RadiatingHope – A decade in global radiation oncology
Images





RadiatingHope (RH) was founded as a nonprofit organization in 2009, at a time when nongovernmental organizational engagement in global radiation oncology was in its infancy. Co-founders Larry Daugherty, MD, and Brandon Fisher, DO, were radiation oncology residents at the time. As avid mountain climbers, they visited some of the most amazing peaks in the world. On their journeys, they would seek out local hospitals and cancer care facilities, seeing that many of these incredible summits were in underserved low- and middle-income countries (LMICs). Most cancers were diagnosed at advanced stages; cancer care was scarce and access to radiation therapy (RT) was poor or often nonexistent. The number of nations without RT equipment was even greater at that time than the current estimates of 44 nations without RT and a worldwide shortfall of 5000 RT machines in LMICs.1-4 It was clear to Daugherty and Fisher that the challenges were not limited to equipment alone; radiation oncology personnel were few and training was difficult to access.
In this climate, under the mentorship of Dr. Luther Brady, RH forged its mission of improving radiation-oncology-related cancer care globally. Avenues to implement this vision quickly expanded to include advocacy, equipment donation, and education and training. At the heart of RH’s vision is to empower local communities and institutions through partnerships with RH, international medical personnel, and members of industry throughout the world.
Advocacy Mountaineering
RH may best be known as the group of radiation oncologists who climb mountains for cancer. These expeditions are a means to increase awareness about the condition of cancer care in LMICs and to further advance radiation oncology services. Each climb has a preset pledge amount; climbers raise tax-deductible funds, which are donated to the mission of advancing cancer care, often in the region of the climb. In the past 4 years, close to 300 climbers – including cancer survivors – have joined RH on the annual Kilimanjaro climb (Figure 1), as well as the Everest Base Camp (EBC) and Machu Picchu excursions. The 80 climbers for the 2017 RH EBC trek raised enough funds to purchase a high-dose-rate (HDR) afterloader for the Kathmandu Cancer Center (KCC) in Nepal.
Prayer Flag Project
On their expeditions, designated RH climbers carry Tibetan prayer flags that represent health, hope, strength and well-being. Flags are individually dedicated to cancer patients and are flown at the summit of each peak. So far, these flags have been to Mount Kilimanjaro, Mount Whitney, Mount Aconcagua, Mount Elbrus, Mount Rainier, Mount Washington, the Arctic Circle, Pico De Orizaba, Mount Chukkung Ri, Mount Denali and have now been left flying at EBC.
Equipment Donation, Education and Training
RH realized that its mission of equipment donation was possible when RT machines were donated to Madagascar (cobalt) and Peru (linac) through the Luther Brady Research Institute. With the project in Dakar, Senegal, RH took its first step into the unknown.
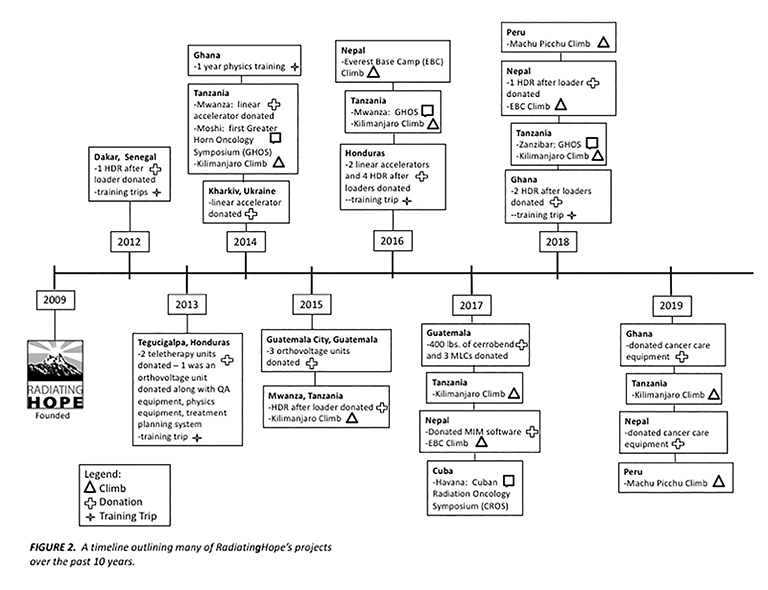
The RH projects in Senegal, Ghana, Honduras, Guatemala and Nepal include equipment donations and training programs to create self-sustainability as well as methods for training others. These endeavors are described in detail in the sidebar to the right; many other projects are listed in Figure 2.
