The treatment of scleredema with repeat radiation
Images
CASE SUMMARY
A 50-year-old man with a history of poorly controlled type 2 diabetes mellitus presented to the Texas Department of Corrections Dermatology clinic in 2004 with an 8-year history of worsening neck and upper-back skin thickening associated with pain, difficulty in turning his head, and pruritus over the involved skin. He was subsequently diagnosed with scleredema adultorum of Buschke associated with poor control of his diabetes based on clinical presentation and skin biopsy results from the back.
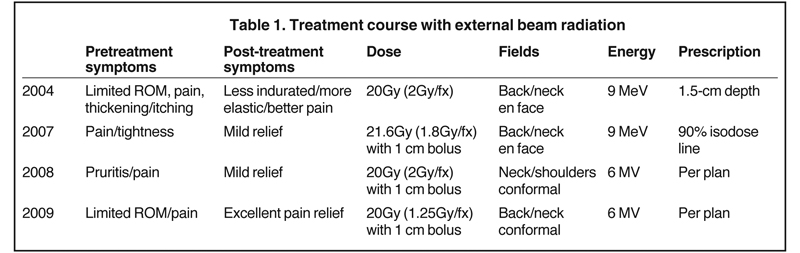
He was initially treated with topical treatments, but they failed and the patient was referred for external beam radiation. He received multiple rounds of radiation treatments from 2004 to 2009 due to the progressive nature of his disease in the setting of poorly controlled diabetes with varied response to treatment. A patchwork of radiation fields were used to prevent significant overlap when needed (Table 1). The patient tolerated treatments well, but did receive antihistamines for pruritus and aloe vera cream for skin erythema. Following his final round of treatment in 2009, the patient had excellent pain relief. His skin was less indurated and more elastic. He continues to use topical body lotion for postradiation changes and Benadryl for occasional pruritis. He has not required any further treatment and most likely will not receive additional radiation to previously treated areas based on the cumulative dose received.
DIAGNOSIS
Scleredema adultorum of Buschke associated with poor control of diabetes
DISCUSSION
Scleredema adultorum of Buschke is a skin condition that can occur in the setting of different medical aliments, but most commonly in poorly controlled diabetes mellitus. Its prevalence in diabetic patients has been reported up to 14%.1 It typically presents as diffuse, nonpitting, indurated skin with possible erythema and pain and is most commonly located in the posterior neck, scalp, and upper back. On histology, there is increased mucin deposition and widening of the collagen bundles in the reticular dermis.2,3 Treatment consists of multiple modalities, including topical cyclosporine, penicillin, methotrexate, psoralen, and UV-A (PUVA) and radiation therapy; however, no single treatment has proven to be effective in the majority of patients for a prolonged period of time.4
Radiation therapy has a variable history in the treatment of scleredema. Angeli Besson et al reported a case of scleredema treated with 20Gy in 10 fractions using electron beam therapy.5 Although a complete recovery was not accomplished, the patient had improved functional use of his legs and back and was able to stop systemic corticosteroid treatment. Tamburin et al used the same treatment schedule in a patient with scleredema associated with Type 1 diabetes mellitus.6 The patient received a total of 20Gy electron beam radiation therapy (EBRT) after failing initial treatment with corticosteroids. Following treatment with EBRT, the patient had both symptomatic relief and clinical regression, and remained disease free at time of publication. Lee et al provided further evidence for the use of EBRT.3 Two patients were treated. One received 24Gy in 2Gy per fraction and the other received 20Gy in 2Gy per fraction. They reported symptomatic and clinical improvement but not complete remission of disease. No major complications were reported. Tobler et al reported a case of scleredema in a diabetic patient.7 A total dose of 20Gy in 2Gy fractions was delivered via 12 MeV electrons. At 7 months, the patient had diminished skin thickening and maintained the improvement in range of motion. Bowen et al were among the first to report the effects of retreatment with radiation.8 Three patients were treated with 2 courses of either electrons or mixed photon/electron radiation. All 3 patients experienced improvement in shoulder abduction from pretreatment baseline. The patients treated with electrons experienced minimal side effects. However, the patient treated with mixed photon therapy developed sore throat, nausea, fatigue, and headache during treatment. This suggests the possibility that photon therapy may not be equivocal to electron therapy, as more side effects were noted with photons versus electron treatments. Konemann et al treated a diabetic patient with electrons twice in 6 months .9 A total of 20Gy in 2Gy fractions was delivered via 9 MeV electrons. The patient reported symptomatic improvement after the first treatment, but no clinical improvement was observed. The second course of treatment provided both symptomatic and clinical results.
CONCLUSION
These reports identify inconsistencies with the effectiveness of radiation to provide complete remission of disease in scleredema adultorum. However, they also show that symptomatic relief and some clinical response can occur for patients, even if only briefly. Treatment of scleredema with radiation has become the treatment of last resort for patients who do not respond to other treatments. Large radiation fields are used to cover affected areas. A tissue-equivalent bolus material is placed over the skin to bring dose to the surface and provide better coverage. The treatments are painless and last a few minutes. Benign skin pathology usually requires lower radiation dosages and shorter treatment courses than does malignancy, which reduces the risk of side effects. There are limitations when using EBRT to treat scleredema. Patients usually have to be retreated after symptoms recur. This increases the risk for radiation-induced side effects, which may occur acutely or years later. Some of the cutaneous complications with radiation used to treat other disorders are radiation-induced cancer, radiation dermatitis, acne, infections, and dyskeratosis.10 Because of the acute and late side effects of radiation, regular follow-up during and after treatment is required. The long-term effects of retreatment with EBRT have yet to be studied in scleredema. Nonetheless, radiation is an effective treatment option with regard to symptom improvement and quality of life.
REFERENCES
- Satter MA, Diab S, Sugathan TN, Sivanandasingham P, Fenech FF. Scleroedema diabeticorum: A minor but often unrecognized complication of diabetes mellitus. Diabet Med. 1998;5:465-468.
- Beers WH, Ince A, Moore TL. Scleredema adultorum of Buschke: A case report and review of the literature. Semin Arthritis Rheum. 2006;35:355-359.
- Lee MW, Choi JH, Sung KJ, Moon KC, Koh JK. Electron-beam therapy in patients with scleredema. Acta Derm Venereol. 2000;80:307-308.
- Meguerditchian C, Jacquet P, Beliard S, et al. Scleredema adultorum of Buschke: An under-recognized skin complication of diabetes. Diabetes Metab. 2006;32 (5 Pt 1):481-484.
- Angeli-Besson C, Koeppel MC, Jacquet P, Andrac L, Sayag J. Electron-beam therapy in scleredema adultorum with associated monoclonal hypergammaglobulinaemia. Br J Dermatol.1994;130:394-397.
- Tamburin LM, Pena JR, Meredith R, Soong VY. Scleredema of Buschke successfully treated with electron beam therapy. Arch Dermatol. 1998;134: 419-422.
- Tobler M, Leavitt DD, Gibbs FA Jr. Dosimetric evaluation of a specialized radiotherapy treatment technique for scleredema. Med Dosim. 2000;24:215-218.
- Bowen AR, Smith L, Zone JJ. Scleredema adultorum of Buschke treated with radiation. Arch Dermatol. 2003;139:780-784.
- Konemann S, Hesselmann S, Bolling T, et al. Radiotherapy of benign diseases – scleredema adultorum Buschke. Strahlentherapie und Onkologie. 2004;180:811-814.
- Carrotte-Lefebvre I, Delaporte E, Mirabel X, Piette F. Radiation-induced skin reactions (except malignant tumors). Bull Cancer. 2003;4:319-325.