Adaptive replanning of IMRT for head and neck cancer
Images
Case Summary
A 39-year-old male presented with a right-sided neck mass and sore throat. The patient was placed on antibiotics initially with no resolution in symptoms. The neck mass continued to enlarge and the patient was noted to have erythema of the right tonsil. Fine-needle aspiration of the right neck mass demonstrated atypical cells, prompting an examination under anesthesia and right-sided simple tonsillectomy for further evaluation. Pathology from the excised tonsil demonstrated a moderate to poorly differentiated, human papillomavirus (HPV)-positive, p16-positive, squamous cell carcinoma. The patient was referred to radiation oncology for definitive treatment of tonsillar bed and neck disease.
Imaging Findings
Computed tomography (CT) imaging of the neck with contrast demonstrated a 3.0-cm × 1.3-cm × 2.3-cm right level IIA, cystic nodal mass, and 2 adjoining, enlarged right level IIB lymph nodes measuring 1.4 cm × 1.6 cm and 1.2 cm × 0.9 cm. 18F-2-fluoro-2-deoxyglucose positron emission tomography/computed tomography (FDG PET/CT) imaging revealed symmetric FDG uptake within the bilateral tonsillar fossae along with FDG-avid left level IIA nodes, 1.0 × 1.4 cm (SUVmax of 3.7) and 1.3× 1.4 cm (SUVmax of 3.8), right level II-V cystic node 4.3 × 4.2 × 3.4 cm (SUVmax 28.3) and right level IV node 1.0 × 1.2 cm (SUVmax of 4.3). No evidence of distant metastases was observed. On a clinical neck examination, an 8 × 7-cm right level II-V neck mass was noted, with no additional palpable nodes. Tumor staging for this patient was T1N3M0 or AJCC stage grouping, IVB.
Diagnosis
HPV-positive squamous cell carcinoma of the right tonsil
Treatment Summary
A 7-field, step-and-shoot, intensity-modulated radiation therapy (IMRT) technique was utilized, treating to a dose of 72 Gy in 40 fractions at 1.8 Gy per fraction over 8 treatment weeks with concurrent cisplatin and 5-FU chemotherapy given in-house on weeks 1 and 4 of IMRT. Daily image-guided radiation therapy (IGRT) with cone-beam CT imaging (CBCT) ensured setup accuracy. Treatment planning margins included a 3-mm expansion from gross tumor volume (GTV) to clinical target volume (CTV-72), and a 3-mm additional expansion of CTV-72 to PTV-72 for both the initial plan and adaptive replan, making total expansion of 6 mm from GTV to PTV-72.
An adaptive radiation therapy (ART) planning CT scan in the treatment position occurred at fraction number 20 of 40, with implementation of the adapted IMRT plan starting on fraction 21. There was no interruption or delay in the patient’s course of radiation during the ART replanning process.
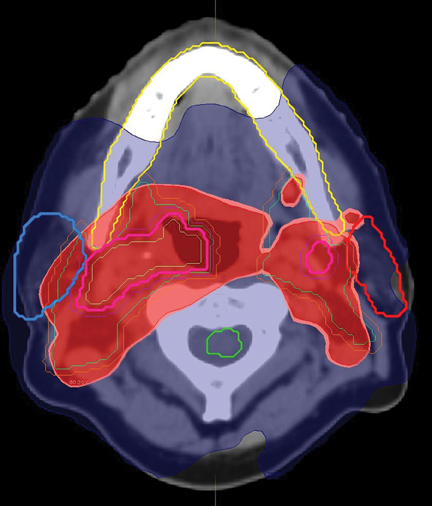
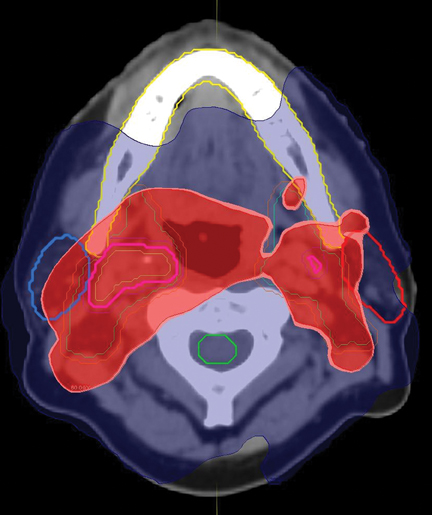
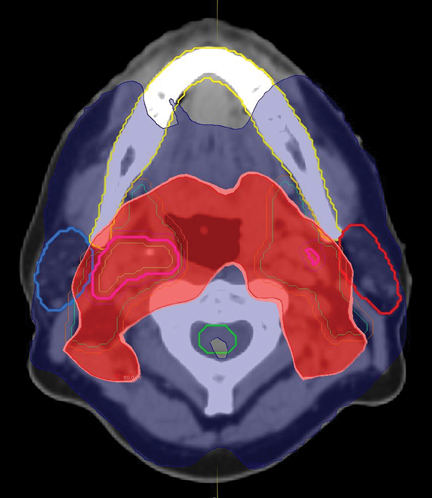
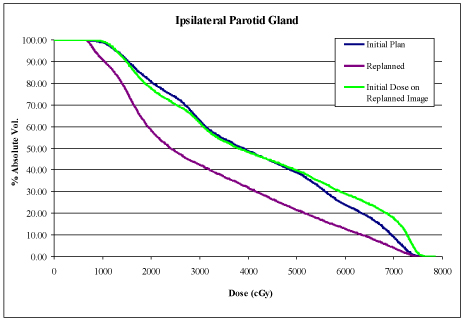
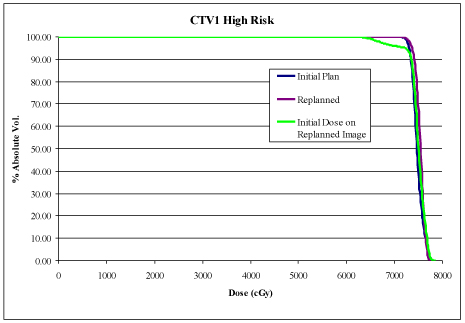
During ART planning, CT imaging demonstrated significant anatomical and geometric changes compared to the initial pretreatment CT simulation images. Overlay of initial treatment contours and dose onto the mid-treatment CT using a rigid registration algorithm (MIM® Software) demonstrated significant anatomical shift in organs at risk (OAR) with associated changes in predicted delivered dose (Figure 1). Automated deformable image registration software using mutual information (MIM® Software) was used to aid in recontouring the OARs, CTV, and planning-target volumes (PTV) onto the mid-treatment CT scan images (Figure1). Final analysis and comparison of the original IMRT and new, ART IMRT plans demonstrated a significant improvement in delivered dose to the OARs, CTVs, and PTVs (Figure 1).