Upcoming Projects
RH is working to help build a partnership with Kenyatta Hospital and Stanford University to create a paradigm for sustainable distance-based clinical learning and an HDR distance training program similar to the one in Ghana; in parts of Central and South America, RH is collaborating with Rayos Contra Cancer and Project ECHO to implement a similar program. Uniting with industry and an international builder, RH is working with Hospital Municipal La Portada in La Paz, Bolivia, to build and equip a start-up oncology center.
Symposia
Starting in March 2014, RH hosted its first international meeting – the Greater Horn Oncology Symposium (GHOS), in Moshi, Tanzania, at the Kilimanjaro Christian Medical Centre (KCMC). GHOS serves as a multidisciplinary oncology forum for improving access to cancer care in the Greater Horn of Africa and to create a platform for exchanging ideas among oncology medical professionals around the globe. The second GHOS was held in June 2016 in Mwanza, Tanzania, in collaboration with Bugando Medical Center, and the third in June 2018 in Zanzibar. At the Zanzibar conference, 15 nations were present (Africa - 8, North America - 2, Europe - 4, South Asia -1). Of the 56 attendees, 29 were from Africa, 1 was from Nepal and the remainder were from North America and Europe (Figure 3). Ten participants were radiation oncology residents from Ocean Road Cancer Institute in Dar es Salaam, Tanzania, who had the opportunity to speak directly with international experts in radiation oncology. By bringing together this group of radiation oncologists (ROs), medical physicists (MPs), radiation therapists (RTTs), and members of industry for 3 days, GHOS has sparked collaborations among institutions in North America or Europe and LMICs present at the meeting, and among African nations to help create self-sustaining collaborations in developing local cancer care. Examples include partnerships between physicians in Tanzania and Turkey, as well as ties between institutions in Switzerland and Senegal to advance from 2D to 3D planning. The next GHOS is in June 2020.
A similar meeting – the Cuban Radiation Oncology Symposium (CROS) – was planned for October 2017 in Havana, Cuba. Due to US state department travel recommendations at the time, few US participants attended the meeting; however, more than 20 Cuban ROs were present.
These symposia are largely funded with assistance from industry members, such as Varian (Palo Alto, California) and Elekta (Stockholm, Sweden), covering the travel and lodging expenses of local conference participants; all North American and European participants have managed their own expenses.
Challenges
While undertaking global radiation oncology work, the list of challenges quickly outpaces the list of successes. As is clear from the few projects discussed above, equipment alone is not the only piece of the puzzle missing in advancing global oncology care. The current projected need of these medical personnel in LMICs by 2035 is greater than 10 000 ROs, 9000 MPs and 25 000 RTTs.8 Training sites for these highly specialized individuals are difficult to access, as evidenced by Ghanaian physicists receiving training in China.
Regarding equipment, several nations will not accept used or refurbished RT equipment (including machines and physics equipment). For countries that do, not all donations have been or can be utilized. An institution may have a bunker to hold the machines, but may not have the infrastructure or resources to deploy the equipment. Prior to donating equipment (including machines, treatment applicators, software, etc.), RH undertakes thorough, in-person research of the receiving site in regard to space/bunker availability and appropriateness for equipment, medical personnel availability, medical personnel knowledge, financial stability, energy source stability, local government support, and maintenance for optimal use of equipment. Additionally, contracts are signed for agreement and sustained communication. However, despite these painstaking efforts, not all projects are completed. The 2 orthovoltage units donated to Central America are in storage due to costs of making the units functional, as is the case of the MLCs waiting to be installed in Guatemala. The linac donated to the Bugando Medical Center in Tanzania still sits in crates due to assembly costs required by the manufacturer and the Ministry of Health’s challenges in meeting these demands. Furthermore, governments here are often slower to respond and leadership can change frequently, setting back progress. The donation at the Kharkiv Institute in Ukraine could not be reassembled; however, it was used for parts to update linacs throughout the country.
In Dakar, where the HDR afterloader was successfully installed, used and maintained, several challenges remained with continued operation of the unit, including the cost and logistical difficulty with source changes, limited RO and treatment room time availability for procedures, and equipment downtime, which can be significant. Sustained communication with some sites after donation can also become difficult.
