Nasopharyngeal stenosis following curative chemoradiation therapy for oropharyngeal cancer in a patient with active oral lichen
Images


BACKGROUND
Lichen planus is an inflammatory disorder of immune dysregulation that affects the skin and mucosa. Oral lichen planus (OLP) is a chronic variant characterized by white mucosal lesions,1 most commonly with bilateral buccal mucosa involvement and frequently involving the tongue and gingiva as well.2 Although the underlying cause remains obscure, OLP is thought to have an autoimmune etiology and has been linked with genetic factors, hypertension, diabetes mellitus, hepatitis C virus, and thyroid dysfunction.3
OLP onset involves the activation of immune pathways leading to migration and activation of T cells and the destruction of keratinocytes.4 It is thought that oral mucosal keratinocytes are activated by the expression of unknown antigens, which recruit lymphocytes. This T-cell-mediated response is coupled with the simultaneous nonspecific response of matrix metalloproteases, chemokines and mast cells, together causing apoptosis of the basal keratinocytes by various mechanisms.
OLP can undergo malignant transformation to oral squamous cell carcinoma (OSCC) in a small subset of OLP patients (1%), more commonly in smokers, alcoholics, and hepatitis C patients.5 It is thus considered an OSCC precursor lesion. Topical steroids are the first-line treatment, but systemic steroids and topical calcineurin inhibitors can be used to manage recalcitrant cases.6
Oral and oropharyngeal SCC are commonly treated with surgery and/or radiation and chemotherapy, which cause adverse reactions including mucositis, xerostomia, dysphagia, dysgeusia, and thrush. These toxicities can persist weeks to months following treatment, and severity is correlated with the chemoradiation (CRT) dose.7 Pharyngoesophageal stenosis, a late effect, can significantly compromise quality of life, often necessitating parenteral nutrition.8
In this report, we present a case of a patient with active OLP for 26 years who was diagnosed with HPV-associated oropharyngeal SCC and treated with CRT. Following treatment, nasopharyngeal stenosis and dysphagia developed.
CASE SUMMARY
A 63-year-old woman presented to her physician with a sore throat, dysphagia and an enlarged left neck lymph node. She had a 26-year history of OLP for which she followed regularly with a dentist. She has a 7.5 pack-year smoking history and quit 25 years before presentation.
After fine-needle aspiration of the lymph node raised suspicion for malignancy, the patient was referred to a head-and-neck surgeon. Examination identified white oral patches consistent with OLP. In addition, an exophytic left base of tongue (BOT) lesion was visible (Figure 1A). Nasopharyngoscopy showed no involvement of the tonsils or right BOT.
IMAGING FINDINGS
Computed tomography (CT) of the neck confirmed a left BOT mass with inferior extension to the vallecula, crossing the left glossotonsillar sulcus. A 2.5-cm left level IIA cervical nodal involvement and smaller adenopathy in left level IIB and left level III were identified. A PET/CT (positron emission tomography/CT) showed hypermetabolic activity in the left BOT and the identified left neck lymph nodes.
DIAGNOSIS
A biopsy of the BOT confirmed a diagnosis of AJCC (American Joint Committee on Cancer) 7th edition stage cT2N2bM0 HPV-positive SCC of the oropharynx (overall stage IVA).
