understanding of the illness, how much they would like to know, the associated risks/benefits, and treatment limitations, and respond to their emotions, physical presence during conversations, and high-quality care.96,101-103 Specific to radiation treatment planning, it is essential to address patient needs based on age, sedation requirements, and management of uncontrolled symptoms to ensure treatment accuracy and safety. Child-life therapy, social work, and interpreter services are valuable resources to facilitate information sharing and improve their experience.104
Prognostication
When faced with a life-threatening illness, most parents prefer to be well-informed about their child’s diagnosis, treatment-related complications, survival outcomes, and the potential impact on function and QOL.105-110 If the children are diagnosed with advanced malignancies, parents often prefer cancer-directed therapy (eg, surgery, chemotherapy, biologic agents, RT) rather than more palliative therapies with an emphasis on comfort measures of prolonging life and/or relief of symptoms.99,110,111 Parents’ understanding and perception of their child’s disease depends on the effectiveness of communication from the primary care team.26,114-117 Explicit or clear sources of information regarding a parent’s child, conversations with the oncologist at the time of diagnosis, or daily conversations with the oncologist and nurses, were informative approximately 73% to 85% of the time.116 Implicit, or inherent sources of information, including “how parents feel their child is doing,” or “how the oncologist appears to feel the child is doing,” were informative. Parents who valued implicit information had lower prognostic accuracy, particularly when focusing on a “general sense of how my child’s oncologist seems to feel my child is doing.”118 Parental preference, developmental stage variabilities, the family provider, and patient should be included in conversations about their disease and decision-making.26,117,118 Children and adolescents are aware of their disease and prognosis as early as age 3 years; it is critical for clinicians to encourage open and honest conversations.118,119
Advanced Care Planning and EOL
Early introduction of PPC by the team facilitates discussions around advanced care planning EOL hospice conversations and enrollment, improved symptom control, introduction of do-not-resuscitate orders, and preparations during the child’s last month of life.88,120
It is important to appreciate the perspective of the child, siblings, and parents regarding the emotional experience and medical-decision making, and address supports following the child’s death to reduce complicated bereavement risk.121-124 Children harbor a strong intuition and sensitivity to the experience of loneliness, anxiety, and imminent death.28 Despite their young age, children ages 10 to 20 years who are diagnosed with advanced malignancies are competent to participate in medical-decision making, engage in EOL discussions, and understand the consequences and impact of their decisions on how their death may influence loved ones.125
Bereavement
The death of a child can be shattering and transformative, influencing the psychosocial and physical health of family and caregivers involved.126-129 Bereaved parents are at long-term risk of developing physical and psychosocial co-morbidities.130-137 Mortality rates have been reported the highest among bereaved parents within the first 3 years following a child’s death; however, some studies report no difference in morbidity or mortality rates between bereaved and nonbereaved parents.138,139 Studies have confirmed increased chronic illnesses during the first 6 months following a child’s death.129,140 To assist with emotional and psychological adjustment prior to the child’s death and to assure appropriate support throughout the deteriorating disease state, bereavement support should be initiated well before the dying phase.27,141,142 As a radiation oncologist, acknowledgement of the evolving palliative and bereavement supports needed for the patient, siblings, and family is essential.142
Barriers to Pediatric Palliative Care
The low incidence of pediatric malignancies and death, differences in pediatric developmental stages, insufficient exposure of current medical school and residency programs to palliative education and competencies, lack of insurance provider reimbursement, and the limitations of prospective data on the incidence and management of symptoms are some of the major barriers to delivering high-quality comprehensive PC in children with advanced malignancies.143 Despite attempts to provide effective comprehensive EOL care, various barriers remain, including unrealistic expectations from the family (47.5%), prognostic denial from the family (35.7%), familial conflict (30.3%), the patient’s unrealistic expectations (10.1%), and prognostic denial from the patient (7.6%).144 The growth and execution of dedicated PC may be curtailed due to the child/family requirements for additional emotional and psychosocial support; limited resources, scarcity of trained staff, and institutional budget constraints.145 Clinical triggers for PC consultations may help facilitate earlier involvement.31
Barriers to Palliative Radiation Therapy