Last, but by no means least, shipping linacs and HDR afterloaders is no small feat. Disassembling a linac, transporting it to storage, shipping it overseas, and transporting it to a facility, can take months, sometimes longer, to reassemble and make functional. These steps depend on the availability of manufacturers in the region, and their ability to put into motion refurbished/used equipment with local government support.
RadiatingHope past projects
Senegal Project — Lead: Adam Shulman, MS
In 2012, RH identified the Institut Curie at L’Hôpital Aristide Le Dantec in Dakar, Senegal, as a site in need of brachytherapy for the treatment of cervical carcinoma. West Africa has one of the highest rates of cervical cancer in the world.5 Institut Curie, with more than 500 cases of cervical cancer to treat annually, had a single cobalt teletherapy machine, a fluoroscopic simulator, 2 radiation oncologists (ROs), 3 medical physicists (MPs), 1 nurse (RN) and 2 radiation therapists (RTTs) to serve the RT needs of Senegal and 4 adjacent nations. Unfortunately, the center had no brachytherapy. The treatment paradigm for carcinoma of the cervix was surgery for early stage disease and either palliative hypofractionated radiation and chemotherapy or neoadjuvant chemotherapy/radiation therapy followed by surgery for more advanced disease. Definitive chemoradiotherapy was not an option for curative treatment of the disease.
RH facilitated the donation of a refurbished HDR afterloader to the Institut Curie in December of 2012, when a team from RH (ROs, MPs and RNs) traveled to Senegal for HDR brachytherapy training. The ROs in Dakar were previously trained in placement of low-dose-rate brachytherapy applicators. The trip focused on developing fractionation schedules and a treatment planning process that would be feasible with the limited resources; the afterloader would be housed in the cobalt bunker limiting treatment time, and no CT simulator was available. To optimize resources, while trying to minimize toxicity, a hypofractionated regimen of 3 fractions of 7.5 Gy was chosen. The treatment planning process has been described previously and consisted of using fixed-geometry tandem and ring applicators with a library of plans corresponding to each geometry.>6 After insertion, patients underwent conventional simulation with orthogonal radiographs and isodose overlay transparencies were used to estimate ICRU (International Commission on Radiation Units) rectal and bladder point doses.
In March 2013 a second RH team (ROs, MPs and RN) assisted in performing the first 10 brachytherapy procedures. The process worked efficiently, was reproducible and was easily adopted by the team in Dakar. Over the next 3 years 62 patients with cervical cancer were treated using this approach with acceptable control and toxicity rates.7 Further work is being explored including a prospective clinical trial using both hypofractionated external-beam radiation and a hypofractionated brachytherapy schedule to further optimize throughput of cervical cancer patients. The training provided to the Dakar team carries on as this center has new linacs and HDR afterloaders; the medical personnel are engaged in training new ROs and MPs. RH continues to fund these efforts and has supported a training trip for the MPs to spend 1 week at the Karmanos Cancer Institute in Detroit.
Ghana Project — Lead: Adam Shulman, MS
RH began to build a relationship with the Sweden Ghana Medical Centre (SGMC) in Accra when Shulman was working as an MP there from August 2014 to August 2015. He worked alongside hospital administration and staff to ensure the establishment of SGMC as a free regional training center for MPs across Sub-Saharan Africa. SGMC is a comprehensive cancer center with medical and radiation oncology as well as primary care. The radiation oncology department has modern equipment including: a linac with MV imaging, treatment planning software, a record and verify system; a 16-slice CT sim, and a 0.3T MRI sim. Department staffing consists of: 2 ROs (1 completed residency in Canada, and 1 completed residency in Accra at Korle Bu Teaching Hospital); 2 MPs (with MS degrees in medical physics from the School of Nuclear and Allied Sciences, University of Ghana, Legon); 1 physics student (in medical physics MS program at Duke Kunshan University in China as of press time); 1 dosimetrist (an RTT trained on dosimetry), 4 RTTs; and 1 diagnostic radiologist (from the University of Ghana).