TREATMENT
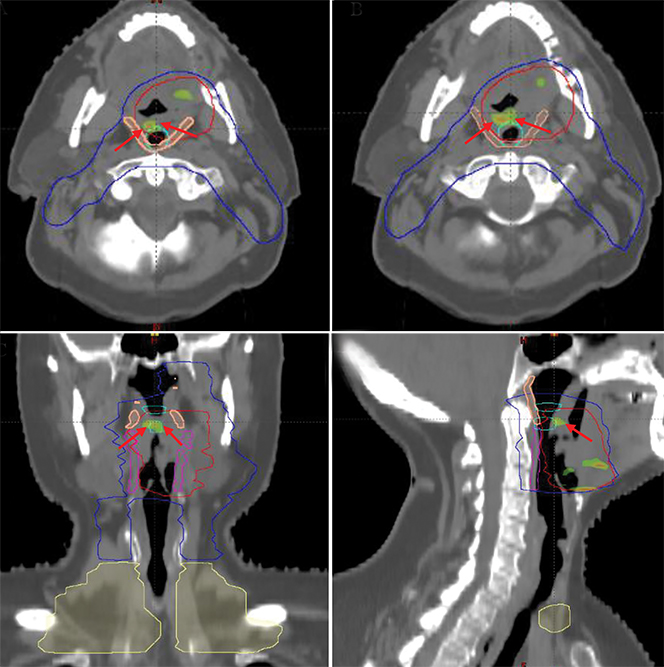
The patient underwent concurrent CRT to a total dose of 7000 cGy over 33 fractions, with cisplatin 100 mg/m2 delivered on days 1, 22, and 43 of radiation. The radiation technique was intensity-modulated radiation therapy (IMRT) with volumetric-modulated arc therapy (VMAT) and a simultaneous integrated boost. Target volume coverage was excellent, with planning target volume (PTV) 7000 D 95% = 6800 cGy. Doses to organs at risk were minimized while prioritizing optimal PTV coverage. Dose to nearby superior constrictor muscles were mean 6361 cGy and max dose 7336 cGy, and middle constrictors received mean 6650 cGy and max 7415 cGy. Hot-spot dose closest to the area that developed stenosis was 105%, or 7350 cGy (Figure 1B).
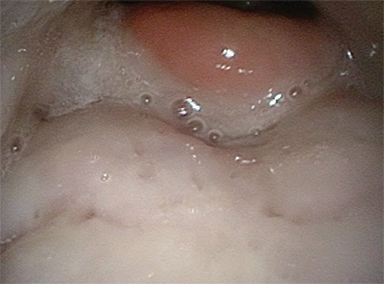
Treatment was completed without breaks. She experienced the following expected side effects: grade 3 mucositis (Figure 2); grade 2 dysphagia, dermatitis, dysgeusia, constipation; and grade 1 pruritis, neck edema, nausea, xerostomia, and salivary duct inflammation. She was able to tolerate soft and some solid foods during the treatment course. Karnofsky Performance Score was stable at 80% to 90% throughout the course, and oral analgesics were not required. She lost 11.5% of her body weight during CRT.
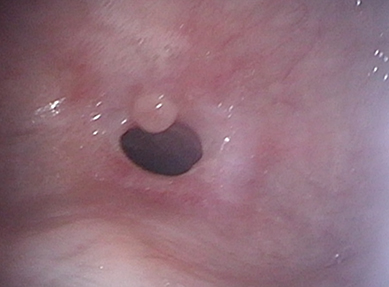
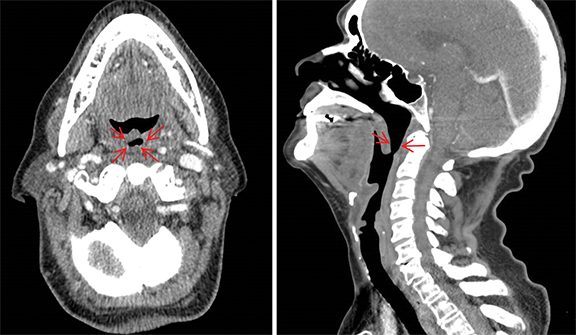
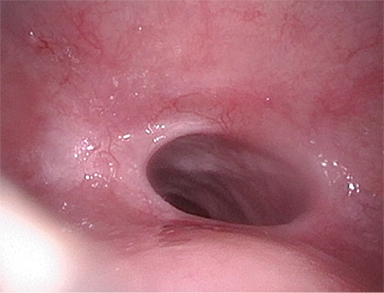
During follow-up, she had no evidence of disease clinically and radiographically on PET/CT scan, and she experienced improvement in saliva production and gustation. However, she complained of dysphagia at the conclusion of CRT without improvement 8 months later. She could not eat large portions or gain weight, and experienced dyspnea while eating. Nasopharyngoscopy revealed marked stenosis of the pharyngeal inlet at the level of the inferior nasopharynx (Figure 3). Specifically, there was moderate narrowing of the inlet to the oropharynx, with an approximately 1 cm opening (normal inlet opening: ≥ 3 cm). Mucosal surfaces were notable for telangiectasias and post-RT fibrosis. True vocal cords, supraglottis, and hypopharynx appeared normal.