Discussion
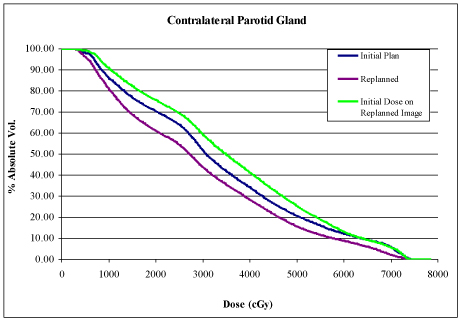
Innovative techniques in radiation oncology have greatly reduced patient toxicity while maintaining, or in some cases improving, outcomes such as local-regional control and overall survival. IMRT has been shown to reduce overall toxicity compared to 3-dimensional radiation therapy (3DRT) in head and neck cancer.1 Additional refinement of IMRT resulted from adaptive replanning to further reduce toxicity related to anatomical change and increased dosing to OARs. Anatomical change during treatment can result in dosimetric variations to OARs and target volumes that can be greatly improved with adaptive replanning.2 Anatomical changes have been correlated with pretreatment nodal disease >4 cm, with the greatest change occurring in the first half of treatment.3 Our patient was determined to be at risk for significant anatomical change based upon the extent of nodal disease and predicted therapeutic response to chemoradiation. He was scheduled upfront, prior to the start of IMRT, for an ART, mid-treatment CT scan. New ROI contours were generated by MIM software using automated deformable image registration of the initial region of interest (ROI) contours onto the mid-treatment CT followed by physician review and editing prior to ART planning.4 Significant anatomical change affecting delivered dose to OARs was observed. Overall, ART planning improved the patient’s therapeutic ratio by significantly reducing the maximum and mean doses to a number of OARs (Figure 2), preventing under dosing to CTVhigh dose (Figure 2), and by delivering dose more conformally to CTV and PTV. ART planning has been shown to have beneficial effects on reducing chronic radiation-induced toxicity, while maintaining comparable local-regional control and survival outcomes.5 Our patient continues to be disease free 2 years post-ART planning with only mild, chronic radiation toxicity.
Conclusion
Our patient presented with HPV-positive, p16-positive, squamous cell carcinoma of the right tonsil with significant bulky nodal disease, placing him at risk for considerable anatomical and geometric changes during a course of definitive IMRT with concurrent cisplatin, 5-FU chemotherapy. If not accounted for, anatomical changes can result in overdosing of OARs and under-dosing of CTV or PTV target volumes, which may result in worse outcomes. The patient underwent ART planning at mid-treatment to account for the associated anatomical change. ART planning based upon mid-treatment CT imaging improved this patient’s therapeutic ratio by reducing delivered dose to OARs while ensuring conformal dose coverage of CTV and PTV target volumes. The patient continues to be disease free 2 years post-ART planning with minimal long-term toxicity.
References
- Nutting CM, Morden JP, Harrington KJ, et al. Parotid-sparing intensity modulated versus conventional radiotherapy in head and neck cancer (PARSPORT): A phase-3 multicentre randomized controlled trial. Lancet Oncol. 2011;12:127-136.
- Ahn PH, Chen CC, Ahn AI, et al. Adaptive planning in intensity-modulated radiation therapy for head and neck cancers: Single-institution experience and clinical implications. Int J Radiat Oncol Biol Phys. 2011;80:677-685.
- Barker JL, Garden AS, Ang KK, et al. Quantification of volumetric and geometric changes occurring during fractionated radiotherapy for head-and-neck cancer using an integrated CT/Linear accelerator system. Int J Radiat Oncol Biol Phys. 2004;59:960-970.
- Tsuji SY, Hwang A, Weinberg V, et al. Dosimetric evaluation of automatic segmentation for adaptive IMRT for head-and-neck cancer. Int J Radiat Oncol Biol Phys. 2010;77:707-714.
- Schwartz DL, Garden AS, Thoma J, et al. Adaptive radiotherapy for head-and-neck cancer: Initial clinical outcomes from a prospective trial. Int J Radiat Oncol Biol Phys. 2012;83:986-993.