Training focused on safety with attention to areas with greatest risk for systematic and/or large errors, in addition to working with staff to develop an in-depth understanding of all aspects of clinical workflow and tasks. Process management was emphasized as an essential element of quality assurance (QA) and treatment planning. With his experience in Africa over the past decade, Shulman believes the most effective way to improve clinical understanding, while simultaneously optimizing safety and efficiency, is by introducing standard procedures, documents, and Excel spreadsheets, and by customizing them during training. In this technique, each document is introduced individually, and modified as necessary line by line accounting for the site’s environment, staffing, workload, equipment, etc. Through this process, the trainees not only learn exactly why each line is written, but how it is done, while creating a guideline to follow in the future. An invaluable teaching tool, this method of standardization has the additional benefit of facilitating communication among sites trained by RH and RH trainers, allowing for easier discussion and streamlined troubleshooting. Opening doors for communication among African countries and the world is priceless, as one of the largest difficulties faced by many MPs in Africa is isolation. Ultimately, the SGMC staff was trained in theory, clinical use, safety and efficiency. They learned QA on linacs and imaging devices, treatment planning, secondary checks and monitor unit (MU) calculations. They were also trained on data collection and measurement device selection, and performed multiple sessions of annual QA work on all equipment.
The CEO of SGMC and professional staff had agreed to provide free training to MPs across Africa upon completion of this year-long training. This project passed the self-sustainability test when the SGMC MPs trained an MP from Senegal for 2 weeks, educating her on all of the equipment and procedures they had learned; she reported she learned more in 2 weeks at SGMC than she had in 2 months in France. Similarly, an external audit was performed by MPs from South Africa. They stated that the physics program led by the 2 Ghanaian MPs was as good as any physics program in South Africa. Since 2015, the physics team in Ghana has trained MPs from Ghana, Senegal, Nigeria, and Kenya for up to 3 months at a time; RH has received positive feedback from all MPs who trained at SGMC.
Recently, SGMC acquired a cobalt HDR unit, and the Komfo Anokye Teaching Hospital in Kumasi, Ghana, received 2 HDR afterloaders donated with assistance from RH. Using the same principles outlined above, a distance training program for HDR brachytherapy has been implemented for the Ghanaian MPs; RH has provided template documents on all aspects of HDR brachytherapy, from commissioning to source exchange to EQD2 documents and checklists. In the summer of 2018, a 2-week, in-person, RO and MP training was held in Ghana; distance training continues.
Central America Project – Lead: Peter Sandwall, PhD
Honduras
In 2011 a pair of independent, volunteer physicists traveled to Tegucigalpa, Honduras, to ensure the team at the Centro Oncologico Hondureño could use a donated planning system (Pinnacle [Royal Phillips, Amsterdam, the Netherlands]) with their recently purchased linac – a 600C (Varian, Palo Alto, California), the first in the city and second in the country. The linac’s multileaf collimator (MLC) system was destroyed in shipment, necessitating the use of cerrobend blocks for 3-dimensional (3D) treatments.
Over the years, RH has been able to facilitate several equipment donations to Honduras, including an orthovoltage machine, a daily QA device, miscellaneous physics equipment, and a newer Pinnacle treatment planning system. In 2017, RH received a large donation (valued at more than $1,000,000); 2 high-energy linacs and 4 HDR afterloaders were shipped via container to Tegucigalpa. Upon receiving this donation, the first project was to transfer one of the linac heads (including MLC) to the 600c in operation at Centro Oncologico Hondureño. The construction of a second vault is being explored to house the other linac. Sandwall is working with San Felipe, a public hospital, to place the HDR units at this location.
This 2017 donation, along with other physics equipment, has facilitated installation of a Varian 2100EX at Hospital Bendaña in San Pedro Sula in 2018; the process of commissioning served as an educational opportunity for the local physics community. Independent initiatives in Honduras continue for the performance of annual QA and reference dosimetry on the accelerator. The internal efforts to improve medical use of radiation in Honduras are becoming more robust by a new generation of MPs. Several trained outside of their home country (Mexico and Italy) and are creating opportunities for hands-on education and academic training at home (Figure 4).
Guatemala
An orthovoltage unit was donated and shipped by RH to Liga Nacional Contra el Cancer/Instituto Nacional de Cancerologia (LIGA/INCAN) in Guatemala City, Guatemala, in 2015. Following this donation, RH and an RO, made a trip to this center for a needs assessment; LIGA/INCAN was equipped with 2 linacs and an aging cobalt unit, both without MLCs, and they were suffering a cerrobend shortage. With the help of RH, 400 lbs of cerrobend and MLCs were shipped to this center. In addition to the above-mentioned equipment, in 2018 an Elekta (Stockholm, Sweden) Monaco treatment planning system was given to RH and sent to LIGA/INCAN. In Guatemala, RH is working closely with Rayos Contra Cancer, another nongovernmental organization focused on advancing global radiation oncology-related cancer care.