The patient’s surgical oncologist initiated a conservative regimen of intranasal inhaled steroids twice a day and nasal saline 4 times a day, which led to gradual improvement. A percutaneous endoscopic gastrostomy tube was not inserted. A year later, she reported subjective swallowing improvement for the first time. Eighteen months after initiating this regimen, she tolerates soft foods without difficulty and repeat nasopharyngoscopy demonstrates a wider nasopharyngeal opening with less circumferential stenosis (Figure 4).
DISCUSSION
Long-term dysphagia as a result of radiation-related stenosis is an uncommon complication of CRT typically observed in patients with hypopharyngeal malignancies. Nasopharyngeal stenosis is rarer, although it has been reported in cases of RT for nasopharyngeal carcinoma.9 It is unclear why mucosal injury from CRT resolves spontaneously in some patients while it progresses to stenosis/stricture in others.10 Nonradiation risk factors for stricture include chemotherapeutic agents, tumor characteristics, age, sex, and patient co-morbidities. We believe that OLP was a risk factor for this patient’s stenosis. Radiation-related factors shown to contribute to pharyngoesophageal stricture, a similar post-CRT complication, include dose, fractionation, target, and technique.11 The structures at risk during radiation that can lead to long-term dysphagia are the constrictor muscles, the BOT, the larynx, the upper esophageal sphincter, and esophagus.12 Efforts should be made during planning to reduce the dose to these structures, particularly the constrictor muscles.13 Different CRT delivery may have prevented this complication; for example, radiation fraction size (212 cGy) should be limited to ≤ 200 cGy. In addition, weekly cisplatin dosing is less likely to cause severe mucositis14 and therefore may lead to less permanent dysphagia. In this particular patient, hotspots were not excessively high (105%). We did not prioritize constrictor muscle dose constraints over PTV coverage. As a result, the constrictors received a high mean and maximum dose. These doses may have contributed to the development of the localized stenosis in this region. However, we have never at our institution observed a similar complication in any of the dozens of oropharyngeal and nasopharyngeal cancer patients who receive similarly high doses to this region; therefore, this case exhibits a rare complication. We hypothesize that the chronic inflammatory state of oral lichen planus is related to this unusual complication. It is unclear if reducing constrictor dose would have made a difference in the setting of the chronic inflammatory state.
In this case, our patient had active OLP during CRT. The patient had known disease in the oral cavity, but additional inflammatory involvement of the pharynx is possible. Although less common than oral involvement, lichen planus can involve any mucosal surface and there are reports of LP affecting laryngeal and esophageal mucosa.15,16 Esophageal lichen planus is becoming increasingly recognized and is reportedly seen in a quarter of patients with OLP, often with patients complaining of dysphagia.17 The presence of this disease process close to the radiation field could have created subclinical pharyngeal mucosal disease or an inflammatory milieu that contributed to severe mucosal injury, ultimately leading to nasopharyngeal stenosis. In the setting of an autoimmune process such as OLP, the radiation-induced inflammation of the oral/pharyngeal mucosa may lead to hyperactive immune response, resulting in fibrosis and stricture formation during recovery. To our knowledge, this mechanism has not yet been reported. It is unclear if the HPV association of this tumor plays any role in the aforementioned inflammatory response.
Treatment of pharyngeal stenosis requires knowledge of its cause and severity. Nasal steroids were used in this case because the stenosed area was accessible to inhaled medication and because the patient experienced sinonasal symptoms secondary to the stenosis. Conservative treatment here was effective and durable. Strictures refractory to medical therapy are amenable to serial dilation. Deeper tissue injury and scarring can also occur following aggressive CRT,18 and treatment options available for these cases include balloon dilation and reconstructive surgery.
CONCLUSION
We report a case of long-term nasopharyngeal stenosis and dysphagia post-CRT for HPV-related OPSCC in a patient with a long history of active OLP. Her inflammatory state combined with radiation-induced fibrosis likely led to stenosis, which lasted almost 2 years before conservative treatment eventually improved symptoms. We advise that OLP patients who will receive RT/CRT undergo pre-treatment multidisciplinary consultation with their oncologists and dentist to select an ideal treatment paradigm for their unique conditions. This proactive approach may prevent pharyngeal stenosis and dysphagia post-CRT in the setting of chronic inflammatory conditions such as OLP.