Several barriers have been identified resulting in the underutilization of pediatric palliative RT, predominately secondary to misconceptions or concerns for treatment-related toxicities. In a Canadian survey, formally trained palliative medicine physicians were more likely to refer children for palliative RT compared to responders without a palliative background (94 % vs 73 %, p < .01).146 Numerous barriers include, but are not limited to, patient/family reluctance, potential benefit ignorance, potential treatment-related side effect misconceptions, short life expectancy, cancer center proximity, transportation limitations, concern for lack of improvement, and impact on QOL.146
A collaborative multi-institutional survey reported on the practice patterns of palliative RT in 365 pediatric patients in an international pediatric research consortium.6 Treatment toxicity (83%) was the most common physician-reported barrier to initiation of RT, and treatment resources, insurance authorization/cost, anesthesia availability, and parental concerns were less of a deterrent.6 A recent publication noted that the 2 most common indications for palliative RT were oligometastatic disease in asymptomatic patients (39%) and pain (25%).147 A similar study reported only low-grade self-limiting acute toxicity outcomes of 45 children treated with palliative RT: Nausea (3.6%), dermatitis (6.0%), and fatigue (3.6%); no grade 3 or late toxicities were described.7
Education and innovative oncology curriculums emphasize increasing clinical exposure and didactic lectures to improve communication skills and develop a stronger knowledge base of palliative competencies. Greater clinical education and addressing parental and provider concerns may increase the appropriate consideration and implementation of palliative RT.135,146,148,149
Future Directions
Most palliative RT treatments are delivered using 3D-CRT, varying 41% to 63%.6,7,147 Incorporating more advanced radiotherapeutic techniques including IMRT, SBRT, SRS, and proton beam therapy (PBT), can deliver highly conformal treatment to achieve the desired tumor response dose and spare normal tissue, while achieving symptomatic relief.60,61,64 Current controversy centers on cost of these modalities if a child is not expected to live long enough to benefit from the therapy received; however, if a potential for decreased toxicity and local failure exists, a more conformal dose-escalated approach would be favorable, especially in the re-irradiation setting.147,150,151
Research
Future research direction is necessary to better define guidelines for palliative RT delivery for pediatric patients. Although there are standard guidelines for palliative RT in adults, it is well known that response rates vary depending on tumor histologies.5 Similarly, pediatric tumors vary in histology and response specifically to RT, as described in several series.6,7,9,44,152,153 Leukemia, neuroblastoma, and Ewing sarcoma are more likely to achieve a complete response with RT compared to CNS malignancies. There is a need to standardize doses by reducing the required treatment doses to maintain optimal local control and symptomatic relief, decrease treatment time and lower toxicity. A meta-analysis of the collective literature or a collaborative effort for a multi-institutional prospective study is warranted to evaluate optimal dose and fractionation schema specific to disease sites, symptomatic response, treatment-related toxicities, survival outcomes, and QOL measures to summarize the evidence and identify a consensus of comprehensive care and treatment guidelines.
Conclusion
Prospective research is necessary to establish palliative RT guidelines for management of pediatric malignancies to honor preferences and maintain best practices. With more technologic advances, multidisciplinary team plan of care and communication will become extremely important in providing the correct medical, emotional and psychosocial decisions and supports for the patient and family unit.
References
- American Cancer Society. Cancer Facts & Figures 2017. http://www.cancer.org/content/dam/cancer-org/research/cancer-facts-and-statistics/annual-cancer-facts-and-figures/2017/cancer-facts-and-figures-2017.pdf. Accessed January 23, 2017.
- Howlander N, Noone AM, Krapcho, M, et al, eds. SEER Cancer Statistics Review, 1975-2013, National Cancer Institute, Bethesda, Maryland. http://seer.cancer.gov/csr/1975_2013. Based on November 2015 SEER data submission, posted to the SEER web site. April 2016.
- Glimelius B, Ask A, Bjelkengren G, et al. Number of patients potentially eligible for proton therapy. Acta Oncologica. 2005;44(8):836-849.
- Rosenschold M, Engelholm SA, Brodin PN, et al. A retrospective evaluation of the benefit of referring pediatric cancer patients to an external proton therapy center. Pediatr Blood Cancer. 2015;63(2):262-269.
- Varma S, Friedman DL, Stavas MJ. The role of radiation therapy in palliative care of children with advanced cancer: clinical outcomes and patterns of care. Pediatr Blood Cancer. 2017;64:e26359.
- Rao AD, Chen Q, Ermorian RP, et al. Practice patterns of palliative radiation therapy in pediatric oncology patients in an international pediatric research consortium. Pediatr Blood Cancer. 2017;64(11).
- Rahn DA, 3rd, Mundt AJ, Murphy JD. Clinical outcomes of palliative radiation therapy for children. Pract Radiat Oncol. 2015;5(3):183-187.
- Bertsch H, Rudoler S, Needle M, et al. Emergent/urgent therapeutic irradiation in pediatric oncology: patterns of presentation, treatment, and outcome. Med Pediatr Oncol. 1998;30:101-105.
- Lutz S, Balboni T, Jones J, et al. Palliative radiation therapy for bone metastases: update of an ASTRO evidence-based guideline. Pract Radiat Oncol. 2017;7:4-12.