Nepal Project — Lead: Brandon Fisher, DO
Nepal, a country of 26 million people in the heart of the Himalayas, and home to the highest mountains in the world including Mt. Everest, faces a similarly enormous feat to climb with access to cancer care. With this population, you could justify well over 100 radiation machines; however, Nepal only has only 4 functioning machines (2 cobalt and 2 linacs). RH began working with Nepal in 2016 in partnership with the Kathmandu Cancer Center (KCC) and Dr. Subhas Pandit, with the goal of implementing brachytherapy to provide definitive and curative treatments for cervical cancer – the most common cancer treated at the center. KCC uses state-of-the-art external-beam radiation therapy, pulling off technically demanding plans, using 3D planning and intensity-modulated radiation therapy. Their linac runs around the clock – and is powered by a generator during power shortages. Unfortunately, KCC lacked funds to purchase a brachytherapy machine. RH was scheduled to receive 2 donated machines to be shipped and installed at KCC in 2017; however, the government restricted entry of used machines. Committed to providing brachytherapy to KCC, RH partnered with Varian to purchase a new HDR afterloader, which was installed in March 2019 (Figure 5); the EBC trekkers in 2017 (Figure 6) raised over $100K, which was used to purchase this unit. KCC has received their radioactive source and completed its first 4 brachytherapy treatments for cervical cancer on May 1, 2019. Part of ongoing efforts to support the cancer center include annual medical missions to the center and frequent EBC treks; an RH training trip is scheduled in December with ROs and MPs.
Conclusions
RH’s vision remains clear, and its devotion to increasing access to global radiation oncology care runs deep, strengthened by the incredible individuals engaged in the work and their dedication to help provide cancer care to their family and friends. Since its inception in 2009, RH has learned much along its journey of advancing global cancer care and has encountered seemingly insurmountable difficulties. The importance of collaboration worldwide is obvious during the times of these impossible-appearing summits. As RH climbers have adopted a “climb on” mantra when facing obstacles on a trek, so too has the global oncology world.
Acknowledgements
RH Board of Directors
John P. Einck, MD (president), Tom Ladd (executive director), Tosh Rymer (treasurer), Mira M. Shah, MD (vice president)
RH Board of Trustees
Ashley Cogswell, Ron DiGiaimo, MBA, FACHE, Arno J. Mundt, MD, Shilpen Patel, MD, Adam Shulman, MD
RH Society President
Arno J. Mundt, MD
RH Board Members
George Felis Acquah, MS, Derek Brown, PhD, Brandi Page, MD, David Snow, Ben Wilkinson, MD
Equipment Donors in projects referenced in this article
University of Minnesota, Mayo Clinic, Rutland Regional Medical Center, Connecticut X-Ray, Horizon Medical Services Florida, Willis-Knighton, First Dayton Cancer Care.
Volunteers
Angela Babbo, MD, Anuja Jhingran, MD
References
- DIRAC/IAEA database. https://dirac.iaea.org/2016. Accessed October 1, 2018.
- Abdel-Wahab M, Fidarova E, Polo A. Global access to radiotherapy in low- and middle-income countries. Clin Oncol. 2017;29(2):99-104.
- IAEA brochure. https://cancer.iaea.org/documents/AGaRTBrochure.pdf. Accessed October 1, 2018.
- IAEA outreach materials. https://www.iaea.org/services/key-programmes/programme-of-action-for-cancer-therapy-pact/outreach-materials. Accessed October 1, 2018.
- Bray F, Ferlay J, Soerjomataram I, et al. Global cancer statistics 2018: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J Clin 2018;68(6):394-424.
- Einck J, Hudson A, Shulman A, et al. Implementation of a high-dose-rate brachytherapy program in Senegal: a pragmatic model for the developing world. Int J Radiat Oncol Biol Phys 2013;89(3):462-467.
- Personal communication.
- Atun R, Jaffray DA, Barton MB, et al. Expanding global access to radiotherapy. Lancet Oncol. 2015;12:1153-1186.
Citation
MM S, JP E, T L, AJ M, A S, P S, L D, B F. RadiatingHope – A decade in global radiation oncology. Appl Radiat Oncol. 2019;(2):27-32.
July 11, 2019