REFERENCES
- Xiao C, Hanlon A, Zhang Q, et al. Risk factors for clinician-reported symptom clusters in patients with advanced head and neck cancer in a phase 3 randomized clinical trial: RTOG 0129. Cancer. 2014;120(6):848-854.
- Ismail SB, Kumar SK, Zain RB. Oral lichen planus and lichenoid reactions: etiopathogenesis, diagnosis, management and malignant transformation. J Oral Sci. 2007;49(2):89-106.
- Alrashdan MS, Cirillo N, McCullough M. Oral lichen planus: a literature review and update. Arch Dermatol Res. 2016;308(8):539-551.
- Payeras MR, Cherubini K, Figueiredo MA, Salum FG. Oral lichen planus: focus on etiopathogenesis. Arch Oral Biol. 2013;58(9):1057-1069.
- Aghbari SMH, Abushouk AI, Attia A, et al. Malignant transformation of oral lichen planus and oral lichenoid lesions: a meta-analysis of 20095 patient data. Oral Oncol. 2017;68:92-102.
- Al-Hashimi I, Schifter M, Lockhart PB, et al. Oral lichen planus and oral lichenoid lesions: diagnostic and therapeutic considerations. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2007;103 Suppl:S25.e21-12.
- Minhas S, Kashif M, Altaf W, Afzal N, Nagi AH. Concomitant-chemoradiotherapy-associated oral lesions in patients with oral squamous-cell carcinoma. Cancer Biol Med. 2017;14(2):176-182.
- Urken ML, Jacobson AS, Lazarus CL. Comprehensive approach to restoration of function in patients with radiation-induced pharyngoesophageal stenosis: report of 31 patients and proposal of new clasification scheme. Head Neck. 2012;34(9):1317-1328.
- Bonfils P, de Preobrajenski N, Florent A, Bensimon JL. Choanal stenosis: a rare complication of radiotherapy for nasopharyngeal carcinoma. Cancer Radiother. 2007;11(3):143-145.
- Prisman E, Miles BA, Genden EM. Prevention and management of treatment-induced pharyngo- oesophageal stricture. Lancet Oncol. 2013;14(9):e380-386.
- Best SR, Ha PK, Blanco RG, et al. Factors associated with pharyngoesophageal stricture in patients treated with concurrent chemotherapy and radiation therapy for oropharyngeal squamous cell carcinoma. Head Neck. 2011;33(12):1727-1734.
- Eisbruch A, Schwartz M, Rasch C, et al. Dysphagia and aspiration after chemoradiotherapy for head-and-neck cancer: which anatomic structures are affected and can they be spared by IMRT? Int J Radiat Oncol Biol Phys. 2004;60(5):1425-1439.
- Duprez F, Madani I, De Potter B, Boterberg T, De Neve W. Systematic review of dose--volume correlates for structures related to late swallowing disturbances after radiotherapy for head and neck cancer. Dysphagia. 2013;28(3):337-349.
- Mackiewicz J, Rybarczyk-Kasiuchnicz A, Lasinska I, et al. The comparison of acute toxicity in 2 treatment courses: three-weekly and weekly cisplatin treatment administered with radiotherapy in patients with head and neck squamous cell carcinoma. Medicine (Baltimore). 2017;96(51):e9151.
- Rennie CE, Dwivedi RC, Khan AS, Agrawal N, Ziyada W. Lichen planus of the larynx. J Laryngol Otol. 2011;125(4):432-435.
- Al-Shihabi BM, Jackson JM. Dysphagia due to pharyngeal and oesophageal lichen planus. J Laryngol Otol. 1982;96(6):567-571.
- Dickens CM, Heseltine D, Walton S, Bennett JR. The oesophagus in lichen planus: an endoscopic study. BMJ. 1990;300(6717):84.
- Franzmann EJ, Lundy DS, Abitbol AA, Goodwin WJ. Complete hypopharyngeal obstruction by mucosal adhesions: a complication of intensive chemoradiation for advanced head and neck cancer. Head Neck. 2006;28(8):663-670.
Citation
L M, J F, DP K, N S, S T. Nasopharyngeal stenosis following curative chemoradiation therapy for oropharyngeal cancer in a patient with active oral lichen . Appl Radiat Oncol. 2019;(3):50-53.
July 11, 2019