- Scoccianti S, Ricardi U. Treatment of brain metastases: review of phase III randomized controlled trials. Radiother Oncol. 2012;102:168-179.
- Sundstrom S, Bremnes R, Aasebo U, et al. Hypofractionated palliative radiotherapy (17 Gy per two fractions) in advanced non-small-cell lung
- carcinoma is comparable to standard fractionation for symptom control and survival: A national phase III Trial. J Clin Oncol. 2004 22(5):801-810.
- Ingram L, Rivera GK, Shapiro DN. Superior vena cava syndrome associated with childhood malignancy: analysis of 24 cases. Med Pediatr Oncol. 1990;18(6):476-481.
- Raffel C, Neave VC, Lavine S, McComb. Treatment of spinal cord compression by epidural malignancy in childhood. Neurosurgery. 1991;28(3):349-352.
- Ch’ien LT, Kalwinsky DK, Peterson G, et al. Metastatic epidural tumors in children. Med Pediatr Oncol. 1982;10(5):455-462.
- Pizzo PA, Horowitz ME, Poplack PG, et al. Solid tumors of childhood. In: DeVita VT, Hellmann S, Rosenberg SA eds: Cancer: Principles & Practice of Oncology, 4th ed. Philadelphia, PA: JB Lippincott, 1993:1738-1791.
- Bruckman JE, Bloomer WD. Management of spinal cord compression. Semin Oncol. 1978;5:135-140.
- Gilbert RW, Kim JH, Posner JB. Epidural spinal cord compression from metastatic tumor: diagnosis and treatment. Ann Neurol. 1978 3(1):40-51.
- Rodriguez M, Dianpoli RP. Spinal cord compression: with special reference to metastatic epidural tumors. Mayo Clin Proc. 1980;55(7):442-448.
- Klein SL, Sanford RA, Muhlbauer MS. Pediatric spinal epidural metastases. 1991; J Neurosurg. 74(1):70-75.
- Lange B, D’Angio G, Ross AJ III, et al. Oncologic emergencies. In: Pizzo PA, Poplack DG, eds. Principles and Practice of Pediatric Oncology, 2nd ed. Philadelphia, PA: J.B. Lippincott Co. 1993:951-972.
- Lewis DW, Packer RJ, Raney B, et al. Incidence, presentation, and outcome of spinal cord disease in children with systemic cancer. Pediatrics. 1986;78(3):438-443.
- Wolfe J, Klar N, Grier HE, et al. Understanding of prognosis among parents of children who died of cancer: impact on treatment goals and integration of palliative care. JAMA. 2000;284(19):2469-2475.
- Wolfe J, Orellana L, Ullrich C, et al. Symptoms and distress in children with advanced cancer: prospective patient-reported outcomes from the PediQUEST Study. J Clin Oncol. 2015;33(17):1928-1935.
- Ullrich CK, Dussel V, Hilden JM, et al. End-of-Life experience of children undergoing stem cell transplantation for malignancy: parent and provider perspectives and patterns of care. Blood. 2010;115(19):3879-3885.
- Kaye EC, Gushue CA, DeMarsh S, et al. Illness and end-of-life experiences of children with cancer who receive palliative care. Pediatr Blood Cancer. 2018;65(4). E26895. DOI: 10.1002/pbc.26895.
- Himelstein BP, Hilden JM, Boldt AM, Weissman D. Pediatric palliative care. N Engl J Med. 2004;350(17):1752-1762.
- Contro N, Larson J, Scofield S, et al. Family perspectives on the quality of pediatric palliative care. Arch Pediatr Adolesc Med. 2002;156(1):14-19.
- Hechler T, Blankenburg M, Friedrichsdorf SJ et al. Parents’ perspective on symptoms, quality of life, characteristics of death and end-of-life decisions for children dying from cancer. Klin Padiatr. 2008;220(3):166-174.
- Wolfe J, Grier HE, Klar N, et al. Symptoms and suffering at the end of life in children with cancer. New Engl J Med. 2000;342(5):326-333.
- Liben S, Papadadou D, Wolfe J. Paediatric palliative care: challenges and emerging ideas. Lancet. 2008;371(9615):852-864.
- Weaver MS, Rosenberg AR, Tager J, et al. A summary of pediatric palliative care team structure and services as reported by centers caring for children with cancer. J Palliat Med. 2017. DOI: 10.1089/jpm.2017.0405
- Hain R, Heckford E, McCulloch R. Paediatric palliative medicine in the UK: past, present, future. Arch Dis Child. 2012;97(4):381-384.
- Kang T, Hoehn KS, Licht DJ, et al. Pediatric palliative, end-of-life, and bereavement care. Pediatr Clin N Am. 2005;52(4):1029-1045.
- Section on Hospice and Palliative Medicine and Committee on Hospital Care. Pediatric Palliative Care and Hospice Care Commitments, Guidelines, and Recommendations. Pediatrics. 2013;966-972.
- Friebert S, Williams C. NHPCO’s Facts and Figures. Pediatric Palliative & Hospice Care in America. National Hospice and Palliative Care Organization: 2015 Edition. 1-12. https://www.nhpco.org/sites/default/files/public/quality/Pediatric_Facts-Figures.pdf. Accessed May 10, 2018.
- World Health Organization. Definition of Palliative Care. World Health Organization Web Site. http://www.who.int/cancer/palliative/definition/en. Accessed November 22, 2017.
- Waldeman E, Wolfe J. Palliative care for children with cancer. J Nat Rev Clin Oncol. 2013;10: 100-107.
- Holgersen LO, Santulli TV, Schullinger JN, Berdon WE. Neuroblastoma with intraspinal (dumbbell) extension. J Pediatr Surg. 1983;18(4):406-411.
- Kozlowski K, Beluffi G, Masel J, et al. Primary vertebral tumours in children: report of 20 cases with brief literature review. Pediatr Radiol. 1984;14(13):129-139.
- Lyding JM, Tseng A, Newman A, Collins S, Shea W. Intramedullary spinal cord metastases in Hodgkin’s disease: rapid diagnosis and treatment resulting in neurologic recovery. Cancer. 1987;60(8):1741-1744.
- Obviatt DL, Kirshner HS, Stein RS. Successful chemotherapeutic treatment of epidural compression in non-Hodgkin’s lymphoma. Cancer. 1982;49(12):2446-2448.
- Ortega JA, Wharam M, Gehan EA, et al. Clinical features and results of therapy for children with paraspinal soft tissue sarcoma. J Clin Oncol. 1991;9(5):796-801.
- Hayes FA, Thompson EI, Hvizdala E, et al. Chemotherapy as an alternative to laminectomy and radiation in the management of epidural tumor. J Pediatr. 1984;104(2):221-224.
- Paulino AC. Palliative radiotherapy in children with neuroblastoma. Pediatr Hematol Oncol. 2003;20(2):111-117.
- Kumari A, Gupta S, Singhal PP. Superior vena cava syndrome in children: a case report. Middle East J Anesthesiol. 2006;18(5):933-938.
- Loeffler JS, Leopold KA, Recht A, et al. Emergency prebiopsy radiation for mediastinal masses: impact on subsequent pathologic diagnosis and outcome. J Clin Oncol. 1986;4(5):716-721.
- King RM, Telander RL, Smithson WA, et al. Primary mediastinal tumors in children. J Pediatr Surg. 1982;17(5):512-520.
- Arya LS, Narain S, Tomar S, et al. Superior vena cava syndrome. Indian J Pediatr. 2002; 69(4):293-297.
- Ferrari LR, Bedford RF. General anesthesia prior to treatment of anterior mediastinal masses in pediatric cancer patients. Anesthesiology. 1990;72(6):991-995.
- D’Angio GJ, Mitus A, Evans AE. The superior mediastinal syndrome in children with cancer. Am J Roentgenol. 1975;93:537-544.
- Foley KM. Pain syndromes in patients with cancer. Med Clin N Am. 1987;71: 169-184.
- Foley KM. Acute and Chronic cancer pain syndromes. In: Doyle D, Hanks G, Cherny N, Calman K, eds. Oxford Textbook of Palliative Medicine, 3rd ed. Oxford: Oxford University Press. 2004.
- Steenland E, Leer JW, van Houwelingen H, et al. The effect of a single fraction compared to multiple fractions on painful bone metastases: a global analysis of the Dutch Bone Metastasis Study. Radiother Oncol. 1999;52(2):101-109.
- The Bone Pain Trial Working Party. 8 Gy single fraction radiotherapy for the treatment of metastatic skeletal pain: randomized comparison with a multi-fraction schedule over 12 months of patient follow-up. Radiother Oncol. 1999;52(2):111-121.
- Hartsell WF, Scott CB, Bruner DW, et al. Randomized trial of short vs long- course radiotherapy for palliation of painful bone metastases. J Natl Cancer Inst. 2005;97(11):798-804.
- Koontz BF, Clough RW, Halperin EC. Palliative radiation therapy for metastatic Ewing sarcoma. Cancer. 2006;106(8):1790-1793.
- Deutsch M, Tersak JM. Radiotherapy for symptomatic metastases to bone in children. Am J Clin Oncol. 2004; 27(2):128-131.
- Caussa L, Hijal T, Michon J, Helfre S. Role of palliative radiotherapy in the management of metastatic pediatric neuroblastoma: a retrospective single- institution study. Intl J Radiat Oncol. 2011;79(1):214-219.
- Anderson PM, Wiseman GA, Dispenzieri A, et al. High-dose samarium-153 ethylene diamine tetramethylene phosphonate: low toxicity of skeletal irradiation in patients with osteosarcoma and bone metastases. J Clin Oncol. 2002;20(1):189-196.
- Brown LC, Lester RA, Grams MP, et al. Stereotactic body radiotherapy for metastatic and recurrent Ewing sarcoma and osteosarcoma. 2014; Sarcoma: Article ID 418270:1-9.
- Nanda R, Dhabbaan A, Janss A, et al. The feasibility of frameless stereotactic radiosurgery in the management of pediatric central nervous system tumors. J Neurooncol. 2014;117(2):329-335.
- Botsa E, Poulou LS, Koutsogiannis I, et al. CT-guided radiofrequency tumor ablation in children. Pediatr Radiol. 2014;44(11):1421-1425.
- Resche I, et al. Palliation of pain associated with metastatic bone cancer using samarium-153 lexidronam: a double-blind placebo-controlled clinical trial. J Clin Oncol. 1998;16(4):1574-1581.
- DuBois S, Bender JG, Krailo M, et al. Children’s Oncology Group AEWS1221- Randomized Phase II Evaluated the addition of IGF-1R monoclonal antibody Ganitumab (AMG 479, NSC#750008, IND#120449) to multiagent chemotherapy for patients with newly diagnosed metastatic Ewing sarcoma.
- Baten M, Vannucci RC. Intraspinal metastatic disease in childhood cancer. J Pediatr. 1977;90(2):207-212.
- Punt J, Pritchard J, Pincott JR, Till K. Neuroblastoma: a review of 21 cases presenting with spinal cord compression. Cancer. 1980;45(12):3095-3101.
- Pollono D, Tomarchia S, Drut R, et al. Spinal cord compression: a review of 70 pediatric patients. Pediatr Hematol Oncol. 2003;20(6):457-466.
- Tachdjian MO, Matson DD. Orthopaedic aspects of intraspinal tumors in infants and children. J Bone Joint Surg Am. 1965;47:223-248.
- Fabian CJ, Mansfield CM, Dahlberg S, et al. Low dose involved field radiation after chemotherapy in advanced Hodgkin’s disease: a Southwest Oncology Group randomized study. Ann Intern Med. 1994;120(11):903-912.
- Simon T, Niemann CA, Hero B, et al. Short- and long-term outcome of patients with symptoms of spinal cord compression by neuroblastoma. Dev Med Child Neurol. 2012;54(4):347-352.
- Bernardi BD, Pianca C, Pistamiglio P, et al. Neuroblastoma with symptomatic spinal cord compression at diagnosis: treatment and results with 76 cases. J Clin Oncol. 2001;19(1):183-190.
- Shyn PB, Campbell GA, Guinto FC, Crofford MJ. Primary intracranial ependymoblastoma presenting as spinal cord compression due to metastasis. Childs Nerv Syst. 1986;2(6):323-325.
- Gupta V, Srivastava A, Bhatia B. Hodgkin’s disease with spinal cord compression. J Pediatr Hematol Oncol. 2009 31(10):771-773.
- Allen JC. Brain metastases. In: Deutsch M, ed. Management of Childhood Brain Tumors. Boston, MA: Kluwer Academic Publishers. 1990;457-464.
- Deutsch M, Albo V, Wollman MR. Radiotherapy for cerebral metastases in children. Int J Radiat Oncol Biol Phys. 1982;8(8):1441-1446.
- Deutsch M, Orlando S, Wolmann M. Radiotherapy for metastases to the brain in children. Med Pediatr Oncol. 2002;39(1):60-62.
- Suki D, Khoury Abdulla R, et al. Brain metastases in patients diagnosed with a solid primary cancer during childhood experience from a single referral cancer center. J Neurosurg Pediatr. 2014;14(4):372-385.
- Ostrom QT, Gittleman H, Fulop J, et al. CBTRUS Statistical Report: Primary Brain and Central Nervous System Tumors Diagnosed in the United States in 2008-2012. Neuro Oncol. 2015;17Suppl4:iv1-iv62.
- Graus F, Walker RW, Allen JC. Brain metastases in children. J Pediatr. 1983;103(4):558-561.
- MacRae T, Grimard L, Hsu E, et al. Brain metastases in Wilms’ tumor: case report and literature review. J Pediatr Hematol Oncol. 2002;24(2): 149-153.
- King D, Connolly D, Zaki H, et al. Successful treatment of metastatic relapse of medulloblastoma in childhood with single session stereotactic radiosurgery: a report of 3 cases. J Pediatr Hematol Oncol. 2014;36(4):301-304.
- Keshavarzi S, Meltzer H, Ben-Haim S et al. Initial clinical experience with frameless optically guided stereotactic radiosurgery/radiotherapy in pediatric patients. Childs Nerv Syst. 2009; 2(7):837-844.
- Wolfe J, Friebert S, Hilden J. Caring for children with advanced cancer integrating palliative care. J Pediatr Clin N Am. 2002;49(5):1043-1062.
- Collins JJ, Byrnes ME, Dunkel IJ, et al. The measurement of symptoms in children with cancer. J Pain Sympt Manage. 2000;19(5):363-377.
- Collins JJ, Devine TD, Dick GS, et al. The measurement of symptoms in young children with cancer: the validation of the Memorial Symptom Assessment Scale in children aged 7-12. J Pain Sympt Manage. 2002;23(1):10-16.
- Hedén L, Pöder U, von Essen L, Ljungman G. Parents’ perceptions of their child’s symptom burden during and after cancer treatment. J Pain Sympt Manage. 2013;46(3) 366-375.
- Pöder U, Ljungman G, von Essen L. Parents’ perceptions of their children’s cancer-related symptoms during treatment: a prospective longitudinal study. J Pain Sympt Manage. 2010; 40(5):661-670.
- Vern-Gross TZ, Lam CG, Graff Z, et al. Patterns of end-of-life care in children with advanced solid tumor malignancies enrolled on a palliative care service. J Pain and Sympt Manage. 2015;50(3):305-312.
- Cohen LL, Lemanek K, Blount RL, et al. Evidence-based assessment of pediatric pain. J Ped Psych. 2008;33(9)939-955.
- Stinson JN, Jibb LA, Nguyen C, et al. Development and testing of a multidimensional iPhone pain assessment application for adolescents with cancer. J Med Internet Res. 2013;15(3):e51.
- Friedrichsdorf SJ. Pain management in children with advanced cancer and during end-of-life care. Pediatr Hematol Oncol. 2010;27:257-261.
- Varni JW, Burwinkle TM, Katz ER, et al. The Peds QL in pediatric cancer: reliability and validity of the Pediatric Quality of Life Inventory Generic Core Scales, Multidimensional Fatigue Scale, and Cancer Module. J Clin Oncol. 2002;33(17):1928-1935.
- American Academy of Pediatrics. Committee on Bioethics and Committee on Hospital Care. Palliative care for children. Pediatrics. 2000;106;351-357.
- Dussel V, Kericbergs U, Hilden JM, et al. Looking beyond where children die: Determinants and effects of planning a child’s location of death. J Pain Sympt Manage. 2009;37(1):33-43.
- Pantilat SZ. Communicating with seriously ill patients. Better words to say. JAMA. 2009;301(12):1279-1281.
- Garwick AW Patterson J, Bennett FC, Blum RW. Breaking the news. How families first learn about their child’s chronic condition. Arch Pediatr Adolesc Med. 2012;149(9):991-997.
- Thomas, KW. Conflict and Conflict Management. Reflections and Update. J Organizat Behav, Vol. 13, No. 3, Special Issue: Conflict and Negotiation in Organizations: Historical and Contemporary Perspectives (May, 1992), pp. 265-274.
- Thomas, KW. Conflict and Conflict Management. In: Dunnette MD, ed. Handbook of Industrial and Organizational Psychology. Chicago, IL: Rand McNally; 1976.
- Hinds PS, Oakes L, Furman W, et al. Decision making by parents and healthcare professionals when considering continued care for pediatric patients with cancer. Oncol Nurs Forum. 1997;24(9):1523-1528.
- Kane J, Hilden J. Tools to aid decision-making in the care of pediatric patients with cancer. Am Soc Clin Oncol Ed Book. 2007;188-192.
- Masera G Chesler MA, Jankovic M, et al. SIOP Working Committee on psychosocial issues in pediatric oncology: guidelines for communication of the diagnosis. Med Pediatr Oncol. 1997;28(5):382-385.
- Makoul G, Winter RJ. MSJAMA Communication skills education in medical school and beyond. JAMA. 2003;289(1):93.
- Baile WF, Buckman R, Lenzi R, et al. SPIKES-A six step protocol for delivering bad news: application to the patient with cancer. Oncologist. 2000; 5(4):302-311.
- Scott MT, Todd KE, Oakley H. Reducing anesthesia and health care cost through utilization of child life specialists in pediatric radiation oncology. Intl J Radiat Oncol Biol Phys. 2016;96(1):401-405.
- Boman K, Lindahl A, Björk O. Disease-related distress in parents of children with cancer at various stages after the time of diagnosis. Acta Oncol. 2003;42(2):137-146.
- Mack JW, Wolfe J, Grier HE, et al. Communication about prognosis between parents and physicians of children with cancer: parent preferences and the impact of prognostic information. J Clin Oncol. 2006;24(33):5265-5270.
- Trask CL, Welch JJ, Manley P, et al. Parental needs for information related to neurocognitive late effects from pediatric cancer and its treatment. Pediatr Blood Cancer. 2009; 52(2):273-279.
- Ringnér A, Jansson L, Graneheim UH. Parental experiences of information within pediatric oncology. J Pediatr Oncol Nurs. 2011;28(4):244-251.
- Kilicarslan-Toruner E, Akgun-Citak E. Information-seeking behavior and decision-making process of parents of children with cancer. Eur J Oncol Nurs. 2013;17(2):176-183.
- Mack JW, Joffe S, Hilden JM, et al. Parents’ view of cancer-directed therapy for children with no realistic chance for cure. J Clin Oncol. 2008;26(29):4759-4764.
- Slevin ML, Stubbs L, Plant HJ, et al. Comparing view of patients with cancer with those of doctors, nurses and general public. BMJ. 1990;300(6737):1458-1460.
- Mulhern RK, Crisco JJ, Camitta BM. Patterns of communication among pediatric patients with leukemia, parents, and physicians: prognostic disagreements and misunderstandings. J Pediatr. 1981;99(3):480-483.
- Mack JW, Cook EF, Wolfe J, et al. Understanding of prognosis among parents of children with cancer: parental optimism and the parent-physician interaction. J Clin Oncol. 2007;28(11):1357-1362.
- Lamont EB, Christakis MA. Complexities in prognostication in advanced cancer “To help them live their lives the way they want to.” JAMA. 2003;290(1):98-104.
- Weeks JC, Cook EF, O’Day SJ, et al. Relationship between cancer patients’ predictions of prognosis and their treatment preferences. JAMA. 1998;279(21):1709-1714.
- Sisk BA, Kang TI, Mack JW. How parents of children with cancer learn about their children’s prognosis. Pediatrics. 2018;141(1):e20172241.
- Young B, et al. Parents’ experiences of their children’s presence in discussions with physicians about leukemia. Pediatrics. 2011;127.e1230e1238.
- Wiener L, Zadeh S, Wexler LH, Pao M. When silence is not golden: engaging adolescents and young adults in discussions around end-of-life care choices. Pediatr Blood Cancer. 2013;60:715-718.
- Bluebond-Langner M. The Private Worlds of Dying Children. Princeton, NJ: Princeton University Press; 1978.
- Wolfe J, Hammel JF, Edwards KE, et al. Easing of suffering in children with cancer at the end-of-life: Is care changing? J Clin Oncol. 2008;26(10):
- 1717-1723.
- Gaab EM, Owens GR, MacLeod RD. Siblings caring for and about pediatric palliative care patients. J Palliat Med. 2014;17(1):62-67.
- Kreicbergs UC, Lannen P, Onelov E, Wolfe J. Parental grief after losing a child to cancer: impact of professional and social support on long-term outcomes. J Clin Oncol. 2007;25(22):3307-3312.
- Kreicbergs U, Valdimarsdóttir U, Onelov E, et al. Care-related distress. a nationwide study of patents who lost their child to cancer. J Clin Oncol. 2005;23(36):9162-9171.
- Houlahan KE, Branowicki PA, Mack JW, et al. Can end of life care for the pediatric patient suffering with escalating and intractable symptoms be improved? J Pediatr Oncol Nurs. 2006;23(1):45-51.
- Hinds PS, Drew D, Fouladi M, et al. End-of-life care preferences of pediatric patients with cancer. J Clin Oncol. 2005;23(36):9146-9154.
- Martinson IM. Improving care of dying children. West J Med. 1995;163:258-262.
- Brown PG. Families who have a child diagnosed with cancer: what the medical caregiver can do to help them and them and themselves. Issues in Compr Pediatr Nurs. 1989;12(2-3):247-260.
- Sloper P, While D. Risk factors in the adjustment of siblings of children with cancer. J Child Psychol Psychiatr. 1996;37(5):597-607.
- Dias N, Brandon D, Haase JE, Tanabe P. Bereaved parents’ health status during the first 6 months after their child’s death. Am J Hosp Palliat Care. 2017. PMID: 29202599.
- Rosenberg AR, Baker KS, Syrjala K, Wolfe J. Systemic review of psychosocial morbidities among bereaved parents of children with cancer. Pediatr Blood Cancer. 2012;58(4):503-512.
- Hendrickson KC. Morbidity, mortality, parental grief: a review of the literature on the relationship between the death of a child and the subsequent health of the parents. Palliat Support Care. 2009;7(1):109-119.
- Dyregrov A, Dyregrov K. Long-term impact of sudden infant death: a 12- to 15 year follow-up. Death Stud. 1999;23:635-661.
- Saunders CM. A comparison of adult bereavement in the death of a spouse, child, and parent. Omega. 1979-1980;10:302-322.
- Stroebe M, Schut H, Stroebe W. Health outcomes of bereavement. Lancet. 2007;370(9603): 1960-1973.
- Kreicbergs U, Valdimarsdottir U, Onelov UVE, et al. Anxiety and depression in parents 4-9 years after the loss of a child owing to a malignancy: a population-based follow-up. Psychol Med. 2004; 34(8);1431-1441.
- Li J, Hansen D, Mortensen PB, Olsen J. Myocardial infarction in parents who lost a child: a nationwide prospective cohort study in Denmark. Circulation. 2002;106 (13):1634-1639.
- Li J, Johansen C, Hansen D, Olsen J. Cancer incidence in parents who lost a child: a nationwide study in Denmark. Cancer. 2002;95(1):2237-2242.
- Levav I, Friedlander Y, Kark JD, Peritz E. An epidemiolic study of mortality among bereaved parents. N Engl J Med. 1988;319;(8):457-461.
- Harper M, O’Connor RC, O’Carroll RE. Increased mortality in parents bereaved in the first year of their child’s life. BMJ Support Palliat Care. 2011;1(3):306-309.
- Gilmer MJ, Foster TL, Vannatta K et al. Changes in parents after the death of a child from cancer. J Pain Sympt. Manage. 2012;44(4):572-582.
- Rando TA. Bereaved parents: particular difficulties, unique factors, and treatment issues. Soc Work. 1985;30(1):19-23.
- deCinque N, Monterosso L, Dadd G, et al. Bereavement support for families following the death of a child from cancer: experience of bereaved parents. J Psychosoc Oncol. 2006;24(2):65-83.
- Institute of Medicine, National Research Council, National Cancer Policy Board. Foley KM, Gelband H, eds. Improving Palliative Care for Cancer: Summary and Recommendations. Washington, DC: National Academies Press; 2001.
- Hilden JM, Emanuel EJ, Fairclough DL, et al. Attitudes and practices among pediatric oncologists regarding end-of-life care: results of the 1998 American Society of Clinical Oncology survey. J Clin Oncol. 2001;19(1):205-212.
- Hui D, Elsayem A, De La Cruz M, et al. Availability and integration of palliative care at US cancer centers. JAMA. 2010;303:1054-1061.
- Tucker TL, Samant RS, Fitzgibbon EJ. Knowledge and utilization of palliative radiotherapy by pediatric oncologists. Curr Oncol. 2010;17(1):48-55.
- Mak KS, Lee SW, Balboni TA, Marcus KJ. Clinical outcomes and toxicity following palliative radiotherapy for childhood cancers. Pediatr Blood Cancer. 2018;65(1).
- Back AL, Arnold RM, Baile WF, et al. Efficacy of communication skills training for giving bad news and discussing transitions to palliative care. Arch Intern Med. 2007;167(5):453-460.
- Sulmasy DP, Cimino JE, HE MK, Frishman WH. U.S. medical students’ perceptions of the adequacy of their schools’ curricular attention to care at the end of life: 1998-2006. J Palliat Med. 2008;11:707-716.
- Bakst RL, Dunkel IJ, Gilheeney S, et al. Reirradiation for recurrent medulloblastoma. Cancer. 2011;117(21):4977-4982.
- Brown AP, Barney CL, Grosshans DR, et al. Proton beam craniospinal irradiation reduces acute toxicity for adults with medulloblastoma. Int J Radiat Oncol Biol Phys. 2013;56(2):277-284.
- Halperin EC, Cox EB. Radiation therapy in the management of neuroblastoma: the Duke University Medical Center experience 1967-1984. Int J Radiat Oncol Biol Phys. 1986;12(10):1829-1837.
- Chamberlain MC. Pediatric leptomeningeal metastases: Outcome following combined therapy. J Child Neurol. 1997;12 (1):53-59.
- Vern-Gross TZ. Pediatric palliative radiation oncology. In: Lutz S, Chow E, Hoskin P, eds. Radiation Oncology in Palliative Cancer Care. Chichester, UK: John Wiley & Sons, Ltd.; 2013;220-234.
Citation
T V. Comprehensive care for the child or adolescent diagnosed with a childhood malignancy requiring palliative radiation therapy. Appl Radiat Oncol. 2018;(2):7-17.
June 19, 2018